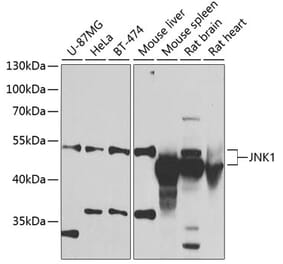
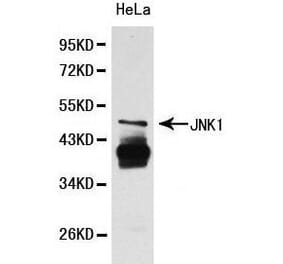
Unconjugated
The process of islet transplantation for treating type 1 diabetes has been limited by the high level of graft failure that may be overcome by locally delivering trophic factors to enhance engraftment. Regenerating islet-derived protein 3 alpha (Reg3α) is a pancreatic secretory protein, which functions as an antimicrobial peptide in control of inflammation and cell proliferation. In this study, to investigate whether Reg3α could improve islet engraftment, a marginal mass of syngeneic islets pretransduced with adenoviruses expressing Reg3α or control EGFP were transplanted under the renal capsule of streptozotocin-induced diabetic mice. Mice receiving islets with elevated Reg3α production exhibited significantly lower blood glucose levels (9.057 ± 0.59 mmol/l vs 13.48 ± 0.35 mmol/l, P < 0.05) and improved glucose-stimulated insulin secretion (1.80 ± 0.17 ng/ml vs 1.16 ± 0.16 ng/ml, P < 0.05) compared with control group. The decline of apoptotic events (0.57% ± 0.15% vs 1.06% ± 0.07%, P < 0.05) and increased beta-cell proliferation (0.70% ± 0.10% vs 0.36% ± 0.14%, P < 0.05) were confirmed in islet grafts overexpressing Reg3α by morphometric analysis. Further experiments showed that Reg3α production dramatically protected cultured islets and pancreatic beta-cells from cytokine-induced apoptosis and the impairment of glucose-stimulated insulin secretion. Moreover, exposure to cytokines led to the activation of MAPKs in pancreatic beta-cells, which was reversed by Reg3α overexpression in contrast to control group. These results strongly suggest that Reg3α could enhance islet engraftments through its cytoprotective effect and advance the therapeutic efficacy of islet transplantation.
OCILRP2 is a typical Type-II transmembrane protein that is selectively expressed in activated T lymphocytes, dendritic cells, and B cells and functions as a novel co-stimulator of T cell activation. However, the signaling pathways underlying OCILRP2 in T cell activation are still not completely understood. In this study, we found that the knockdown of OCILRP2 expression with shRNA or the blockage of its activity by an anti-OCILRP2 antagonist antibody reduced CD3/CD28-costimulated EL4 T cell viability and IL-2 production, inhibit Raf1, MAPK3, and MAPK8 activation, and impair NFAT and NF-κB transcriptional activities. Furthermore, immunoprecipitation results indicated that OCILRP2 could interact with the DAP12 protein, an adaptor containing an intracellular ITAM motif that can transduce signals to induce MAP kinase activation for T cell activation. Our data reveal that after binding with DAP12, OCILRP2 activates the Raf-MAP kinase pathways, resulting in T cell activation.
Cathepsin B (CB), an important proteinase that participates in joint destruction in rheumatoid arthritis (RA), exhibits higher expression in fibroblast-like synoviocyte (FLS) of abnormal proliferative synovial tissues. Whether and how it affects the biological behaviours of RA-FLS, such as migration and invasion, are poorly understood. In the present study, CB expression in synovial tissues of patients with RA and ostearthritis (OA) were measured by quantitative polymerase chain reaction (qPCR) and immunohistochemistry (IHC), respectively. Stable depletion of endogenous CB was achieved by small interfering RNA (siRNA) transfection, and decrease of CB activity was acquired by using its specific inhibitor (CA074Me). The effects of CA074Me and RNA interference (RNAi) treatments on proliferation, migration, invasion, matrix metalloproteinase (MMP)-2/-9 expression, focal adhesion kinase (FAK) activation, and mitogen-activated protein kinases (MAPKs) phosphorylation of FLS were analysed. In RA synovial tissues, CB was expressed at elevated levels compared with OA synovial tissues. CA074Me could inhibit invasion of FLS obtained from RA patients in an ex-vivo invasion model. CA074Me and siRNA treatments suppressed the migration and invasion of FLS, reduced the activity, expression and mRNA level of MMP-2, restrained the activation of FAK and reduced the expression of F-actin. Moreover, CA074Me decreased the phosphorylation of P38 MAPK and c-Jun N-terminal kinase (JNK) in FLS, while siCB treatment reduced the phosphorylation of P38 but not JNK. CB substantially contributes to the invasive phenotype of FLS that leads to joint destruction in RA. This proteinase may show promise as a therapeutic target in inflammatory arthritis.
Currently, synthetic hydroxyapatite nanoparticles (HANPs) are used in nanomedicine fields. The delivery of nanomedicine to the bloodstream exposes the cardiovascular system to a potential threat. However, the possible adverse cardiovascular effects of HANPs remain unclear. Current observations using coculture models of endothelial cells and monocytes with HANPs to mimic the complex physiological functionality of the vascular system demonstrate that monocytes could play an important role in the mechanisms of endothelium dysfunction induced by the exposure to HANPs. Our transmission electron microscopy analysis revealed that both monocytes and endothelial cells could take up HANPs. Moreover, our findings demonstrated that at a subcytotoxic dose, HANPs alone did not cause direct endothelial cell injury, but they did induce an indirect activation of endothelial cells, resulting in increased interleukin-6 production and elevated adhesion molecule expression after coculture with monocytes. The potential proinflammatory effect of HANPs is largely mediated by the release of soluble factors from the activated monocytes, leading to an inflammatory response of the endothelium, which is possibly dependent on p38/c-Jun N-terminal kinase, and nuclear factor-kappa B signaling activation. The use of in vitro monocyte-endothelial cell coculture models for the biocompatibility assessment of HANPs could reveal their potential proinflammatory effects on endothelial cells, suggesting that exposure to HANPs possibly increases the risk of cardiovascular disease.
It has been documented in in vitro studies that zinc oxide nanoparticles (ZnO NPs) are capable of inducing oxidative stress, which plays a crucial role in ZnO NP-mediated apoptosis. However, the underlying molecular mechanism of apoptosis in neurocytes induced by ZnO NP exposure was not fully elucidated. In this study, we investigated the potential mechanisms of apoptosis provoked by ZnO NPs in cultured primary astrocytes by exploring the molecular signaling pathways triggered after ZnO NP exposure. ZnO NP exposure was found to reduce cell viability in MTT assays, increase lactate dehydrogenase (LDH) release, stimulate intracellular reactive oxygen species (ROS) generation, and elicit caspase-3 activation in a dose- and time-dependent manner. Apoptosis occurred after ZnO NP exposure as evidenced by nuclear condensation and poly(ADP-ribose) polymerase-1 (PARP) cleavage. A decrease in mitochondrial membrane potential (MMP) with a concomitant increase in the expression of Bax/Bcl-2 ratio suggested that the mitochondria also mediated the pathway involved in ZnO NP-induced apoptosis. In addition, exposure of the cultured cells to ZnO NPs led to phosphorylation of c-Jun N-terminal kinase (JNK), extracellular signal-related kinase (ERK), and p38 mitogen-activated protein kinase (p38 MAPK). Moreover, JNK inhibitor (SP600125) significantly reduced ZnO NP-induced cleaved PARP and cleaved caspase-3 expression, but not ERK inhibitor (U0126) or p38 MAPK inhibitor (SB203580), indicating that JNK signaling pathway is involved in ZnO NP-induced apoptosis in primary astrocytes.
Hydrogen sulfide (H(2)S) has been proposed as a novel neuromodulator and neuroprotective agent. Cobalt chloride (CoCl(2)) is a well-known hypoxia mimetic agent. We have demonstrated that H(2)S protects against CoCl(2)-induced injuries in PC12 cells. However, whether the members of mitogen-activated protein kinases (MAPK), in particular, extracellular signal-regulated kinase1/2(ERK1/2) and p38MAPK are involved in the neuroprotection of H(2)S against chemical hypoxia-induced injuries of PC12 cells is not understood. We observed that CoCl(2) induced expression of transcriptional factor hypoxia-inducible factor-1 alpha (HIF-1α), decreased cystathionine-β synthase (CBS, a synthase of H(2)S) expression, and increased generation of reactive oxygen species (ROS), leading to injuries of the cells, evidenced by decrease in cell viability, dissipation of mitochondrial membrane potential (MMP) , caspase-3 activation and apoptosis, which were attenuated by pretreatment with NaHS (a donor of H(2)S) or N-acetyl-L cystein (NAC), a ROS scavenger. CoCl(2) rapidly activated ERK1/2, p38MAPK and C-Jun N-terminal kinase (JNK). Inhibition of ERK1/2 or p38MAPK or JNK with kinase inhibitors (U0126 or SB203580 or SP600125, respectively) or genetic silencing of ERK1/2 or p38MAPK by RNAi (Si-ERK1/2 or Si-p38MAPK) significantly prevented CoCl(2)-induced injuries. Pretreatment with NaHS or NAC inhibited not only CoCl(2)-induced ROS production, but also phosphorylation of ERK1/2 and p38MAPK. Thus, we demonstrated that a concurrent activation of ERK1/2, p38MAPK and JNK participates in CoCl(2)-induced injuries and that H(2)S protects PC12 cells against chemical hypoxia-induced injuries by inhibition of ROS-activated ERK1/2 and p38MAPK pathways. Our results suggest that inhibitors of ERK1/2, p38MAPK and JNK or antioxidants may be useful for preventing and treating hypoxia-induced neuronal injury.
