Unconjugated
This study investigated anti-inflammatory effects and possible mechanisms of Chikusetsusaponin IVa (Chi IVa), one of the main bioactive components in saponins from Panacis japonica (SPJ), which is used in traditional Tujia and Hmong Chinese medicine. To this end, changes in the inflammatory profiles of lipopolysacchride (LPS)-stimulated phrobol 12-myristate 13-acetate(PMA)-differented THP-1 macrophages were evaluated following Chi IVa treatment. The results showed that Chi IVa markedly decreased the expression of inducible nitric oxide synthase (iNOS), cyclooxygenase-2 (COX-2), interleukin-1 beta (IL-1β), interleukin-6 (IL-6), and tumor necrosis factor-α (TNF-α) at both the mRNA and protein level, which proved to be dose-dependent. Further studies revealed that Chi IVa strongly suppressed NF-κB activation and downregulated the phosphorylation of ERK, p38, and JNK. Our present study demonstrates that Chi IVa suppresses the production of iNOS, COX-2, IL-1β, IL-6, and TNF-α in LPS-stimulated THP-1 cells likely by inhibiting NF-κB activation and ERK, JNK, and p38 signal pathway phosphorylation.
Surgery-induced inflammation has been associated with cancer recurrence and metastasis in colorectal cancer (CRC). As a constituent of gram-negative bacteria, lipopolysaccharide (LPS) is frequently abundant in the peri-operative window. However, the definite roles of LPS in tumour progression remain elusive. Here we reported that LPS treatment increased PKM expression through activation of NF-κB signalling pathway, and knockdown of PKM reversed LPS-induced TNF-α, IL-1β production and cell proliferation in CRC cells. We further showed that the PKM2 but not PKM1 mediated the pro-inflammatory and proliferative effects of LPS. Interestingly, LPS promoted PKM2 binding to the STAT3 promoter to enhance STAT3 expression and its subsequent nuclear translocation. Depletion of STAT3 decreased PKM2-induced TNF-α and IL-1β expression, indicating that STAT3 mediates the pro-inflammatory effects of PKM2. Furthermore, it is the protein kinase activity but not the pyruvate kinase activity of PKM2 that is required for inflammatory cytokine production. Collectively, our findings reveal the NF-κB-PKM2-STAT3 axis as a novel mechanism for the regulation of TNF-α and IL-1β production and suggest the importance of PKM2 as a key inflammatory mediator in inflammatory microenvironment.
Alpha-lipoic acid (ALA), a naturally occurring compound and dietary supplement, has been established as a potent antioxidant that is a strong scavenger of free radicals. Recently, accumulating evidences has indicated the relationship between oxidative stress and osteoporosis (OP). Some studies have investigated the possible beneficial effects of ALA on OP both in vivo and in vitro; however, the precise mechanism(s) underlying the bone-protective action of ALA remains unclear. Considering this, we focused on the anti-oxidative capacity of ALA to exert bone-protective effects in vitro and in vivo. In the present study, the effects of ALA on osteoblastic formation in H(2)O(2) -treated MC3T3-E1 pre-osteoblasts and ovariectomy (OVX)-induced bone loss in rats were investigated. The results showed that ALA promoted osteoblast differentiation, mineralization and maturation and inhibited osteoblast apoptosis, thus increasing the OPG/receptor activator of nuclear factor-κB (NF-κB) ligand (RANKL) ratio and leading to enhanced bone formation in vitro and inhibited bone loss in vivo. Further study revealed that ALA exerted its bone-protective effects by inhibiting reactive oxygen species (ROS) generation by down-regulating Nox4 gene expression and protein synthesis and attenuating the transcriptional activation of NF-κB. In addition, ALA might exert its bone-protective effects by activating the Wnt/Lrp5/β-catenin signaling pathway. Taken together, the present study indicated that ALA promoted osteoblastic formation in H(2)O(2) -treated MC3T3-E1 cells and prevented OVX-induced bone loss in rats by regulating Nox4/ROS/NF-κB and Wnt/Lrp5/β-catenin signaling pathways, which provided possible mechanisms of bone-protective effects in regulating osteoblastic formation and preventing bone loss. Taken together, the results suggest that ALA may be a candidate for clinical OP treatment.
Cisplatin is a first-line chemotherapy drug against ovarian cancer. However, its strong toxic side effects and the development of cisplatin resistance in human cancer cells seriously influence the effects of chemotherapy and quality of life in patients. Noscapine (Nos), a non-toxic benzylisoquinoline alkaloid extracted from opium, has been recently reported to have anti-cancer activity, but the mechanism of that effect has not been clearly established. In the present study, we investigated cytotoxicity of Nos in combination with cisplatin (DDP) in drug-resistant human ovarian cancer cell line SKOV3/DDP in vitro and in vivo null mice xenograft model. Cell proliferation was measured by MTT assay, flow cytometry was used to analyze cell cycle and apoptosis, protein expression of several apoptotic factors was investigated by flow cytometry and immunohistochemical method, and their mRNA expression levels were determined by real-time PCR. In vitro experiments showed that Nos significantly inhibited proliferation of SKOV3/DDP cells. DDP/Nos-combined treatment notably enhanced DDP-induced inhibition of cell proliferation and increased the pro-apoptotic effect of DDP in SKOV3/DDP cells. DDP/Nos administration increased the proportion of G2/M cells, reduced both protein and mRNA expression of anti-apoptotic factors XIAP, surviving and NF-kB, and augmented protein and mRNA levels of pro-apoptotic caspase-3. In vivo experiments revealed that Nos/DDP treatment increased the apoptotic rate of xenograft tumors in null mice. Tumor volume decreased from 1.733 ± 0.155 g in mice treated with DDP alone to 1.191 ± 0.106 g in animals treated with Nos/DDP. These observations suggest that Nos increases the anti-cancer activity of DDP against the drug-resistant ovarian cancer cell line SKOV3/DDP by modulating the cell cycle and activating apoptotic pathways. The study provides a new chemotherapy strategy for the treatment of DDP-resistant human ovarian cancer.
