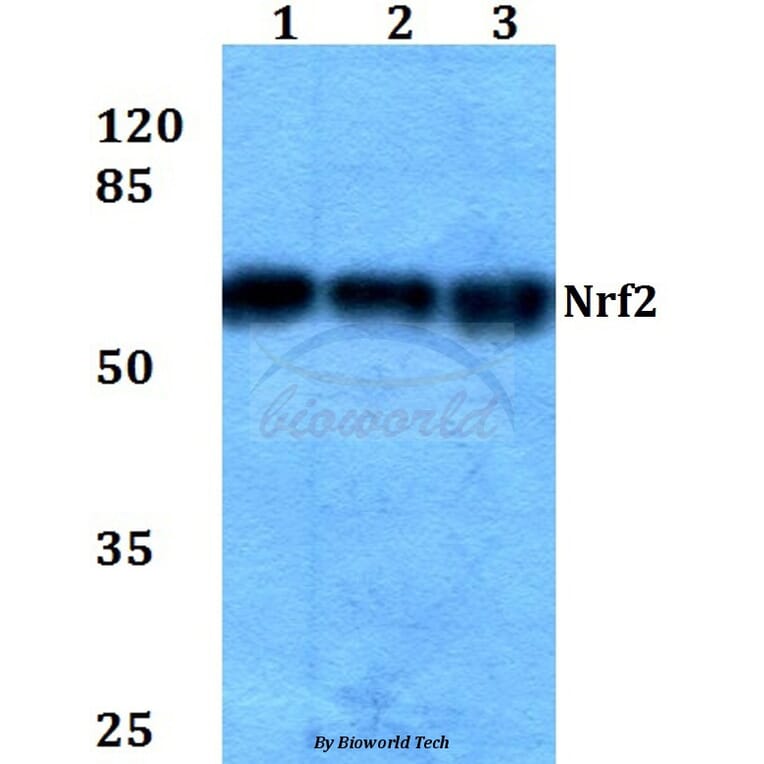
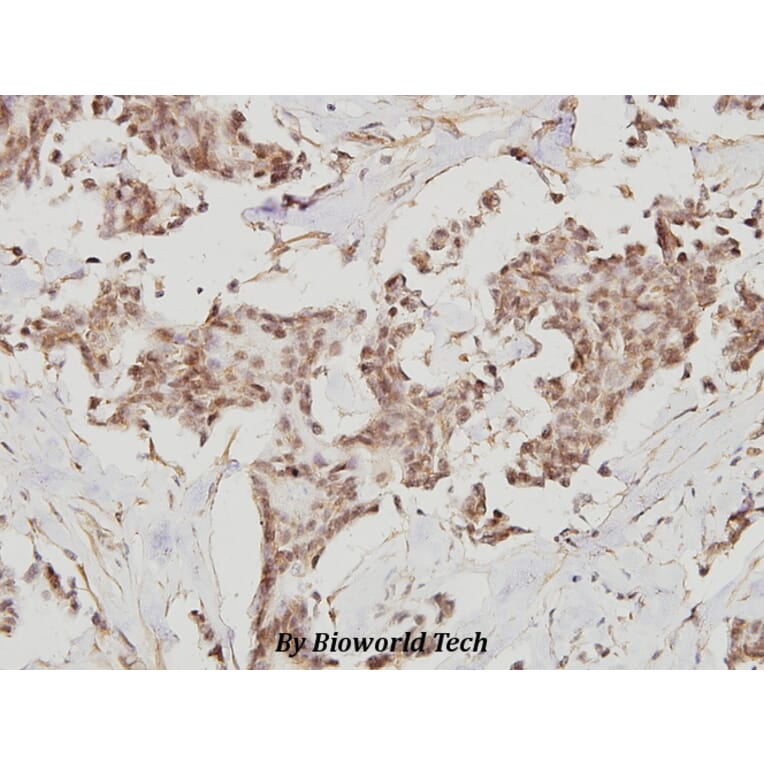
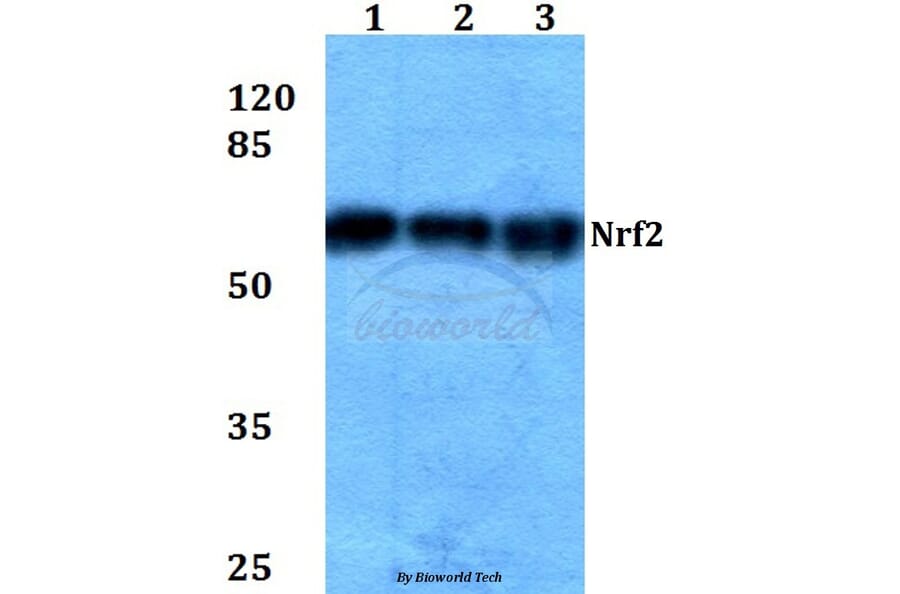
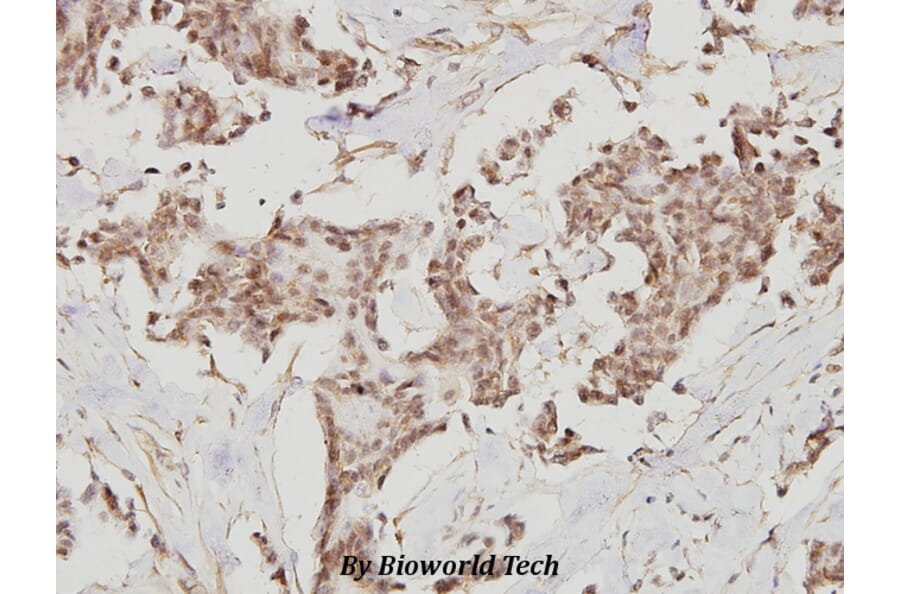
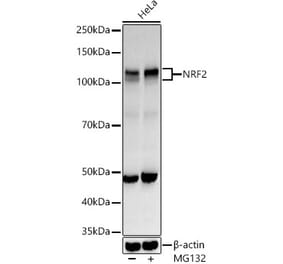
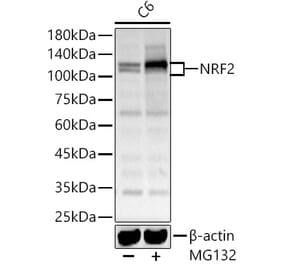
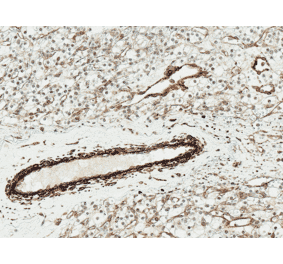
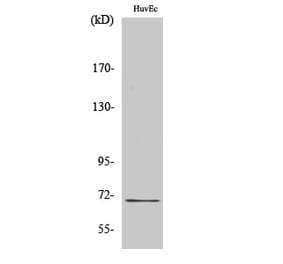
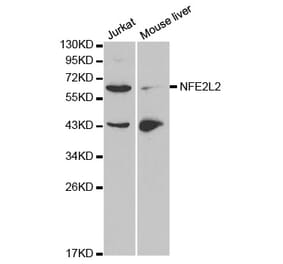
Unconjugated
Alpha-lipoic acid (ALA), occurring naturally in human food, is known to possess antioxidative and anti-inflammatory activities. Induction of heme oxygenase-1 (HO-1) has been reported to exhibit a therapeutic effect in several inflammatory diseases. The aim of study was to test the hypothesis that the protection of ALA against lipopolysaccharide-(LPS-) induced acute lung injury (ALI) is mediated by HO-1. Pre- or posttreatment with ALA significantly inhibited LPS-induced histological alterations of ALI, lung tissue edema, and production of proinflammatory cytokine, cytokine inducible neutrophil chemoattractant-3, and nitrite/nitrate in bronchoalveolar lavage fluid. In addition, the inflammatory responses including elevation of superoxide formation, myeloperoxidase activity, polymorphonuclear neutrophils infiltration, nitrotyrosine, inducible nitric oxide synthase expression and nuclear factor-kappa B (NF- κ B) activation in lung tissues of LPS-instilled rats were also markedly reduced by ALA. Interestingly, treatment with ALA significantly increased nuclear factor-erythroid 2-related factor 2 (Nrf2) activation and HO-1 expression in lungs of ALI. However, blocking HO-1 activity by tin protoporphyrin IX (SnPP), an HO-1 inhibitor, markedly abolished these beneficial effects of ALA in LPS-induced ALI. These results suggest that the protection mechanism of ALA may be through HO-1 induction and in turn suppressing NF- κ B-mediated inflammatory responses.