PURPOSE:
Oxidative stress is widely implicated in the death of retinal ganglion cells associated with various optic neuropathies. Agonists of the dopamine D(1) receptor have recently been found to be potentially neuroprotective against oxidative stress-induced injury. The goal of this study was to investigate whether SKF83959, a next-generation high-affinity D(1) receptor agonist, could protect retinal ganglion cell 5 (RGC-5) cells from H(2)O(2)-induced damage and the molecular mechanism involved.
METHODS:
We examined expression of the D(1) receptor in RGC-5 cells with reverse-transcription-PCR and immunoblotting and assessed neuroprotection using propidium iodide staining and the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide assay. In addition, we monitored the activation and involvement of members of mitogen-activated protein kinase family, extracellular signal-regulated kinase (ERK), p38 and c-Jun NH(2)-terminal kinase, with western blot and specific inhibitors.
RESULTS:
We found that the D(1) receptor was expressed in RGC-5 cells, but the sequence analysis suggested this cell line is from mouse and not rat origin. SKF83959 exhibited a remarkable neuroprotective effect on H(2)O(2)-damaged RGC-5 cells, which was blocked by the specific D(1) receptor antagonist, SCH23390. ERK and p38 were activated by SKF83959, and pretreatment with their inhibitors U0126 and SB203580, respectively, significantly blunted the SKF83959-induced cytoprotection. However, the specific c-Jun NH(2)-terminal kinase inhibitor, SP600125, had no effect on the SKF83959-induced protection.
CONCLUSIONS:
We conclude that SKF83959 attenuates hydrogen peroxide-induced injury in RGC-5 cells via a mechanism involving activation of the ERK and p38 pathways and the D(1) receptor is a potential molecular target for developing neuroprotective drugs.
BACKGROUND:
Inorganic particles, such as drug carriers or contrast agents, are often introduced into the vascular system. Many key components of the in vivo vascular environment include monocyte-endothelial cell interactions, which are important in the initiation of cardiovascular disease. To better understand the effect of particles on vascular function, the present study explored the direct biological effects of particles on human umbilical vein endothelial cells (HUVECs) and monocytes (THP-1 cells). In addition, the integrated effects and possible mechanism of particle-mediated monocyte-endothelial cell interactions were investigated using a coculture model of HUVECs and THP-1 cells. Fe₃O₄ and SiO₂ particles were chosen as the test materials in the present study.
RESULTS:
The cell viability data from an MTS assay showed that exposure to Fe₃O₄ or SiO₂ particles at concentrations of 200 μg/mL and above significantly decreased the cell viability of HUVECs, but no significant loss in viability was observed in the THP-1 cells. TEM images indicated that with the accumulation of SiO₂ particles in the cells, the size, structure and morphology of the lysosomes significantly changed in HUVECs, whereas the lysosomes of THP-1 cells were not altered. Our results showed that reactive oxygen species (ROS) generation; the production of interleukin (IL)-6, IL-8, monocyte chemoattractant protein 1 (MCP-1), tumor necrosis factor (TNF)-α and IL-1β; and the expression of CD106, CD62E and tissue factor in HUVECs and monocytes were significantly enhanced to a greater degree in the SiO₂-particle-activated cocultures compared with the individual cell types alone. In contrast, exposure to Fe₃O₄ particles had no impact on the activation of monocytes or endothelial cells in monoculture or coculture. Moreover, using treatment with the supernatants of SiO₂-particle-stimulated monocytes or HUVECs, we found that the enhancement of proinflammatory response by SiO₂ particles was not mediated by soluble factors but was dependent on the direct contact between monocytes and HUVECs. Furthermore, flow cytometry analysis showed that SiO₂ particles could markedly increase CD40L expression in HUVECs. Our data also demonstrated that the stimulation of cocultures with SiO₂ particles strongly enhanced c-Jun NH2-terminal kinase (JNK) phosphorylation and NF-κB activation in both HUVECs and THP-1 cells, whereas the phosphorylation of p38 was not affected.
CONCLUSIONS:
Our data demonstrate that SiO₂ particles can significantly augment proinflammatory and procoagulant responses through CD40-CD40L-mediated monocyte-endothelial cell interactions via the JNK/NF-κB pathway, which suggests that cooperative interactions between particles, endothelial cells, and monocytes may trigger or exacerbate cardiovascular dysfunction and disease, such as atherosclerosis and thrombosis. These findings also indicate that the monocyte-endothelial cocultures represent a sensitive in vitro model system to assess the potential toxicity of particles and provide useful information that may help guide the future design and use of inorganic particles in biomedical applications.
The anti-cancer effects of dioscin have been widely reported. However, its effect on laryngeal cancer remains unknown. In the present paper, our results showed that dioscin markedly caused cell apoptosis and DNA damage, increased reactive oxygen species (ROS) level, induced S-phase arrest, and inhibited invasion of human laryngeal cancer HEp-2 and TU212 cells. Mechanism investigation showed that dioscin markedly up-regulated p53 level, and down-regulated cyclin-dependent kinase 2 (CDK2) and Cyclin A levels. In addition, dioscin significantly down-regulated the levels of p-ERK, Bcl-2, up-regulated the levels of p-JNK, p-p38, Bax, cleaved caspase-3/-9, and caused Cytochrome c release. Furthermore, U0126, an ERK1/2 inhibitor, markedly down-regulated Bcl-2 level, up-regulated the levels of Bax, cleaved caspase-3/9, and enhanced Cytochrome c release inducted by dioscin. While, SP600125 (one JNK inhibitor) and SB203580 (one p38 inhibitor) markedly up-regulated Bcl-2 level, down-regulated the levels of Bax, cleaved caspase-3/9, and obviously boosted Cytochrome c release induced by dioscin. Interestingly, dioscin also markedly down-regulated the levels of MMP2 and MMP9 associated with tumor invasion. Taken together, our study indicated that dioscin suppressed laryngeal cancer cells growth via inducting cell-cycle arrest, MAPK-mediated mitochondrial- derived apoptosis and inhibiting tumor invasion, which could be used as one potential candidate for the treatment of laryngeal cancer in the future.
Endotoxin can stimulate inflammatory cytokine release from monocytes/macrophages and result in septic shock. Glycyrrhetinic acid (GA), the main bioactive component of licorice, possesses substantial anti-inflammatory activity. Here, we explored effect of 11-deoxy-18α-glycyrrhetinic acid-30-ethyl ester (DGAEE), a newly synthesized derivative of GA, on septic shock. DGAEE and its main metabolite 11-deoxy-18α-glycyrrhetinic acid (DGA) significantly alleviated septic shock as evidenced by improvements of survival rates, lung histopathological changes and wet/dry ratio in lipopolysaccharide (LPS)/D-galactosamine-stimulated mice, and decreased blood pressure in LPS/D-galactosamine-stimulated rats. The two compounds decreased serum levels of NO, TNF-α, IL-6, IL-1β, and increased the level of IL-10 more potently in mice. In LPS-stimulated RAW 264.7 cells, DGA but not DGAEE showed marked regulation of NO, TNF-α, IL-6 and IL-10 levels, suggesting that DGAEE display anti-shock effect by DGA rather than itself. Moreover, the neutralizing antibody against IL-10 markedly prohibited the inhibitory effect of DGA on the production of cytokines from RAW 264.7 cells, and AS101 (an inhibitor of IL-10 biosynthesis) almost completely reversed the anti-shock effect of DGA in mice. In addition, DGA did not affect activation of NF-κB-p65 and p38 MAPK as well as IκBα degradation, but moderately reduced activation of ERK and JNK, and markedly increased phosphorylation of GSK3β in LPS-stimulated RAW 264.7 cells. LY294002 (an inhibitor of GSK3β phosphorylation) and LiCl (an inhibitor of GSK3β activity) diminished and potentiated increase of IL-10 levels by DGA, respectively. In conclusion, DGAEE alleviates septic shock through DGA in an IL-10-dependent manner, and the mechanism is related to inactivation of GSK3β.