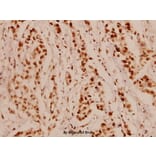
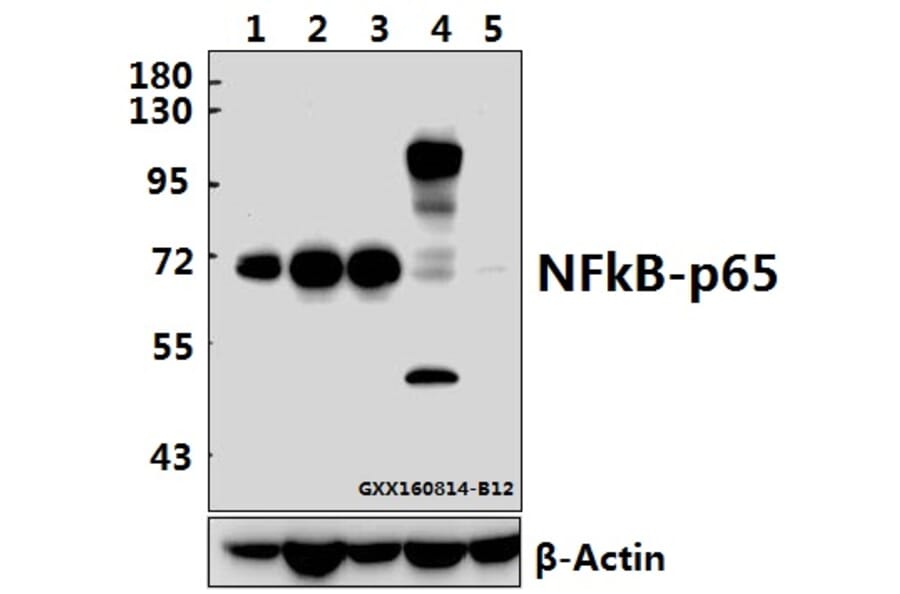
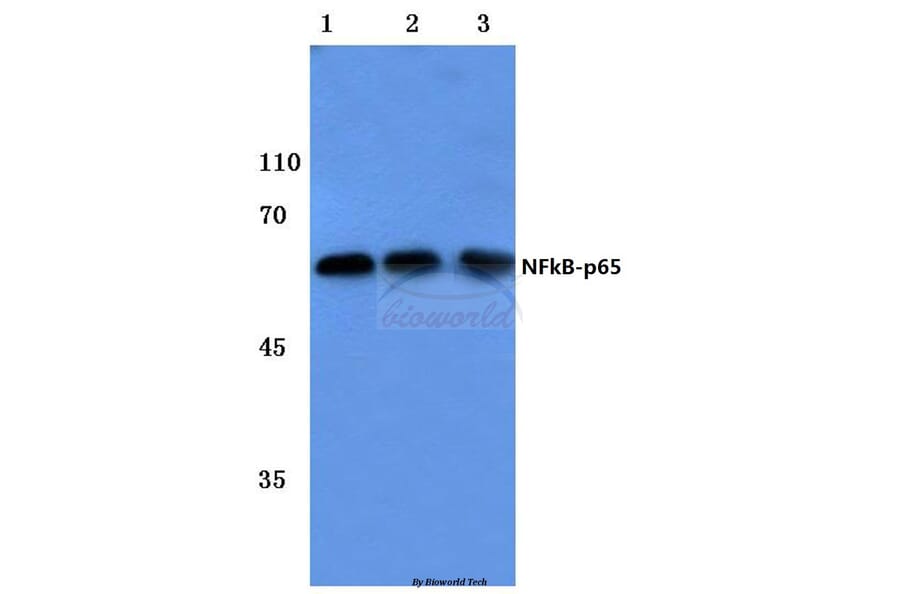
This study was designed to investigate the effects of mangiferin on renal fibrosis, osteopontin production, and inflammation in the kidney of diabetic rats. Diabetes was induced through the single administration of streptozotocin (55 mg/kg, i.p.). Diabetic rats were treated with mangiferin (15, 30, and 60 mg/kg/day, i.g.) for 9 weeks. The kidney was fixed in 10% formalin for glomerulus fibrosis examination using Masson trichrome staining. Kidney and blood were obtained for assays of the associated biochemical parameters. Chronic mangiferin treatment prevented renal glomerulus fibrosis evidenced by decreases in Mason-stained positive area of glomeruli, protein expression of type IV collagen, and α-smooth muscle actin in the kidney of diabetic rats, in comparison with decreases in mRNA and protein expression of osteopontin as well as protein expression of cyclooxygenase 2 and NF-кB p65 subunit in the renal cortex of diabetic rats. Moreover, mangiferin reduced the levels of interleukin 1β in both the serum and the kidney of diabetic rats. Our findings demonstrate that mangiferin prevents the renal glomerulus fibrosis of diabetic rats, which is realized through the suppression of osteopontin overproduction and inflammation likely via inactivation of NF-кB.