AIM:
SMXZF (a combination of ginsenoside Rb1, ginsenoside Rg1, schizandrin and DT-13) derived from Chinese traditional medicine formula ShengMai preparations) is capable of alleviating cerebral ischemia-reperfusion injury in mice. In this study we used network pharmacology approach to explore the mechanisms of SMXZF in the treatment of cardio-cerebral ischemic diseases.
METHODS:
Based upon the chemical predictors, such as chemical structure, pharmacological information and systems biology functional data analysis, a target-pathway interaction network was constructed to identify potential pathways and targets of SMXZF in the treatment of cardio-cerebral ischemia. Furthermore, the most related pathways were verified in TNF-α-treated human vascular endothelial EA.hy926 cells and H2O2-treated rat PC12 cells.
RESULTS:
Three signaling pathways including the NF-κB pathway, oxidative stress pathway and cytokine network pathway were demonstrated to be the main signaling pathways. The results from the gene ontology analysis were in accordance with these signaling pathways. The target proteins were found to be associated with other diseases such as vision, renal and metabolic diseases, although they exerted therapeutic actions on cardio-cerebral ischemic diseases. Furthermore, SMXZF not only dose-dependently inhibited the phosphorylation of NF-κB, p50, p65 and IKKα/β in TNF-α-treated EA.hy926 cells, but also regulated the Nrf2/HO-1 pathway in H2O2-treated PC12 cells.
CONCLUSION:
NF-κB signaling pathway, oxidative stress pathway and cytokine network pathway are mainly responsible for the therapeutic actions of SMXZF against cardio-cerebral ischemic diseases.
INTRODUCTION:
Osteoarthritis (OA) is a common joint disease that can cause gradual disability among the aging population. Nuclear factor (erythroid-derived 2)-like 2 (Nrf2) is a key transcription factor that regulates the expression of phase II antioxidant enzymes that provide protection against oxidative stress and tissue damage. The use of histone deacetylase inhibitors (HDACi) has emerged as a potential therapeutic strategy for various diseases. They have displayed chondroprotective effects in various animal models of arthritis. Previous studies have established that Nrf2 acetylation enhances Nrf2 functions. Here we explore the role of Nrf2 in the development of OA and the involvement of Nrf2 acetylation in HDACi protection of OA.
METHODS:
Two OA models-monosodium iodoacetate (MIA) articular injection and destabilization of the medial meniscus (DMM)-were used with wild-type (WT) and Nrf2-knockout (Nrf2-KO) mice to demonstrate the role of Nrf2 in OA progression. A pan-HDACi, trichostatin A (TSA), was administered to examine the effectiveness of HDACi on protection from cartilage damage. The histological sections were scored. The expression of OA-associated matrix metalloproteinases (MMPs) 1, 3, and 13 and proinflammatory cytokines tumor necrosis factor (TNF)-α, interleukin (IL)-1β, and IL-6 were assayed. The effectiveness of HDACi on OA protection was compared between WT and Nrf2-KO mice.
RESULTS:
Nrf2-KO mice displayed more severe cartilage damage in both the MIA and DMM models. TSA promoted the induction of Nrf2 downstream proteins in SW1353 chondrosarcoma cells and in mouse joint tissues. TSA also reduced the expression of OA-associated proteins MMP1, MMP3, and MMP13 and proinflammatory cytokines TNF-α, IL-1β, and IL-6. TSA markedly reduced the cartilage damage in both OA models but offered no significant protection in Nrf2-KO mice.