Isoliquiritigenin (ILG), a chalcone from Glycyrrhiza uralensis, has various biological properties. ILG markedly inhibited inflammation, but the effects on the brain inflammation and insulin resistance induced by high-fat diet (HFD) are still unknown, so our study intended to investigate its effect on cognitive dysfunction induced by HFD and the relevant mechanisms. ICR mice were treated with HFD diet for 8 weeks to induce peripheral insulin resistance prior to being intervened with rosiglitazone, ILG (30, 60 mg/kg). 4 weeks later, Morris Water Maze (MWM) was used to assess the learning and memory, the insulin resistance index was measured, and the brain inflammation cytokines (IL-1β, TNF-α) were assessed. Meanwhile, the p-JNK, p-IRS Ser(307) protein expressions in the hippocampus were also detected using the western blot to explore the corresponding mechanisms. Our results suggested that ILG could significantly alleviate the cognitive impairments in the MWM test and attenuate peripheral insulin resistance. The IL-1β, TNF-α levels declined with the administration of ILG, meanwhile the p-IRS Ser(307) expression decreased with the inhibition of p-JNK. In conclusion, ILG could improve the spatial learning and memory lesions induced by HFD via the inhibition of TNF-α/JNK/IRS pathway.
Previous studies have demonstrated that tumor necrosis factor-alpha (TNF-α) in the red nucleus (RN) plays a facilitated role in the development of neuropathic pain. Here, we further investigated the expression changes and roles of the downstream signaling molecules of the red nucleus TNF-α, including nuclear factor-kappa B (NF-κB), extracellular signal-regulated kinase (ERK), p38 mitogen-activated protein kinase (MAPK) and c-Jun N-terminal kinase (JNK), in the initiation and maintenance of neuropathic pain induced by spared nerve injury (SNI). Immunohistochemistry demonstrated that increased expressions of NF-κB, phospho-ERK (p-ERK) and p-p38 MAPK were observed in the RN contralateral (but not ipsilateral) to the nerve injury side at 3 days after SNI compared with sham-operated and normal rats, the up-regulations of NF-κB and p-ERK but not p-p38 MAPK remained at high levels till 14 days later. An elevated expression of p-JNK occurred at 14 days (but not 3 and 7 days) after SNI, which was later than those of NF-κB, p-ERK and p-p38 MAPK. The up-regulations of NF-κB, p-ERK, p-p38 MAPK and p-JNK all could be abolished by microinjection of anti-TNF-α antibody into the RN of rats with SNI. Microinjection of NF-κB inhibitor PDTC, ERK inhibitor PD98059, p38 MAPK inhibitor SB203580 but not JNK inhibitor SP600125 into the RN contralateral to the nerve injury side at 3 days postinjury significantly alleviated SNI-induced mechanical allodynia. In addition, microinjection of PDTC, PD98059 and SP600125 but not SB203580 into the RN at 14 days postinjury significantly alleviated SNI-induced mechanical allodynia. These results suggest that the red nucleus TNF-α produces the algesic effect through activating NF-κB, ERK and p38 MAPK in the early initiation stage but relying on the activation of NF-κB, ERK and JNK in the later maintenance stage of SNI-induced neuropathic pain.
The aim of this study was to explore the intracellular mechanisms underlying the cardiovascular toxicity of air particulate matter (PM) with an aerodynamic diameter of less than 2.5 µm (PM2.5) in a human umbilical vein cell line, EA.hy926. We found that PM2.5 exposure triggered reactive oxygen species (ROS) generation, resulting in a significant decrease in cell viability. Data from Western blots showed that PM2.5 induced phosphorylation of Jun N-terminal kinase (JNK), extracellular signal regulatory kinase (ERK), p38 mitogen-activated protein kinase (MAPK) and protein kinase B (AKT), and activation of nuclear factor kappa B (NF-κB). We further observed a significant increase in expressions of intercellular adhesion molecule-1 (ICAM-1) and vascular adhesion molecule-1 (VCAM-1) in a time- and dose-dependent manner. Moreover, the adhesion of monocytic THP-1 cells to EA.hy926 cells was greatly enhanced in the presence of PM2.5 . However, N-acetylcysteine (NAC), a scavenger of ROS, prevented the increase of ROS generation, attenuated the phosphorylation of the above kinases, and decreased the NF-κB activation as well as the expression of ICAM-1 and VCAM-1. Furthermore, ERK inhibitor (U0126), AKT inhibitor (LY294002) and NF-κB inhibitor (BAY11-7082) significantly down-regulated PM2.5 -induced ICAM-1 and VCAM-1 expression as well as adhesion of THP-1 cells, but not JNK inhibitor (SP600125) and p38 MAPK inhibitor (SB203580), indicating that ERK/AKT/NF-κB is involved in the signaling pathway that leads to PM2.5 -induced ICAM-1 and VCAM-1 expression. These findings suggest PM2.5 -induced ROS may function as signaling molecules triggering ICAM-1 and VCAM-1 expressions through activating the ERK/AKT/NF-κB-dependent pathway, and further promoting monocyte adhesion to endothelial cells.
Vitexin is a major bioactive flavonoid compound derived from the dried leaf of hawthorn (Crataegus pinnatifida), a widely used conventional folk medicine in China. Recent studies have shown that vitexin presents neuroprotective effects in vitro. Whether this protective effect applies to the cerebral ischemia/reperfusion (I/R) injury remains elusive. In the present study, we examined the potential neuroprotective effect of vitexin against cerebral I/R injury and underlying mechanisms. A focal cerebral I/R model in male Kunming mice was induced by middle cerebral artery occlusion (MCAO) for 2 h followed by reperfusion for 22 h. The neurological function and infarct volume were assessed by using Long's five-point scale system and triphenyl-tetrazolium chloride (TTC) staining technique, respectively. Neuronal damage was evaluated by histological staining. Extracellular signal-regulated kinases 1/2 (ERK1/2), c-Jun N-terminal kinases (JNK) and p38 phosphorylation, and apoptosis were measured via Western blot at 24 h after reperfusion. As a result, systemic vitexin treatment significantly reduced neurological deficit, cerebral infarct volume and neuronal damage when compared with the I/R group. Western blot analyses revealed that vitexin markedly upregulated p-ERK1/2 and downregulated p-JNK and p-p38. Meanwhile, vitexin increased Bcl-2 expression and suppressed the overexpression of Bax in the I/R injury mice. In conclusion, the results indicate that vitexin protects brain against cerebral I/R injury, and this effect may be regulated by mitogen-activated protein kinase (MAPK) and apoptosis signaling pathways.
Urocortin (UCN) has exhibited antiinflammatory and neuroprotective effects on intracerebral hemorrhage (ICH). However, the underlying mechanisms are still not clear. Therefore, this study was aimed to investigate effects of UCN1 on ICH in vitro and in vivo and further explore the possible mechanism. ICH was induced by an infusion of autologous blood into the unilateral striatum of anesthetized male Sprague-Dawley rats. The rats were randomly divided into three groups (8 rats per group): sham ICH control group, ICH saline group and ICH UCN1 group. UCN1 was infused into the lateral ventricle after 1h post-ICH. Neurological deficits were evaluated by modified neurological severity score (mNSS). Brain edema was assessed using the dry/wet method. The neurological cell metabolic activity of N2a and SH-SY5Y was detected by CCK-8. The level of VEGF, JNK and p38 were determined by enzyme-linked immunosorbent assay and western blot. Post-treatment with UCN1 could improve neurological deficits and reduce brain edema. Moreover, UCN1 could increase the metabolic activity of neuron cells dose-dependently and these effects could be abolished by corticotropin-releasing factor receptor 2 (CRFR2) antagonist anti-Svg-30. Furthermore, the level of VEGF, JNK and p38 were up-regulated by post-treatment with UCN1 via CRFR2. The protective effects of UCN1 against ICH are possibly mediated by activating the phosphorylation of JNK and p38 and further increasing the level of VEGF via CRFR2.
Obovatol, a compound isolated from the bark cortex of Magnolia officinalis (cortex Magnoliae officinalis; M. officinalis), has been studied for use in the treatment of solid cancers. However, the mechanisms of action and the effects of obovatol against acute myeloid leukemia (AML) remain unclear and require further investigation. Therefore, this study was conducted using a human AML cell line (MM6). Obovatol increased pro-apoptotic (Bax) and decreased anti-apoptotic (Bcl-2) protein expression, resulting in caspase-3 and caspase-9 activation measured by caspase-Glo 3/7 assay. Furthermore, obovatol activated the mitogen-activated protein kinase (MAPK) signaling pathway [c-Jun N-terminal kinase (JNK), extracellular signal-regulated kinase (ERK) and p38] and inhibited the activation of the nuclear factor-κB (NF-κB) signaling pathway analyzed by western blot analysis. Taken together, these findings provide evidence that obovatol inhibits cell proliferation in AML and induces apoptosis through the activation of the MAPK pathway in addition to the intrinsic apoptotic pathway. In addition, obovatol suppressed the expression of mixed-lineage leukemia (MLL) target genes by inhibiting the activation of the NF-κB pathway. Therefore, these results suggest that obovatol may have potential for use in the treatment of leukemia.