The crude powder of the fruit of Arctium lappa L. (ALF) has previously been reported to attenuate experimental colitis in mice. But, its main effective ingredient and underlying mechanisms remain to be identified. In this study, ALF was extracted with ethanol, and then successively fractionated into petroleum ether, ethyl acetate, n-butanol and water fraction. Experimental colitis was induced by dextran sulfate sodium (DSS) in mice. Among the four fractions of ALF, the ethyl acetate fraction showed the most significant inhibition of DSS-induced colitis in mice. The comparative studies of arctigenin and arctiin (the two main ingredients of ethyl acetate fraction) indicated that arctigenin rather than arctiin could reduce the loss of body weight, disease activity index and histological damage in the colon. Arctigenin markedly recovered the loss of intestinal epithelial cells (E-cadherin-positive cells) and decreased the infiltration of neutrophils (MPO-positive cells) and macrophages (CD68-positive cells). Arctigenin could down-regulate the expressions of TNF-α, IL-6, MIP-2, MCP-1, MAdCAM-1, ICAM-1 and VCAM-1 at both protein and mRNA levels in colonic tissues. Also, it markedly decreased the MDA level, but increased SOD activity and the GSH level. Of note, the efficacy of arctigenin was comparable or even superior to that of the positive control mesalazine. Moreover, it significantly suppressed the phosphorylation of MAPKs and the activation of NF-κB, including phosphorylation of IκBα and p65, p65 translocation and DNA binding activity. In conclusion, arctigenin but not arctiin is the main active ingredient of ALF for attenuating colitis via down-regulating the activation of MAPK and NF-κB pathways.
Mitofusin 2 (Mfn2) is a dynamin-like protein anchored in the outer mitochondrial membrane that plays a crucial role in ensuring optimal mitochondrial morphological homeostasis. It has been shown that reduced expression of Mfn2 is associated with insulin resistance, but the mechanism is still unclear. We investigated whether Mfn2 deficiency leads to impaired insulin sensitivity via elevated oxidative stress. L6 skeletal muscle cells were treated with palmitate and Mfn2 expression was repressed by transfection with antisense Mfn2. Levels of antioxidant enzymes, reactive oxygen species (ROS), the phosphorylation of c-Jun N-terminal Kinase (JNK) and nuclear factor-κB (NF-κB) and the mitochondrial membrane potential (Δψm) were measured. The results showed palmitate-induced insulin resistance of skeletal muscle cells was accompanied by Mfn2 repression. Meanwhile, the cells had decreased Δψm and activity of antioxidant enzymes which could increase production of ROS, phosphorylation of JNK and NF-κB. When Mfn2 was up-regulated in palmitate-treated cells, oxidative stress and insulin resistance was alleviated. Furthermore, knock-down of Mfn2 in control cells enhanced oxidative stress. Mfn2 deficiency led to increased superoxide concentration and activation of JNK as well as NF-κB associated with insulin signaling. In conclusion, Mfn2 is a potent repressor for oxidative stress and regulation of Mfn2 expression may prove to be a potential method to circumvent insulin resistance.
This study aimed to assess BA impact on inflammation markers and repair of intestinal mucosa. Forty-eight rats were randomly divided into stress (n = 24) and BA (n = 24) groups. Stress was induced by fettering in all animals, fed enterally with 125.4 kJ/kg/d and 0.2 g/kg/d nitrogen. Then, rats were treated for 8 days with 5 mg/kg/d BA (BA group) or 5 mg/kg/d saline (Stress group). Levels of NF-κB, IL-10, TNF-α, and IFN-γ were measured at different time points, in plasma and intestinal mucosa samples. Changes in intestinal mucosa morphology were observed by electron microscopy. Plasma and/or mucosal levels of NF-κB, TNF-α, and IFN-γ were significantly higher in both groups after stress induction (P < 0.05). These high levels persisted in control animals throughout the experiment, and were significantly reduced in the BA group, 3 and 8 days after stress induction (P < 0.05). Interestingly, IL-10 levels were increased after BA treatment (P < 0.05). At day 8, ileal mucosal villi and crypt structure were significantly restored in the BA group. Bifidobacterial adhesin plays a role in repairing intestinal mucosa injury after stress by regulating the release of inflammatory mediators in the intestinal mucosa.
Cichoric acid extract (CAE) from Echinacea purpurea L. was used to investigate the anti-arthritic effect by using collagen-induced arthritis (CIA) rat model. The hind paw swelling volume and the body weight were measured and recorded. All the drug solutions were administered orally to rats for a total of 28 days. On day 28, the rats were anaesthetized and decapitated. The thymus and spleen were weighed for the determination of the organ index. The concentration of tumor necrosis factor alpha (TNFα), interleukin-1 beta (IL-1β) and prostaglandin E2 (PGE-2) in the serum was measured using commercially available ELISA kits. Total and phosphor-NF-κB and Cox-2 protein expression in synovial tissues were determined by histological slides quantification and western blot analysis. Our data showed that administration of all doses of CAE (8, 16, and 32 mg/kg) significantly decreased the paw swelling, restored body weight gain and decreased the organ index of the thymus and spleen compared with that of the CIA group. CAE (8, 16, and 32 mg/kg) treatment significantly reduced the levels of TNFα, IL-1β and PGE-2 in serum compared with the CIA group. Histopathological analysis demonstrated that CAE has obvious anti-arthritic activity. In addition, CAE (32 mg/kg) significantly decreased the levels of nuclear factor-κB (NF-κB), TNFα and cyclooxygenase 2 (Cox-2) in synovium tissues of the ankle joint compared with the CIA group. Furthermore, CAE administration significantly decreased the protein expression of phosphor-NF-κB and Cox-2 in synovium tissues of the knee joint compared with the CIA group. The results suggest that the anti-inflammatory activity of CAE may account for its anti-arthritic effect, and CAE could be a potential therapeutic drug for the treatment of rheumatoid arthritis (RA).