Mitofusin 2 (Mfn2) is a dynamin-like protein anchored in the outer mitochondrial membrane that plays a crucial role in ensuring optimal mitochondrial morphological homeostasis. It has been shown that reduced expression of Mfn2 is associated with insulin resistance, but the mechanism is still unclear. We investigated whether Mfn2 deficiency leads to impaired insulin sensitivity via elevated oxidative stress. L6 skeletal muscle cells were treated with palmitate and Mfn2 expression was repressed by transfection with antisense Mfn2. Levels of antioxidant enzymes, reactive oxygen species (ROS), the phosphorylation of c-Jun N-terminal Kinase (JNK) and nuclear factor-κB (NF-κB) and the mitochondrial membrane potential (Δψm) were measured. The results showed palmitate-induced insulin resistance of skeletal muscle cells was accompanied by Mfn2 repression. Meanwhile, the cells had decreased Δψm and activity of antioxidant enzymes which could increase production of ROS, phosphorylation of JNK and NF-κB. When Mfn2 was up-regulated in palmitate-treated cells, oxidative stress and insulin resistance was alleviated. Furthermore, knock-down of Mfn2 in control cells enhanced oxidative stress. Mfn2 deficiency led to increased superoxide concentration and activation of JNK as well as NF-κB associated with insulin signaling. In conclusion, Mfn2 is a potent repressor for oxidative stress and regulation of Mfn2 expression may prove to be a potential method to circumvent insulin resistance.
The effect of the total saponins from Rosa laevigata Michx fruit (RLTS) against acetaminophen (APAP)-induced liver damage in mice was evaluated in the present paper. The results showed that RLTS markedly improved the levels of liver SOD, CAT, GSH, GSH-Px, MDA, NO and iNOS, and the activities of serum ALT and AST caused by APAP. Further research confirmed that RLTS prevented fragmentation of DNA and mitochondrial ultrastructural alterations based on TdT-mediated dUTP nick end labeling (TUNEL) and transmission electron microscopy (TEM) assays. In addition, RLTS decreased the gene or protein expressions of cytochrome P450 (CYP2E1), pro-inflammatory mediators (IL-1β, IL-4, IL-6, TNF-α, iNOS, Bax, HMGB-1 and COX-2), pro-inflammatory transcription factors (NF-κB and AP-1), pro-apoptotic proteins (cytochrome C, p53, caspase-3, caspase-9, p-JNK, p-p38 and p-ERK), and increased the protein expressions of Bcl-2 and Bcl-xL. Moreover, the gene expression of IL-10, and the proteins including LC3, Beclin-1 and Atg5 induced by APAP were even more augmented by the extract. These results demonstrate that RLTS has hepatoprotective effects through antioxidative action, induction of autophagy, and suppression of inflammation and apoptosis, and could be developed as a potential candidate to treat APAP-induced liver damage in the future.
Exposure to elevated levels of fluoride can cause a variety of adverse effects in fish. Previously we showed that fluoride causes injuries and apoptosis in the gills of Cyprinus carpio. In this study, the effects of fluoride on caspase-3 activity and on accumulation of proteins in the MAPKs pathways were evaluated using Western blotting and immunohistochemistry methods in vivo and in vitro. In vivo experiments showed that the caspase-3 activity increased with fluoride exposure level in a dose-dependent pattern Western blotting and immunohistochemistry results indicated that ERK relative activation tended to decrease as a function of fluoride exposure concentration. In contrast, relative activation of JNK increased with fluoride exposure level. Fluoride exposure did not appear to affect p38 activation. Furthermore, pretreatment of branchial cells with MAPK-specific inhibitors effectively prevented JNK induction and ERK inhibition, respectively, as well as reversed caspase-3 activity in fluoride-treated branchial cells. Our results indicate that activation of JNK and inactivation of ERK were caused by increased ROS and decreased antioxidant capacity in the gills of chronically exposed C. carpio described previously, which eventually caused the observed apoptosis in the fluoride-exposed gills and cells in C. carpio. JNK activation and ERK inactivation mechanism play a crucial role in gill impairment induced by chronic fluorosis. These findings contribute to a better understanding of the initial molecular and cellular events in the gill of fish chronically exposed to fluoride.
The mechanism of blue light-induced retinal ganglion cell (RGC) injury is poorly understood. In this study, we established a patented light-emitting diode-based system to study the effects of long-term blue light exposure under culture conditions on RGC-5 cells. Long-term blue light exposure significantly reduced cell viability in a time-dependent manner and induced apoptosis and necrosis in RGC-5 cells. Long-term blue light exposure marked an increase in the expression of Bax and active Caspase-3 (p17), which was accompanied by Bcl-2 down-regulation, and displayed features of the mitochondria-dependent apoptosis pathway. Blue light exposure also increased the generation of reactive oxygen species (ROS), and was a strong inducer of ROS-sensitive protein nuclear factor erythroid 2-related factor 2 (Nrf2) and heme oxygenase-1 (HO-1) expression. Moreover, blue light exposure constitutively activated p38 mitogen-activated protein kinases and c-Jun NH2-terminal kinase (JNK), as well as induced the phosphorylation of extracellular signal-regulated kinase in the early phase, in blue light-exposed RGC-5 cells. The protein expression of c-jun and c-fos was further enhanced after RGC-5 cells were exposed to blue light. Taken together, these findings indicated that blue light induced RGC-5 cell line death in dependence upon exposure duration. The potential mechanisms for this phenomenon might be via activated mitochondria-dependent apoptosis, increased ROS production and protein expressions of Nrf2 and HO-1, and activated JNK/p38 MAPK signaling pathways.
Dentin, the predominant mineralized tissue of the tooth, comprises an extracellular matrix of collagen and a heterogeneous mixture of non-collagenous components, many of which have cellular signaling properties. These properties may be important in signaling stem cell involvement in tissue regeneration following injury and the present study investigates their morphogenic effects on differentiation of Bone Marrow Stromal Stem Cells (BMMSCs) in vitro. Non-collagenous dentin matrix proteins (DMPs) were isolated from healthy human teeth and their effects on BMMSCs behavior examined during in vitro culture. In vitro, DMPs enhanced alkaline phosphatase activity and mineralization in BMMSCs cultures as well as increasing the expression of dentinogenic and osteogenic differentiation markers (including runt-related transcription factor 2, osterix, bone sialoprotein, dentin sialophosphoprotein and osteocalcin) at both transcript and protein levels, with 10 μg/mL DMPs being the optimal stimulatory concentration. Expression of phosphor-ERK/phosphor-P38 in BMMSCs was up-regulated by DMPs and, in the presence of the ERK1/2- and p38-specific inhibitors, the differentiation of BMMSCs was inhibited. These data indicate that DMPs promote the dentinogenic/osteogenic differentiation of BMMSCs via the ERK/p38 MAPK pathways.
The present study was to investigate the effects and possible mechanisms of the total saponins from Dioscorea nipponica Makino (TSDN) against CCl₄-induced hepato-toxicity in mice. The mice were orally administrated with TSDN for seven days and then given CCl₄ (0.3%, 10 ml/kg i.p.). The results showed that TSDN significantly attenuated the activities of ALT and AST, consistent with hematoxylin-eosin staining. The ALP levels and relative liver weight were significantly decreased by TSDN compared with model group. Moreover, TSDN dramatically decreased MDA, iNOS and NO levels, while the levels of GSH, GSH-Px and SOD were increased. Further investigations showed that TSDN inhibited CCl₄-induced metabolic activation and CYP2E1 expression, down-regulated the levels of MAPKs phosphorylation, NF-κB, HMGB1, COX-2 as well as effectively suppressed the expressions of Caspase-3, Caspase-9, PARP and Bak. Quantitative real-time PCR assay demonstrated that TSDN obviously decreased the gene expressions of TNF-a, IL-1β, IL-6, IL-10, Fas, FasL, Bax as well as modulated Bcl-2 mRNA level. This is the first time to report the protective actions of the TSDN against CCl₄-induced liver damage in mice through suppression of inflammation and apoptosis. This natural product should be developed as a new drug for treatment of liver injury in future.
Apoptosis of microvascular endothelial cells plays a crucial role in the progression of various lung diseases and triggers microcirculatory disorder and organ dysfunction. LPS, an outer membrane component of Gram-negative bacteria, is one of the major virulence factors for lung diseases. Recent studies have shown that the Rho/Rho kinase (ROCK) pathway plays an important role in the regulation of apoptosis, inflammatory cell migration and chemokine production in various cell types and animal models. We therefore undertake this study to investigate the inhibitory effect of fasudil, a potent and selective inhibitor of ROCK, on LPS-induced apoptosis of rat pulmonary microvascular endothelial cells (PMVECs). The results suggested that fasudil effectively prevented LPS-induced injury of rat PMVECs, as determined by MTT assay, LDH activity assay, apoptosis and western blot analysis of apoptosis-related proteins Bcl-2 and Bax. Furthermore, the mechanisms underlying the protective effect were evaluated. We found that LPS-induced MYPT-1 phosphorylation was markedly suppressed by fasudil. Moreover, fasudil pretreatment obviously inhibited the activation of JNK and p38 MAPKs induced by LPS, whereas that of ERK1/2 was not affected by fasudil. In addition, inhibiting the JNK and p38 pathways by SP600125 and SB203580 respectively attenuated the LPS-induced apoptosis and regulated the expression of apoptosis-related proteins Bcl-2 and Bax. Taken together, these results demonstrate that fasudil exerts an anti-apoptotic effect in rat PMVECs, which is mediated by the inhibition of Rho/ROCK and its downstream JNK and p38 MAPKs.
The c-Jun N-terminal kinase (JNK) is well known to play an important role in cell death signaling of the p75 neurotrophin receptor. However, little has been studied about a role of JNK in the signaling pathways of the tropomyosin-related kinase A (TrkA) neurotrophin receptor. In this study, we investigated JNK inhibitor SP600125-controlled TrkA-dependent targets by proteomic analysis to better understand an involvement of JNK in TrkA-mediated signaling pathways. PDQuest image analysis and protein identification results showed that hnRNP C1/C2, α-tubulin, β-tubulin homolog, actin homolog, and eIF-5A-1 protein spots were upregulated by ectopic expression of TrkA, whereas α-enolase, peroxiredoxin-6, PROS-27, HSP70, PP1-gamma, and PDH E1-alpha were downregulated by TrkA, and these TrkA-dependent upregulation and downregulation were significantly suppressed by SP600125. Notably, TrkA largely affected certain PTM(s) but not total protein amounts of the SP600125-controlled TrkA-dependent targets. Moreover, SP600125 strongly suppressed TrkA-mediated tyrosine phosphorylation signaling pathways as well as JNK signaling, indicating that SP600125 could function as a TrkA inhibitor. Taken together, our results suggest that TrkA could play an important role in the cytoskeleton, cell death, cellular processing, and glucose metabolism through activation or inactivation of the SP600125-controlled TrkA-dependent targets.
Multiple studies have indicated that selective cyclooxygenase-2 (COX-2) inhibitors possess clinically chemopreventive and preclinically anticancer activities. Their long-term use, however, may be limited by the cardiovascular toxicity. This study tried to investigate whether an apple oligogalactan (AOG) could enhance the growth inhibitory effect of celecoxib on colorectal cancer. Caco-2 and HT-29 cell lines were exposed to different concentrations of AOG (0-1 g/L), celecoxib (0-25 μmol/L), and their combination. COX-2 levels were assessed by reverse transcription PCR and Western blot. COX-2 activity was evaluated by measuring prostaglandin E2 concentration. A colitis-associated colorectal cancer (CACC) mouse model was used to determine the effect of the combination in vivo. AOG (0.1-0.5 g/L) could potentiate the inhibitory effect of physiologic doses of celecoxib (5 μmol/L) on cell growth and decrease COX-2 expressions both at RNA and protein levels. In vivo, the combination (2.5% AOG plus 0.04% celecoxib, w/w) prevented against CACC in mice effectively. Our data indicate that AOG could potentiate the growth inhibitory effect of celecoxib on colorectal cancer both in vitro and in vivo through influencing the expression and function of COX-2 and phosphorylation of MAPKs, which suggests a new possible combinatorial strategy in colorectal cancer therapy.
Previous studies have demonstrated that tumor necrosis factor-alpha (TNF-α) in the red nucleus (RN) plays facilitated roles in the development of abnormal pain. Here, the roles of nuclear factor-kappa B (NF-κB), extracellular signal-regulated kinase (ERK), p38 mitogen-activated protein kinase (MAPK) and c-Jun N-terminal kinase (JNK) in TNF-α-evoked mechanical allodynia were investigated. Repeated microinjection of recombinant rat TNF-α (20 ng daily for 3 days) into the unilateral RN of normal rats induced a significant mechanical allodynia in the contralateral but not ipsilateral hind paw at the fifth day and disappeared 24h later. Re-injection of a single bolus of 20 ng TNF-α into the same RN reproduced this mechanical allodynia within 30 min, which was used as a pain model for further experiments. Immunohistochemistry demonstrated that NF-κB, phospho-ERK (p-ERK) and p-p38 MAPK in the RN were significantly up-regulated at 1h after TNF-α microinjection, the up-regulations of NF-κB and p-ERK but not p-p38 MAPK remained at high levels till 4h later. A significant up-regulation of p-JNK occurred at 4h (but not 1h) after TNF-α microinjection, which was later than those of NF-κB, p-ERK and p-p38 MAPK. Pre-treatment with NF-κB inhibitor PDTC, ERK inhibitor PD98059 or p38 MAPK inhibitor SB203580 at 30 min before TNF-α microinjected into the RN completely prevented TNF-α-evoked mechanical allodynia. Pre-treatment with JNK inhibitor SP600125 did not prevent but reversed TNF-α-evoked mechanical allodynia during the subsequent detection time. Post-treatment with PDTC, PD98059 or SP600125 (but not SB203580) at 4h after TNF-α microinjected into the RN significantly reversed TNF-α-evoked mechanical allodynia. These results further prove that TNF-α in the RN plays a crucial role in the development of abnormal pain, and the algesic effect of TNF-α is initiated through activating NF-κB, ERK and p38 MAPK. The later maintenance of TNF-α-evoked mechanical allodynia mainly relies on the activation of NF-κB, ERK and JNK, but not p38 MAPK.
The neuroprotective effect and mechanism of the flavonoid-rich extract (FRE) from Rosa laevigata Michx fruit on cerebral ischemia-reperfusion (I/R) injury were investigated. The contents of flavonoids, saponins and tannin were determined, and ten chemicals including chlorogenic acid, 4-hydroxy-3-methoxybenzoic acid, apigenin, luteolin, kaempferol, querce-tin, kaempferide-3-O-glucoside, quercetin-3-rhamnoside, rutin and isorhamnetin-3-O-β-rutinoside from the crude extract were separated. Oral administration of FRE obviously improved the survival rate and prevented I/R-induced disability and histological damage. Further works showed that the natural product had excellent antioxidant activity, significantly decreased DNA fragmentation, up-regulated the expression of Bcl-2, and down-regulated the expressions of p53, Apaf1, Fas, FasL, Bax, Bid, cytochrome C and active Caspase-3, -9 and -8. Moreover, the FRE decreased the expressions of NF-κB, iNOS, MMP-9, COX-2, TNF-α, IL-1β, IL-4, IL-6, and down-regulated the levels of p-JNK, p-ERK and p-p38 in MAPK pathways. Therefore, the flavonoid-rich extract from R. laevigata Michx fruit has the potential actions for treatment of ischemic stroke due to its anti-oxidant, anti-apoptosis and anti-inflammatory properties.
Urocortin (UCN1) is a member of corticotrophin-releasing factor (CRF) family, which has been proven to participate in inflammation. Previous work showed that dihydrotestosterone (DHT) could promote the inflammatory process. Little is known about the effect of DHT on UCN1 expression. The aim of our study is to investigate the effects and underlying mechanisms of DHT on endothelial UCN1 expression in the absence and presence of induced inflammation. Therefore, we tested the alterations of endothelial UCN1 expression treated with DHT in the presence or absence of lipopolysaccharide (LPS). Our data showed that DHT alone decreased UCN1 levels, which were attenuated in the presence of the androgen receptor (AR) antagonist flutamide. Conversely, in the presence of LPS, DHT augmented the LPS-induced increase in UCN1 expression, which was, interestingly, not affected by flutamide. When cells were treated with DHT alone, AR was upregulated and translocated into the nuclei, which might repress UCN1 expression via a potential androgen-responsive element found in human CRF family promoter. In the presence of LPS, DHT did not influence AR expression and location while it increased toll-like receptor 4 expression and activation, which was not altered by flutamide. DHT enhanced LPS-induced p38MAPK, ERK1/2, and nuclear factor κB pathway activation, which may contribute to the elevated expression of UCN1. These data suggest that DHT differentially influences UCN1 levels under normal and inflammatory conditions in human umbilical vein endothelial cells, which involves AR-dependent and -independent mechanisms respectively.
Metastasis induced by chronic inflammation has been considered as a major challenge during cancer therapy. Epithelial-mesenchymal transition (EMT) is associated with cancer invasion and metastasis promoted by pro-inflammatory cytokine TNFα. However, the mechanisms underlying TNFα-induced EMT in prostate cancer cells is not entirely clear. Here we showed that EMT induced by longstanding stimulation with TNFα in prostate cancer PC3 cells is mediated by up-regulation of the transcriptional repressor Snail. TNFα-mediated EMT was characterized by acquiring mesenchymal fusiform morphology, increasing the expression of Vimentin and decreasing the expression of E-cadherin. Exposure to TNFα increased the expression of transcription factor Snail via post-transcriptional regulation process and induced Snail nuclear localization in PC3 cells. Moreover, overexpressed Snail in PC3 cells induced EMT. Conversely, suppressing Snail expression abrogated TNFα-induced EMT, suggesting that Snail plays a crucial role in TNFα-induced EMT in prostate cancer cells. Finally, we showed that TNFα time-dependently activated NF-κB, AKT, ERK, p38 MAPK signaling pathways, and elevated Snail stability by activating AKT pathway that subsequently inhibited GSK-3β activity. Taken together, these results reveal that stabilization of Snail via AKT/GSK-3β signaling pathway is required for TNFα-induced EMT in prostate cancer cells. This study offers a better understanding of TNFα-induced metastasis and provides an effective therapeutic strategy for prostate cancer treatment.