Accumulating evidence indicate that macrophages activate mesenchymal stem cells (MSCs) to acquire pro-inflammatory phenotype. However, the role of MSCs activated by macrophages in gastric cancer remains largely unknown. In this study, we found that MSCs were activated by macrophages to produce increased levels of inflammatory cytokines. Cell colony formation and transwell migration assays revealed that supernatants from the activated MSCs could promote both gastric epithelial cell and gastric cancer cell proliferation and migration. In addition, the expression of epithelial-mesenchymal transition (EMT), angiogenesis, and stemness-related genes was increased in activated MSCs. The phosphorylated forms of NF-κB, ERK and STAT3 in gastric cells were increased by active MSCs. Inhibition of NF-κB activation by PDTC blocked the effect of activated MSCs on gastric cancer cells. Co-injection of activated MSCs with gastric cancer cells could accelerate gastric cancer growth. Moreover, human peripheral blood monocytes derived macrophages also activated MSCs to prompt gastric cancer cell proliferation and migration. Taken together, our findings suggest that MSCs activated by macrophage acquire pro-inflammatory phenotype and prompt gastric cancer growth in an NF-κB-dependent manner, which provides new evidence for the modulation of MSCs by tumor microenvironment and further insight to the role of stromal cells in gastric carcinogenesis and cancer progression.
Blood-brain barrier (BBB) disruption and brain edema formation play important roles in the secondary neuronal death and neurological dysfunction induced by intracerebral hemorrhage (ICH). Poloxamer 188 (P188), a multiblock copolymer surfactant, has been shown to be capable of sealing damaged cell membranes and decrease neuronal cell death. In this study, we explored whether P188 had a protective effect against ICH and its underlying mechanisms. Male ICR mice were subjected to infusion of type IV collagenase (to induce ICH) of saline (for shams) into the left striatum. The results showed that P188-12 mg post-treatment by tail intravenous injection significantly ameliorated the neurological symptoms and brain edema, attenuated BBB permeability, and decreased cell insults and injury volume at 24 and 72 h after ICH. Furthermore, P188 maintained the protein levels of tight junction (TJ) proteins including claudin-5, occludin, and zonula occludens-1, and reversed the increases of nuclear factor-kappaB (NF-κB), matrix metalloproteinase (MMP)-2, and MMP-9 protein expression at 72 h post ICH. Immunofluorescence showed P188 treatment rearranged the structure of TJ proteins in a continuous and linear pattern. Therefore, the present study concludes that P188 can protect against ICH, and the protective effect was associated with preventing BBB disruption through NF-κB-MMPs-mediated TJ proteins degradation.
D-galactosamine (GalN)/lipopolysaccharide (LPS)-induced lethality and acute liver failure is dependent on endogenously produced inflammatory cytokines. Adenosine has been proven to be a central role in the regulation of inflammatory response. It is not entirely clear that which adenosine action is actually crucial to limiting inflammatory tissue destruction. Here we showed that GalN/LPS challenge elevated hepatic adenosine and induced lethality in adenosine receptor-deficient mice with equal efficiency as wild-type mice. In GalN/LPS-treated mice, pretreatment with adenosine 5'-monophosphate (5'-AMP) significantly elevated hepatic adenosine level and reduced mortality through decreasing cytokine and chemokine production. In RAW264.7 cells, 5'-AMP treatment inhibited the production of inflammatory cytokines, which is not mediated through adenosine receptors. 5'-AMP failed to attenuate LPS-induced nuclear factor-κB (NF-κB) p65 nuclear translocation, but reduced LPS-induced recruitment of NF-κB p65 to inflammatory gene promoters and decreased LPS-induced enrichment of H3K4 dimethylation at the tumor necrosis factor-α (TNF-α) promoter, which was involved in 5'-AMP-induced elevation of cellular adenosine and a decline of methylation potential. In vitro biochemical analysis revealed that adenosine directly attenuated recruitment of NF-κB to the TNF-α and interleukin-6 promoters. Our findings demonstrate that 5'-AMP-inhibiting inflammatory response is not mediated by adenosine receptors and it may represent a potential protective agent for amelioration of LPS-induced liver injury.
Gastric cancer remains the main cause of cancer related deaths all over the world, and upregulated COX2 is a key player in its development. The mechanism as to how COX2 is regulated during the gastric cancer development is largely unknown. In this study, we found that the expression of COX2 was closely correlated with NF-κB activity. Strikingly, NF-κB activity was not absolutely consistent with its nuclear localization. Especially, in some cancer cell lines, such as MKN28, there were abundant nuclear localized NF-κB, while NF-κB luciferase activity in this cell line was relatively low. Furthermore, FOXP3 was found to be abundantly expressed in these cells. When the nuclear localized NF-κB expression was adjusted with the expression of FOXP3, it then correlated well with NF-κB activity. Molecularly, increased FOXP3 expression can interact with NF-κB and thus repress its activity. Knockdown of FOXP3 could increase NF-κB activity, COX2 expression, and cell migration. Taken together, our study revealed that function of FOXP3 as a negative regulator of NF-κB activity and thus plays a tumor suppressor role by reducing cell metastasis.
Reactive oxygen species (ROS)-induced oxidative stress increases in skeletal muscle with aging and decreases the viability of implanted cells. Type 1 insulin-like growth factor (IGF-1) promotes the survival of skeletal muscle cells under oxidative stress. It is unknown whether IGF-1 protects muscle-derived stem cells (MDSCs) from oxidative stress. In this study, we genetically engineered rat MDSCs to overexpress IGF-1 and determined cell viability, apoptosis, and VEGF secretion under oxidative stress. Overexpression of IGF-1 prevented MDSCs from H2O2-induced caspase-dependent apoptotic cell death by upregulating the PI3K/AKT pathway, accompanied with an increase of NF-κB, p-NF-κB, Bcl-2, and VEGF, as well as a decrease of Bax. In contrast, pre-administration of picropodophyllinb, wortmannin, 1L-6-hydroxymethyl-chiro-inositol-2-((R)-2-O-methyl-3-O-octadecylcarbonate), or pyrrolidine-dithiocarbamate, specific inhibitors of IGF-1R, PI3K, AKT, and NF-κB, respectively, followed by treatment with H2O2, resulted in cell death of MDSCs. Our data indicated that IGF-1 suppresses apoptosis and enhances the paracrine function of MDSCs under oxidative stress via enhancing IGF-1R/PI3K/AKT signaling. Thus, IGF-1 gene-modified MDSCs present a potential application in the treatment of muscle wasting, such as urethra intrinsic sphincter deficiency.
Besides secondary injury at the lesional site, Traumatic brain injury (TBI) can cause a systemic inflammatory response, which may cause damage to initially unaffected organs and potentially further exacerbate the original injury. Here we investigated plasma levels of important inflammatory mediators, oxidative activity of circulating leukocytes, particularly focusing on neutrophils, from TBI subjects and control subjects with general trauma from 6 hours to 2 weeks following injury, comparing with values from uninjured subjects. We observed increased plasma level of inflammatory cytokines/molecules TNF-α, IL-6 and CRP, dramatically increased circulating leukocyte counts and elevated expression of TNF-α and iNOS in circulating leukocytes from TBI patients, which suggests a systemic inflammatory response following TBI. Our data further showed increased free radical production in leukocyte homogenates and elevated expression of key oxidative enzymes iNOS, COX-2 and NADPH oxidase (gp91(phox)) in circulating leukocytes, indicating an intense induction of oxidative burst following TBI, which is significantly greater than that in control subjects with general trauma. Furthermore, flow cytometry assay proved neutrophils as the largest population in circulation after TBI and showed significantly up-regulated oxidative activity and suppressed phagocytosis rate for circulating neutrophils following brain trauma. It suggests that the highly activated neutrophils might play an important role in the secondary damage, even outside the injured brain. Taken together, the potent systemic inflammatory response induced by TBI, especially the intensively increase oxidative activity of circulating leukocytes, mainly neutrophils, may lead to a systemic damage, dysfunction/damage of bystander tissues/organs and even further exacerbate secondary local damage. Controlling these pathophysiological processes may be a promising therapeutic strategy and will protect unaffected organs and the injured brain from the secondary damage.
Nicotinamide adenine dinucleotide phosphate (NADPH) oxidase catalyzes the transfer of electrons from NADPH to O2, which is the main source of reactive oxygen species (ROS) in nonphagocytic cells. Excess ROS are toxic; therefore, keeping ROS in homeostasis in cells can protect cells from oxidative damage. It is meaningful to further understand the molecular mechanism by which ROS homeostasis is mediated. Human protein HSCARG is a newly identified oxidative sensor and a negative regulator of NF-κB. Here, we find that HSCARG represses the cellular ROS generation through inhibiting mRNA and protein expression of p47phox, a subunit of NADPH oxidase. In contrast, shRNA-mediated HSCARG knockdown increases endogenous p47phox expression level. And HSCARG has no obvious effect on ROS production in p47phox-depleted cells. Furthermore, HSCARG regulates p47phox through inhibition of NF-κB activity. Our findings identify HSCARG as a novel regulator in regulation of the activity of NADPH oxidase and ROS homeostasis.
Cigarette smoke exposure is associated with increased risk of different disorders. Immunological dysfunction especially in macrophages is one of important reasons in the initiation, progression and exacerbation of smoke-related pulmonary illnesses. However, it is still obscure how cigarette smoke impacts the vitality and functions of macrophages. In the present study, we examined the effects of cigarette smoke extract (CSE) on mouse Ana-1 macrophages and tried to elucidate the involved mechanism. The results showed CSE induced cell apoptosis accompanied by increased releasing of lactate dehydrogenase (LDH), mitochondrial injury and oxidative stress. It also inhibited anti-apoptosis protein Bcl-2 expression and promoted pro-apoptosis protein Bax and Bad expressions. Moreover, low-dose CSE increased nuclear NF-κB levels of macrophages; on the contrary, high-dose CSE or long-time treatment decreased it. These observations were in correspondence with changes of intracellular ROS level and antioxidant enzymes' activity. Furthermore, pretreatment with 10μM of NF-κB inhibitor pyrrolidine dithiocarbamate (PDTC) for 1h significantly enhanced macrophage apoptosis. Taken together, these data implied that mitochondrial dysfunction and oxidative stress played important roles in the injury of Ana-1 cells caused by CSE, which was related to NF-κB pathway; an anti-apoptotic program played a dominant role at low doses/short-term exposure to CSE, whereas a pro-apoptotic program was initiated at high doses/long-term exposure.