Tumor necrosis factor-related apoptosis-inducing ligand (TRAIL) is a promising candidate for the treatment of cancer, because it preferentially induces apoptosis in numerous cancer cells with little or no effect on normal cells. 5,7-Dihydroxyflavone is a dietary flavonoid commonly found in many plants. Here we show that the combined treatment with 5,7-dihydroxyflavone and TRAIL at subtoxic concentrations induced strong apoptotic response in human hepatocarcinoma HepG2 cells, acute leukemia Jurkat T cells, and cervical carcinoma HeLa cells. We further investigated the mechanisms by which 5,7-dihydroxyflavone augments TRAIL-induced apoptosis in HepG2 cells. 5,7-Dihydroxyflavone up-regulated the expression of pro-apoptotic protein Bax, attenuated the expression of anti-apoptotic proteins Bcl-2, Mcl-1, and IAPs, and reduced the phosphorylation levels of Akt and STAT3, weakening the anti-apoptotic signals thus facilitating the process of apoptosis. Moreover, 5,7-dihydroxyflavone and TRAIL were well tolerated in mice, and the combination of 5,7-dihydroxyflavone and TRAIL reduced tumor burden in vivo in a HepG2 tumor xenograft model. Interestingly, 5,7-dihydroxyflavone-mediated sensitization to TRAIL-induced cell death was not observed in normal human hepatocytes L-O2. These results suggest that the 5,7-dihydroxyflavone in combination with TRAIL might be used for cancer prevention and/or therapy.
Formyl peptide receptor 1 (FPR1) plays an important role in the rapid progression of glioblastoma and has been considered as a molecular target for the treatment. Previously, we have shown that oligomer proanthocyanidins (F2, degree of polymerization 2-15), isolated from grape seeds, inhibited FPR1-mediated chemotaxis of U-87 glioblastoma cells. In the present study, we investigated the capacity of F2 to interact with FPR1. The cross attenuation of chemotaxis revealed that F2 shared FPR1 with formyl-methionyl-leucyl-phenylalanine (fMLF), which is a prototype agonist of FPR1. F2 was chemotactic for U-87 cells, and the chemotactic response was abolished when FPR1 gene was silenced or FPR1 was competitively occupied. We further show that F2 specifically blocked the binding of fluorescent agonist to FPR1. Interestingly, F2 exhibited the characteristic of a partial agonist for FPR1, as shown by its capacity to activate FPR1-mediated PI3K-PKC-MAPK pathways. Meanwhile, F2 also attenuated fMLF-triggered MAPK activation, suggesting that F2 could antagonize the effect of an agonist. Furthermore, F2 abolished the invasion of U-87 cells induced by fMLF. Thus, we have identified F2 as a novel, partial agonist for FPR1, which may be useful for glioblastoma therapy.
Tropomyosin-related kinase A (TrkA) is a receptor-type protein tyrosine kinase and exploits pleiotypic roles via nerve growth factor (NGF)-dependent or NGF-independent mechanisms in various cell types. Here, we showed that the inhibition of TrkA activity by GW441756 resulted in the suppression of tyrosine phosphorylation of cellular proteins including extracellular signal-regulated protein kinase (ERK) and c-Jun N-terminal kinase (JNK). To find novel targets associated with TrkA-mediated tyrosine phosphorylation signaling pathways, we investigated GW441756 effects on TrkA-dependent targets in SK-N-MC neuroblastoma cells by proteomic analysis. The major TrkA-dependent protein spots controlled by GW441756 were determined by PDQuest image analysis, identified by MALDI-TOF MS and MALDI-TOF/TOF MS/MS, and verified by 2DE/Western blot analysis. Thus, we found that most of the identified protein spots were modified forms in a normal condition, and their modifications were regulated by TrkA activity. Especially, our results demonstrated that the modifications of α-tubulin and heterogeneous nuclear ribonucleoproteins C1/C2 (hnRNP C1/C2) were significantly upregulated by TrkA, whereas α-enolase modification was downregulated by TrkA, and it was suppressed by GW441756, indicating that TrkA activity is required for their modifications. Taken together, we suggest here that the major novel TrkA-dependent targets such as α-tubulin, hnRNP C1/C2, and α-enolase could play an essential role in TrkA-mediated tyrosine phosphorylation signaling pathways via regulation of their posttranslational modifications.
The adhesion of monocytes to activated vascular endothelial cells is a critical event in the initiation of atherosclerosis. Adhesion is mediated by oxidized low-density lipoprotein (ox-LDL) which up-regulates inflammatory markers on endothelial cells. Here we report that (±) 7, 8-dihydroxy-3-methyl-isochromanone-4 (XJP-1), an inhibitor of ox-LDL-induced adhesion of monocytes to endothelial cells blocks cellular functions which are associated with adhesion. We show that XJP-1 down-regulates ox-LDL-induced over-expression of adhesion molecules (ICAM-1 and VCAM-1) in a dose-dependent manner in human umbilical vein endothelial cells (HUVECs), attenuates ox-LDL-induced up-regulation of low-density lipoprotein receptor (LOX)-1, decreases generation of reactive oxygen species (ROS), blocks translocation of nuclear factor-kappa B (NF-κB) activity, and prevents activation of c-Jun N-terminal kinase (JNK)/p38 pathways in endothelial cells. These findings suggest that XJP-1 may attenuate ox-LDL-induced endothelial adhesion of monocytes by blocking expression of adhesion molecules through suppressing ROS/NF-κB, JNK and p38 pathways.
It is well known that reactive oxygen species (ROS) plays a role in the pathogenesis of insulin resistance which is the hallmark of type 2 diabetes. However, it is still needed to clarify the mechanism underlying insulin resistance. Glucose oxidase (GOD) is an oxi-reductase catalyzing the conversion of glucose to glucolactone, which is further converted to glucuronic acid and H(2)O(2). The present study was designed to establish a rat model of insulin resistance using GOD and to investigate possible mechanisms. The results showed that three days administration of GOD could significantly increase fasting blood glucose, resulting in impaired glucose and insulin tolerance. Moreover, GOD disrupted insulin signaling both in rats and in hepatocytes, as evidenced by decreased phosphorylation of insulin-stimulated Akt, GSK3 and FOXO1α. Furthermore, GOD administration decreased the expression of PPARγ, alterated the phosphorylation of MAPKs, including p38, ERK and JNK, increased the expression of GRP78 and reduced the expression of PGC-1α and decreased the activities of ATPase and respiratory complexes, all of which have been reported to contribute to insulin resistance. Redox balance was evaluated by detecting the expression of antioxidant defenses and ROS generation. After the treatment with GOD, nuclear factorerythroid 2 p45-related factor 2 (Nrf2)-regulated antioxidant enzymes were damaged and ROS production increased significantly. N-acetyl-L-cysteine (NAC), a potent antioxidant, could notably inhibit these effects of GOD. Although further studies are needed to investigate the clear mechanism, these data also support the conclusion that, if not the most early event, ROS generation is the most important event that plays a central role in the pathogenesis of insulin resistance. Overall, our study established an insulin resistant animal model induced by GOD, elucidated the importance of ROS in pathogenesis of insulin resistance and provided the clue for further studies on the underlying mechanisms.
Our previous research data showed that type II cGMP-dependent protein kinase (PKGII) inhibited EGF-induced MAPK/ERK-mediated signal transduction through blocking the phosphorylation of EGFR caused by EGF. Since EGFR also mediates other MAPK-mediated signal transduction pathways, this study was designed to investigate whether PKGII inhibits EGF-induced MAPK/c-Jun N-terminal kinase (JNK) signal transduction. MCF-7 human breast cancer cells were infected with adenoviral constructs encoding the cDNA of PKGII (pAd-PKGII) to increase the expression of PKGII and treated with 8-pCPT-cGMP to activate the enzyme. Western blotting was applied to detect the phosphorylation/activation of EGFR, JNK, MKK7 and c-Jun. The Pull-down method was used to detect the activation of Ras protein. Co-IP was used to analyze the binding between Grb2 and Sos1. TUNEL staining was used to detect the apoptosis of MCF-7 cells. The results showed that EGF treatment increased the phosphorylation of EGFR, the binding between Grb2 and Sos1, the activation of Ras, and the phosphorylation/activation of MKK7, JNK and c-Jun, but decreased the apoptosis of the cells. Increase of PKGII activity through infection with pAd-PKGII and stimulation with 8-pCPT-cGMP efficiently reversed the above changes caused by EGF. The results suggest that PKGII also inhibits EGF-induced MAPK/JNK-mediated signal transduction and further confirmed that PKGII can block the activation of EGFR.