The expression of glucocorticoid receptor (GR) isoforms has been linked to glucocorticoid (GC) resistance in various diseases treated with GC. However, existing data are conflicting in these diseases, and little information is available regarding immune thrombocytopenia (ITP). To further investigate the role of GR isoforms in GC resistance in adult ITP patients, we measured the mRNA expression of GR isoforms (GRα, GRβ, GRγ, GRp) in peripheral blood mononuclear cells (PBMC) from 54 newly diagnosed ITP patients, including GC-sensitive (GCS) and GC-resistant (GCR) patients and 35 healthy volunteers. The GRα and GRβ proteins in PBMC, nuclear factor-κB (NF-κB), and activator protein-1 (AP-1) in the nucleus were detected by Western blotting. Compared to normal subjects, both GRα and GRβ mRNAs were significantly increased in ITP patients (p < 0.05), while there was no significant difference in the mRNA expression of GRγ and GRp. Compared to GCR patients, the expressions of GRα mRNA and GRα protein were significantly higher in GCS patients (p < 0.05). Moreover, no significant difference in the mRNA expression of the GRβ, GRγ, and GRp isoforms was observed between GCS and GCR patients and the GRβ protein could not be detected. Compared to GCS group, the expression of p65/NF-κB was significantly higher in the GCR group (p < 0.05). Overall, we did not find differences in c-Jun/AP-1 protein expression between GCS and GCR patients. In summary, GC resistance in adult ITP patients is associated with a reduced expression of GRα, which may be related with increased NF-κB. GRβ was very low and may not be involved in GC resistance in adult ITP, warranting further exploration.
Neonates with intrauterine growth retardation (IUGR) are susceptible to decreases in cellular immunity. In recent years, a growing body of evidence indicates that Hsp70 may serve as a danger signal to the innate immune system and promote receptor-mediated apoptosis. Using neonatal pigs with IUGR, we investigated immune function of pigs and expression of heat shock protein 70 (Hsp70), nuclear factor-kappa B (NF-κB), and forkhead box O 3a (FoxO3a) in the intestinal tract. Samples from the blood, duodenum, jejunum, and ileum of normal body weight (NBW) piglets and IUGR piglets were collected at day 7 after birth. Furthermore, to test whether Hsp70 is associated with regulation of NF-κB and FoxO3a, Hsp70 was silenced using small RNA interference (siRNA) in IEC-6 cells. Body and intestinal weights were lower in IUGR piglets than in NBW piglets (p < 0.05). Proliferation of peripheral blood lymphocytes was decreased (p < 0.05) in IUGR piglets. Cytokine concentrations (IFN-γ, IL-4, IL-10, IL-1, and IL-8) were lower in serum of IUGR piglets. The levels of IFN-γ and IL-10 were decreased (p < 0.05) in the ileum of IUGR piglets, but IL-4 was increased (p < 0.05). The expressions of Hsp70 and FoxO3a were increased, and NF-κB activity was downregulated in IUGR piglets (p < 0.05). Furthermore, siRNA-mediated Hsp70 downregulation increased NF-κB activity, inhibited expression of FoxO3a, and decreased cell apoptosis. In contrast, overexpression of Hsp70 inhibited NF-κB activation. In conclusion, IUGR impairs immune functions in neonatal pigs. An inefficient immunity in IUGR piglets is associated with overexpression of Hsp70, which impairs NF-κB signaling and upregulates FoxO3a expression.
BACKGROUND:
In our previous study, parathyroid hormone-like hormone (PTHLH) which encodes parathyroid hormone-related protein (PTHrP) was revealed to be up-regulated in oral squamous cell carcinoma (OSCC) compared with paired apparently normal surgical margins using microarray method. However, the function and prognostic indicators of PTHLH/PTHrP in OSCC remain obscure.
METHODS:
The mRNA levels of PTHLH and its protein levels were investigated in 9 OSCC cell lines and in 36 paired OSCC specimens by real-time PCR and western blotting. The biological function of PTHLH/PTHrP was investigated using small interfering RNA (siRNA) in 3 OSCC cell lines, and immunohistochemistry was used to estimate the prognostic value of PTHrP in 101 patients with head and neck squamous cell carcinoma (HNSCC), including OSCC and oropharyngeal squamous cell carcinoma. Cell cycle was tested by flow cytometry and cell cycle related genes were investigated by western blotting and immunocytochemistry assay.
RESULTS:
This study showed that the mRNA and protein levels of PTHLH in 9 OSCC cell lines were much higher than that in normal epithelial cells (P < 0.0001). In 36 paired OSCC tissues, PTHLH mRNA expressions were found higher in 32 OSCC tissues than that of paired apparently normal surgical margins (P = 0.0001). The results revealed that the down-regulation of PTHLH/PTHrP by siRNAs could reduce cell proliferation and inhibit plate and soft agar colony formation as well as affect the cell cycle of OSCC cells. The key proteins related to the cell cycle were changed by anti-PTHLH siRNA. The results showed that cyclin D1 and CDK4 expressions were significantly reduced in the cells transfected with anti-PTHLH siRNA. On the other hand, the expression of p21 was increased. The results also showed that high PTHrP level was associated with poor pathologic differentiation (P = 0.0001) and poor prognosis (P = 0.0003) in patients with HNSCC.
CONCLUSIONS:
This study suggests that PTHLH/PTHrP is up-regulated in OSCCs. Therefore, PTHLH/PTHrP could play a role in the pathogenesis of OSCC by affecting cell proliferation and cell cycle, and the protein levels of PTHrP might serve as a prognostic indicator for evaluating patients with HNSCCs.
OBJECTIVE:
Investigate the therapeutic effect of regional arterial infusion (RAI) with Aspirin-Triggered Lipoxin A4 (ATL) in experimental severe acute pancreatitis (SAP) in rats.
MATERIALS AND METHODS:
SAP was induced by injection of 5% sodium taurocholate into the pancreatic duct. Rats with SAP were treated with ATL (the ATL group) or physiological saline (the SAP group) infused via the left gastric artery 30 min after injection of sodium taurocholate. The sham group was subjected to the same surgical procedure, though without induction of SAP. Serum levels of amylase, phospholipase A2 (PLA2), interleukin-1β (IL-1β), IL-6 and tumor necrosis factor-α (TNF-α) were measured at 12 and 24 h after induction of SAP. Ascitic fluid, the pancreatic index (wet weight ratio) and myeloperoxidase (MPO) levels in the pancreas were determined and histopathological findings were evaluated. The expression of intercellular adhesion molecule-1 (ICAM-1), platelet endothelial cell adhesion molecule-1 (PECAM-1), NF-κB p65, and heme oxygenase-1 (HO-1) in the pancreas were estimated by immunofluorescence and western blot, respectively.
RESULTS:
ATL rats had lower serum levels of TNF-α, IL-1β, and IL-6 (P<0.01), PLA2 (P<0.05), and amylase levels (P<0.05) studied as compared with the SAP group. The pancreatic index in the ATL group decreased only at 24 h as compared with the SAP group (P<0.05). The histopathological findings and MPO levels in the pancreas significantly decreased in the ATL group as compared to the SAP group (P<0.05 and P<0.01, respectively). Immunofluorescence and western blot showed that ATL attenuated the expression of NF-κB p65, ICAM-1 and PECAM-1 in the pancreas, and increased the expression of HO-1 in SAP animals.
CONCLUSIONS:
We demonstrated that RAI with ATL attenuated the severity of experimental SAP, maybe achieved by improving the expression of HO-1, and down-regulating the NF-κB signaling pathway, with decreased expression of ICAM-1 and PECAM-1 and reduced generation of pro-inflammatory cytokines.
AIM:
To investigate the mechanisms of how cyclooxygenase-2 (COX-2) regulates E-cadherin in gastric cancer cells.
METHODS:
COX-2 expression in human gastric cancer cell lines SGC-7901, BGC-823, MGC-803 and AGS were measured at the mRNA and protein level. COX-2 rich cell line SGC-7901 was chosen for subsequent experiments. siRNA mediated gene knockdown was used to investigate the impact of COX-2 on nuclear factor-κB (NF-κB), Snail, and E-cadherin in gastric cancer cells. Gene expression was determined by Western blot and real-time polymerase chain reaction. To analyze whether NF-κB inhibition could interrupt the modulatory effect of COX-2 or prostaglandin E2 (PGE2) on E-cadherin, gastric cancer cells were treated with celecoxib or PGE2, in the presence of NF-κB specific siRNA.
RESULTS:
Highest expression level of COX-2 was found in SGC-7901 cells, both at mRNA and protein levels. siRNA mediated down-regulation of COX-2 led to a reduced expression of NF-κB and Snail, but an increased expression of E-cadherin in SGC-7901 cells. siRNA mediated down-regulation of NF-κB also led to a reduced expression of E-cadherin and Snail in SGC-7901 cells. However, COX-2 expression did not alter after cells were treated with NF-κB specific siRNA in SGC-7901 cells. Treatment of SGC-7901 cells with celecoxib led to a reduced expression of Snail but an increased expression of E-cadherin. In contrast, treatment of SGC-7901 cells with PGE2 led to an increased Snail and a decreased E-cadherin. However, siRNA-mediated knockdown of NF-κB partially abolished the effect of celecoxib and PGE2 on the regulation of E-cadherin and Snail in SGC-7901 cells.
CONCLUSION:
COX-2 likely functions upstream of NF-κB and regulates the expression of E-cadherin via NF-κB/Snail signaling pathway in gastric cancer cells.
ETHNOPHARMACOLOGICAL RELEVANCE:
Cordyceps sinensis has been used as a precious herbal medicine for thousands of years in China. Its polysaccharide fraction has been confirmed possessing immunomodulatory function and we have reported the acid polysaccharide fraction (APSF), from an anamorph of C. sinensis, has stimulating activity on macrophages. The mechanism still needs to be further elucidated.