It has been demonstrated that the water channel protein aquaporin-4 (AQP4) plays an important role in astrocyte plasticity in response to a variety of injuries or stimuli. However, the potential role of AQP4 in astrocyte response to β-amyloid (Aβ) has not been studied. The purpose of this study was to investigate this issue. Compared to media control, the lower concentrations of Aβ(1-42) (0.1-1 μM) increased AQP4 expression in cultured mouse cortical astrocytes, while the higher concentrations of Aβ(1-42) (10 μM) decreased AQP4 expression. AQP4 gene knockout reduced Aβ(1-42)-induced astrocyte activation and apoptosis, which was associated with a reduction in the uptake of Aβ via decreased upregulation of low-density lipoprotein receptor related protein-1. Moreover, time-course and levels of Aβ(1-42)-induced mitogen-activated protein kinase phosphorylation were altered in AQP4 null astrocytes compared with wild-type controls. Our data reveal a novel role of AQP4 in the uptake of Aβ by astrocytes, indicating that AQP4 is a molecular target for Alzheimer's disease.
Insulin-like growth factor 1 (IGF-1) is a potent mitogenic protein which can enhance the osteogenic differentiation of periodontal ligament (PDL) fibroblasts. However, it remains unclear whether IGF-1 can stimulate the osteogenic differentiation and osteogenesis of human periodontal ligament stem cells (PDLSCs). In this study, STRO-1(+) PDLSCs were isolated from human PDL tissues, treated with IGF-1, and their osteogenic capacity was investigated in vitro and in vivo. Dimethyl-thiazol-diphenyl tetrazolium bromide assay and flow cytometry results demonstrated that 10-200 ng/mL IGF-1 can stimulate the proliferation ability of PDLSCs and 100 ng/mL is the optimal concentration. Exogenous IGF-1 can modify the ultrastructure, enhance the alkaline phosphatase activity, the mineralization ability of PDLSCs, and increase the expression of osteogenic markers (runt-related transcription factor 2, osterix, and osteocalcin) at mRNA and protein levels. In vivo transplantation illustrated that IGF-1 treated implants generated more mineralized tissues, and presented stronger expression of RUNX2, OSX, and OCN than control group. Moreover, the expression of phosphor-ERK and phosphor-JNK in these stem cells was upregulated by IGF-1, indicating that MAPK signaling pathway was activated during the osteogenic differentiation of PDLSCs mediated by IGF-1. Together, the results showed that IGF-1 can promote the osteogenic differentiation and osteogenesis of STRO-1(+) PDLSCs via ERK and JNK MAPK pathway, suggesting that IGF-1 is a potent agent for stem cell-based periodontal tissue regeneration.
Arsenic trioxide (As₂O₃) has potential anti-cancer activity against a wide range of carcinomas via apoptosis induction or oncoprotein degradation. The mechanisms involved are not fully elucidated. Here, we demonstrated that As₂O₃ induced-apoptosis in HeLa and MCF-7 cancer cells was in part triggered by tubulin polymerization. High expression of JWA promoted tubulin polymerization and increased the sensitivity of the cancer cells to As₂O₃. The activation of the p38 MAPK (mitogen-activated protein kinases) signaling pathway was found to contribute to JWA-promoted tubulin polymerization. Our results suggest that JWA may serve as an effective enhancer of microtubule-targeted As₂O₃ anti-cancer therapy.
We examined the effects of anti-six-transmembrane epithelial antigen of the prostate-4 (STEAP4) antibodies on glucose transport in mature adipocytes and determined the mechanism of insulin resistance in obesity. Western blotting was performed to determine STEAP4 expression, to assess translocation of insulin-sensitive glucose transporter 4 (GLUT4), and to measure phosphorylation and total protein content of insulin-signaling proteins. Confocal laser microscopy and flow cytometry were used to detect intracellular reactive oxygen species (ROS) and fluctuations in mitochondrial membrane potential (ΔΨ). ATP production was measured by using a luciferase-based luminescence assay kit. After the application of anti-STEAP4 antibodies at 0.002 mg/mL, adipocytes exhibited reduced insulin-stimulated glucose transport by attenuating the phosphorylation of IRS-1, PI3K (p85), and Akt. The antibodies also potentially increase the level of ROS and decrease cellular ATP production and ΔΨ. In conclusion, (i) STEAP4 regulates the function of IRS-1, PI3K, and Akt and decreases insulin-induced GLUT4 translocation and glucose uptake; (ii) ROS-related mitochondrial dysfunction may be related to a reduced IRS-1 correlation with the PI3K signaling pathway, leading to insulin resistance. These observations highlight the potential role of STEAP4 in glucose homeostasis and possibly in the pathophysiology of type 2 diabetes related to obesity and may provide new insights into the mechanisms of insulin resistance in obesity.
In the past years, free fatty acids (FFAs) and obesity have been reported to play an important role in cancer development. Palmitic acid (PA) is the most prevalent saturated FFA in circulation. However, the mechanism underlying the effect of PA on cell proliferation is still to be elucidated. In this report, we, for the first time, investigate the signaling pathway in human normal hepatocytes (QZG) responsible for PA-induced proliferation. The results demonstrate that PA promotes cell cycle progression, accelerates cell proliferation, and induces a transient and sequential activation of a series of kinases. The employment of several inhibitors and antioxidants indicates that a ROS-induced stress-sensitive p38 MAPK/ERK-Akt cascade plays a critical role in the regulation of PA on cell cycle and cell proliferation. Moreover, PA dose and time dependently activates Nrf2 and this activation relies on ROS-induced stimulation of p38 MAPK/ERK-Akt signaling, demonstrating that Nrf2 activation may be associated with the regulation of PA on cell cycle transition and proliferation. In conclusion, our study elucidates the importance of PA metabolism on cell proliferation, and suggests that PA stimulates hepatocyte proliferation through activating the ROS-p38 MAPK/ERK-Akt cascade which is intersected with the activation of Nrf2 and that the effect of ROS on signal transduction is in a dose- and time-dependent manner. All the above noted provide a new clue for the central role of ROS in cell proliferation and tumorigenesis.
In this study, we investigated the underlying molecular mechanism for the potent cell cycle inhibition and pro-apoptotic effect of luteolin (2-(3,4-dihydroxyphenyl)-5,7-dihydroxy-4-chromenone) on human non-small-cell lung carcinoma cell line A549. MTT assay showed that luteolin had obvious cytotoxicity on A549 with IC(50) of 40.2 μM at 48 h. Pro-apoptotic effect of luteolin on A549 cells was demonstrated by Hoechst 33258 staining assay and annexin V-FITC/PI double staining analysis. A great quantity of apoptotic cells and increasing G2 phase cells were observed by flow cytometry. Western blotting assay revealed that luteolin activated JNK, increased Bax, promoted procaspase-9 cleavage and activated caspase-3 at last. Assay using TNFα, an active agent of NF-κB, showed that pretreatment of A549 cells with luteolin could inhibit TNFα induced trans-nuclear of NF-κB. In summary, luteolin displayed a significant cytotoxic effect through cell cycle arrest and apoptosis induction in A549 cells. Pro-apoptotic effect was implemented via activating JNK and inhibiting translocation of NF-κB (p65). These results suggested that luteolin might have therapeutic potential against NSCLC.
Drug carriers are generally introduced into the body intravenously and directly exposed to endothelial cells. Silica nanoparticles could be promising delivery vehicles for drug targeting or gene therapy. However, few studies have been undertaken to determine the biological behavior of silica nanoparticles on endothelial cells. Here we measured reactive oxygen species (ROS) generation, apoptosis and necrosis, proinflammatory and prothrombic properties and the levels of the apoptotic signaling proteins and the transcription factors in human umbilical vein endothelial cells (HUVECs) after exposure to silica nanoparticles of different concentrations (25, 50, 100, and 200 microg/mL) for 24h. The results showed that silica nanoparticles, ranging from 50 microg/mL to 200 microg/mL, markedly induced ROS production, mitochondrial depolarization and apoptosis in HUVECs. At the highest concentration, the necrotic rate, LDH leakage, the expression of CD54 and CD62E, and the release of TF, IL-6, IL-8 and MCP-1 were significantly increased. Silica nanoparticles also activated c-Jun N-terminal kinase (JNK), c-Jun, p53, caspase-3 and NF-kappaB, increased Bax expression and suppressed Bcl-2 protein. Moreover, inhibition of ROS attenuated silica nanoparticles-induced apoptosis and inflammation and the activation of JNK, c-Jun, p53 and NF-kappaB. In summary, our findings demonstrated that silica nanoparticles could induce dysfunction of endothelial cells through oxidative stress via JNK, p53 and NF-kappaB pathways, suggesting that exposure to silica nanoparticles may be a significant risk for the development of cardiovascular diseases such as atherosclerosis and thrombus.
BACKGROUND:
Considering the key role of TF in coagulation of sepsis or acute lung injury (ALI), we investigated whether berberine (BBR) could inhibit TF expression and procoagulant activity and explored its possible mechanism.