MATERIALS AND METHODS:
In order to investigate the effects of APSF on macrophage's phenotypes, Ana-1 mouse macrophages were polarized to M2 phenotype by culturing the cells with culture supernatant of H22 cells. M2 phenotype was determined by measuring the expression of TNF-α and checking cell surface markers mannose receptor (MR) and scavenger receptor (SR). After cultured with H22 supernatant for 72 h, the TNF-α level of Ana-1 cells was decreased while the SR and MR expressions were up-regulated, suggesting that Ana-1 cells were polarized towards M2 macrophages. Then the effects of APSF on M2 macrophages were investigated by measuring mRNA levels of TNF-α, inducible nitric oxide synthase (iNOS), IL-12 and IL-10. Nuclear NF-κB was detected by Western blotting.
RESULTS:
APSF treatment increased the expressions of TNF-α, IL-12 and iNOS, and reduced the expression of IL-10 of Ana-1 cells. Besides, the expressions of SR and MR were down-regulated by APSF. And the result of Western blotting showed NF-κB level was decreased in M2 macrophages and up-regulated after APSF treatment.
CONCLUSIONS:
APSF may convert M2 macrophages to M1 phenotype by activating NF-κB pathway.
Copyright © 2012 Elsevier Ireland Ltd. All rights reserved.
OBJECTIVES:
The main pathogenesis of acute lung injury induced by haemorrhagic shock is inflammation. BML-111, a lipoxinA(4)-receptor agonist, promotes acute inflammatory resolution. We sought to elucidate whether BML-111 protects haemorrhagic shock-induced acute lung injury in rats.
METHODS:
Thirty two adult male rats were randomized to sham group (sham), haemorrhagic shock/resuscitation (HS), HS plus BML-111 (BML-111), and HS plus BML-111 and BOC-2 (BOC-2). Haemorrhagic shock was induced by blood drawing, and then resuscitation was obtained by infusion of shed blood and two-fold volume saline.
RESULTS:
Histological findings, as well as assays of neutrophilic infiltration (myeloperoxidase activity, ICAM-1 expression), inflammatory cytokines and pro-inflammatory factor (IκB-α and NF-κB p65) confirmed that haemorrhagic shock induced acute lung injury. BML-111 significantly mitigated acute lung injury induced by haemorrhagic shock. However, BOC-2, an antagonist of the lipoxinA(4)-receptor, partially reversed the protective effect of BML-111 on the haemorrhagic shock-induced the acute lung injury.
CONCLUSION:
BML-111 protects haemorrhagic shock-induced acute lung injury in rats.
Copyright © 2012 Elsevier Ireland Ltd. All rights reserved.
BACKGROUND:
Most patients after liver transplantation (LT) suffer from intestinal barrier dysfunction. Glycyl-glutamine (Gly-Gln) by parenteral supplementation is hydrolyzed to release glutamine, which improves intestinal barrier function in intestinal injury. This study aimed to investigate the effect of Gly-Gln by enteral supplementation on intestinal barrier function in rats after allogenetic LT under immunosuppressive therapy.
METHODS:
Twelve inbred Lewis rats were selected randomly as donors, and 24 inbred Brown Norway (BN) rats as recipients of allogenetic LT. The recipients were divided into a control group (Ala, n=12) and an experimental group (Gly-Gln, n=12). In each group, 6 normal BN rats were sampled for normal parameters on preoperative day 3. The 6 recipients in the control group received alanine (Ala) daily by gastric perfusion for 3 preoperative days and 7 postoperative days, and the 6 recipients in the experimental group were given Gly-Gln in the same manner. The 12 BN recipients underwent orthotopic LT under sterile conditions after a 3-day fast and were given immunosuppressive therapy for 7 days. They were harvested for sampling on postoperative day 8. The following parameters were assessed: intestinal mucosal protein content, mucosal ultrastructure, ileocecal sIgA content, portal plasma levels of endotoxin and TNF-alpha, and bacterial translocation.
RESULTS:
All recipients were alive after LT. On preoperative day 3, all parameters were similar in the two groups. On postoperative day 8, all parameters in the two groups were remarkably changed from those on preoperative day 3. However, compared to the Ala group, supplementation with Gly-Gln increased the levels of intestinal mucosal protein and ileocecal sIgA, improved mucosal microvilli, and decreased portal plasma levels of endotoxin and TNF-alpha as well as bacterial translocation.
CONCLUSION:
Enteral supplementation with Gly-Gln improved intestinal barrier function after allogenetic LT in rats.
BACKGROUND:
Stimulation of Toll-like receptors (TLRs) by microbial products has been utilised to potentiate immune responses against haematologic malignancies. The maltose-binding protein (MBP) of Escherichia coli could induce the activation of immune cells via TLR4. The aim of the present study was to investigate whether TLRs mediated the biological effects of MBP on U937 and Jurkat cells in vitro. METHODS We observed the effect of MBP on U937 and Jurkat cells by using the WST, cell cycle analysis and morphological observation. Further, cells were stimulated with MBP for indicated times and doses, and detected by RT-PCR, western blotting, immunohistochemistry and immunofluorescence staining to investigate the mechanisms involved in cell viability.
RESULTS:
MBP enhanced the viability of U937 and Jurkat cells, and the effects were blocked by anti-TLR2, but not anti-TLR4 in U937 cells. Further studies confirmed that MBP was able to directly bind to U937 and Jurkat cells and modulate TLR expression. The effects of MBP depended on the activation of NF-κB and MAP kinase in U937 and Jurkat cells.
CONCLUSIONS:
Our results demonstrated that MBP could directly promote U937 cell viability via TLR2. It suggested that MBP may be used as an adjuvant for participating in the immunotherapy of haematologic malignancies.