METHODS:
The effects of berberine on the expression, procoagulant activity of TF and related signal pathways induced by lipopolysaccharide (LPS) were observed in THP-1 cells.
RESULTS:
Our results showed that berberine could inhibit LPS-induced TF activity and expression, and down-regulate NF-κB, Akt and MAPK/JNK/p38/ERK pathways.
CONCLUSION:
Berberine inhibits TF expression and related pathway, which provides some new insights on its mechanism for sepsis treatment.
Copyright © 2014 Institute of Pharmacology, Polish Academy of Sciences. Published by Elsevier Urban & Partner Sp. z o.o. All rights reserved.
OBJECTIVES:
The aim of this study was to investigate effects of mineral trioxide aggregate (MTA) on odonto/osteogenic differentiation of bone marrow stromal cells (BMSCs) from craniofacial bones.
MATERIALS AND METHODS:
Craniofacial BMSCs were isolated from rat mandible and effects of MTA on their proliferation, differentiation and MAPK pathway involvement were subsequently investigated, in vitro. MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl-2,5-tetrazoliumbromide) assay was performed to evaluate proliferation of the MTA-treated cells. Alkaline phosphatase (ALP) activity, alizarin red staining, real-time reverse transcription polymerase chain reaction and western blot assays were used to assess differentiation capacity as well as MAPK pathway involvement.
RESULTS:
0.02 mg/ml MTA-treated BMSCs had significantly higher ALP activity and formed more mineralized nodules than the untreated group. Odonto/osteoblastic marker genes/proteins (Alp, Runx2/RUNX2, Osx/OSX, Ocn/OCN and Dspp/DSP respectively) in MTA-treated cells were remarkably upregulated compared to untreated ones. Mechanistically, phosphorylated Jun N-terminal kinase (P-JNK) and phosphorylated extracellular regulated protein kinases (P-ERK) in MTA-treated BMSCs increased significantly in a time-dependent manner, while inhibition of JNK and ERK MAPK pathways dramatically blocked MTA-induced odonto/osteoblastic differentiation, as indicated by reduced ALP levels, weakened mineralization capacity and downregulated levels of odonto/osteoblastic marker genes (Alp, Runx2, Osx, Ocn and Dspp).
CONCLUSION:
Mineral trioxide aggregate promoted odonto/osteogenic capacity of craniofacial BMSCs via JNK and ERK MAPK signalling pathways.
© 2014 John Wiley & Sons Ltd.
SCOPE:
Flavonoids have well-known antioxidant, anti-inflammatory, and anti-cancer activities. Isoflavone genistein is considered a potent antioxidant agent against oxidative stress. Although several mechanisms have been proposed, a clear antioxidant mechanism of genistein is still remained to be answered.
METHODS AND RESULTS:
In this study, we focused on the concerted effects on expression of Nrf2 and phase II enzyme pathway components. Transient transfection assays, RT-PCR and immunoblot analysis were performed to study its molecular mechanisms of action. In Caco-2 cells, treatment with genistein markedly attenuated H(2)O(2) -induced peroxide formation; this amelioration was reversed by buthionine sulfoximine(GCLC inhibitor) and zinc protoporphyrin(HO-1 inhibitor). Genistein increased HO-1 and GCLC mRNA and protein expression. Genistein treatment activated the ERK1/2 and PKC signaling pathway; therefore increased Nrf2 mRNA and protein expression. The roles of the ERK1/2 and PKC signaling pathway were determined using PD98059 (ERK1/2 inhibitor) and GF109203X (PKC inhibitor) and RNA interference directed against Nrf2. Both inhibitors and siNrf2 abolished genistein-induced HO-1 and GCLC protein expression. These results suggest the involvement of ERK1/2, PKC, and Nrf2 in inducing HO-1 and GCLC by genistein.
CONCLUSION:
Our studies show that genistein up-regulated HO-1 and GCLC expression through the EKR1/2 and PKC /Nrf2 pathways during oxidative stress.
© 2012 WILEY-VCH Verlag GmbH & Co. KGaA, Weinheim.
AIM:
We investigated whether 8-dihydroxy-3-methyl-isochromanone (XJP-1), a novel angiotensin-converting enzyme inhibitor (ACEI), exhibited inhibitory activity to lipopolysaccharide (LPS)-accelerated vascular inflammation.
METHODS:
Human umbilical vein endothelial cells (HUVECs) were isolated from human umbilical cords and cultured. The direct effect of XJP-1 on the activation of endothelial cells was measured using MTT assay. Nitric oxide (NO) in the culture medium was measured using Griess method. The expression of cell adhesion molecules (ICAM-1 and VCAM-1) was determined by flow cytometry and RT-PCR. The protein expression levels of tumor necrosis factor-α (TNF-α), monocyte chemotactic protein (MCP)-1, and endothelin-1 (ET-1) secretion were measured using ELISA. Quantitative analysis of eNOS, iNOS, inhibitory factor NF-κB (IκB) and MAPKs were determined using Western blot analysis. The translocation of NF-κB from the cytoplasm to the nucleus was determined using immunofluorescence.
RESULTS:
XJP-1 significantly inhibited LPS-mediated endothelial cell dysfunction, as measured by NO production, iNOS expression, adhesion molecule (ICAM-1, VCAM-1) expression, and chemokine (TNF-α, MCP-1) production in vitro. It up-regulated eNOS expression in the same experimental setting. XJP-1 alone was found non-cytotoxic at the concentration up to 1000μM. The mechanistic investigations of XJP-1 suppression LPS-induced inflammation in HUVECs revealed that XJP-1 blocked NF-κB nuclear entry in an IκB-dependent manner, as well as inhibited MAPK activation induced by LPS. XJP-1 reduced endothelin-1 secretion and increased nitric oxide metabolite production by HUVECs. However, the effect of XJP-1 on nitric oxide and endothelin-1 metabolite production is mediated by the activation of bradykinin B(2) receptor being counteracted, at least in part, by a specific antagonist.
CONCLUSION:
XJP-1 inhibited LPS-induced cytotoxicity and inflammatory response. The mechanism underlying this protective effect might be related to the inhibition of MAPK and NF-κB signaling pathway activation, suggesting the potential inhibition of the atherosclerotic process by suppressing the expression of chemoattractant molecules and monocyte adhesion. XJP-1 also has an effect in improving endothelin-1 through activating bradykinin B(2) receptor. These findings indicated that XJP-1 is potentially a novel therapeutic candidate for the treatment of atherosclerosis.
Copyright © 2011 Elsevier Ireland Ltd. All rights reserved.
PURPOSE:
To determine the presence of integrin-linked kinase (ILK) in tissue samples of retinoblastoma patients, and to explore the function of ILK in human Y79 retinoblastoma cells.
METHODS:
The expression of ILK was studied in samples of retinoblastoma patients by immunohistochemistry. In vitro, specific small interfering RNA (siRNA) targeting ILK was transfected into Y79 retinoblastoma cells using liposome. Silencing of ILK expression was measured by reverse transcription-polymerase chain reaction (RT-PCR), real-time PCR and Western blotting assays. Then the regulation of cell proliferation and apoptosis was assessed by Cell Counting Kit-8(CCK-8), Annexin V-FITC/ propidium iodide (PI) immunofluorescence, and flow cytometry assays. Furthermore, the involvement of c-Jun N-terminal kinase signal pathway was tested by JNK signal transduction inhibitor assay.
RESULTS:
Positive staining for ILK was detected in 15 of the 17 retinoblastoma tissue samples. Specific siRNA targeting ILK significantly silenced ILK expression in Y79 retinoblastoma cells, as confirmed by RT-PCR, real-time PCR and Western blotting assays (P < 0.01). This was accompanied by decreased cell proliferation (P < 0.05) and enhanced apoptosis (P < 0.01). The phosphorylation status of JNK and c-Jun was constitutively activated by ILK siRNA (P < 0.01), and JNK inhibitor simultaneously reversed the effects on cell proliferation and apoptosis induced by ILK siRNA.
CONCLUSION:
Our results demonstrated that ILK promoted proliferation and suppressed apoptosis via repressing phosphorylations of the JNK signal pathway in human retinoblastoma cells. This might provide a potential therapeutic target in the treatment of this deadly disease.
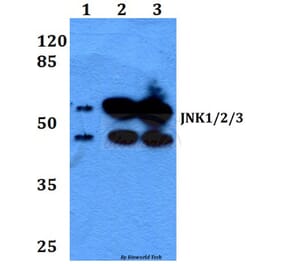
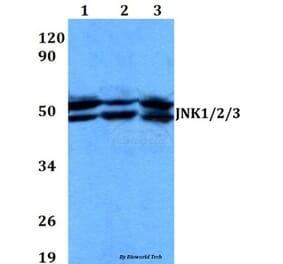















![Western Blot - Anti-JNK1 Antibody [ARC2908] (A306418) - Antibodies.com](https://cdn.antibodies.com/image/catalog/306/A306418_1.jpg?profile=product_alternative)