CONCLUSIONS:
Nrf2 has a major chondroprotective role in progression of OA and is a critical molecule in HDACi-mediated OA protection.
BACKGROUND:
Over-production of mucus is an important pathophysiological feature in chronic airway disease such as chronic obstructive pulmonary disease (COPD) and asthma. Cigarette smoking (CS) is the leading cause of COPD. Oxidative stress plays a key role in CS-induced airway abnormal mucus production. Hydrogen protected cells and tissues against oxidative damage by scavenging hydroxyl radicals. In the present study we investigated the effect of hydrogen on CS-induced mucus production in rats.
METHODS:
Male Sprague-Dawley rats were divided into four groups: sham control, CS group, hydrogen-rich saline pretreatment group and hydrogen-rich saline control group. Lung morphology and tissue biochemical changes were determined by immunohistochemistry, Alcian Blue/periodic acid-Schiff staining, TUNEL, western blot and realtime RT-PCR.
RESULTS:
Hydrogen-rich saline pretreatment attenuated CS-induced mucus accumulation in the bronchiolar lumen, goblet cell hyperplasia, muc5ac over-expression and abnormal cell apoptosis in the airway epithelium as well as malondialdehyde increase in the BALF. The phosphorylation of EGFR at Tyr1068 and Nrf2 up-regulation expression in the rat lungs challenged by CS exposure were also abrogated by hydrogen-rich saline.
CONCLUSION:
Hydrogen-rich saline pretreatment ameliorated CS-induced airway mucus production and airway epithelium damage in rats. The protective role of hydrogen on CS-exposed rat lungs was achieved at least partly by its free radical scavenging ability. This is the first report to demonstrate that intraperitoneal administration of hydrogen-rich saline protected rat airways against CS damage and it could be promising in treating abnormal airway mucus production in COPD.
AIM:
To investigate the protective effects of hydrogen sulfide (H2S) against inflammation, oxidative stress and apoptosis in a rat model of resuscitated hemorrhagic shock.
METHODS:
Hemorrhagic shock was induced in adult male SD rats by drawing blood from the femoral artery for 10 min. The mean arterial pressure was maintained at 35-40 mmHg for 1.5 h. After resuscitation the animals were observed for 200 min, and then killed. The lungs were harvested and bronchoalveolar lavage fluid was prepared. The levels of relevant proteins were examined using Western blotting and immunohistochemical analyses. NaHS (28 μmol/kg, ip) was injected before the resuscitation.
RESULTS:
Resuscitated hemorrhagic shock induced lung inflammatory responses and significantly increased the levels of inflammatory cytokines IL-6, TNF-α, and HMGB1 in bronchoalveolar lavage fluid. Furthermore, resuscitated hemorrhagic shock caused marked oxidative stress in lung tissue as shown by significant increases in the production of reactive oxygen species H2O2 and ·OH, the translocation of Nrf2, an important regulator of antioxidant expression, into nucleus, and the decrease of thioredoxin 1 expression. Moreover, resuscitated hemorrhagic shock markedly increased the expression of death receptor Fas and Fas-ligand and the number apoptotic cells in lung tissue, as well as the expression of pro-apoptotic proteins FADD, active-caspase 3, active-caspase 8, Bax, and decreased the expression of Bcl-2. Injection with NaHS significantly attenuated these pathophysiological abnormalities induced by the resuscitated hemorrhagic shock.
CONCLUSION:
NaHS administration protects rat lungs against inflammatory responses induced by resuscitated hemorrhagic shock via suppressing oxidative stress and the Fas/FasL apoptotic signaling pathway.
PURPOSE:
3,3'-Diindolylmethane (DIM) is a natural component of cruciferous plants. It has strong antioxidant and anti-angiogenic effects and promotes the apoptosis of a variety of tumor cells. However, little is known about the critical role of DIM on cardiac hypertrophy. In the present study, we investigated the effects of DIM on cardiac hypertrophy.
METHODS:
Multiple molecular techniques such as Western blot analysis, real-time PCR to determine RNA expression levels of hypertrophic, fibrotic and oxidative stress markers, and histological analysis including H&E for histopathology, PSR for collagen deposition, WGA for myocyte cross-sectional area, and immunohistochemical staining for protein expression were used.
RESULTS:
In pre-treatment and reverse experiments, C57/BL6 mouse chow containing 0.05% DIM (dose 100 mg/kg/d DIM) was administered one week prior to surgery or one week after surgery, respectively, and continued for 8 weeks after surgery. In both experiments, DIM reduced to cardiac hypertrophy and fibrosis induced by aortic banding through the activation of 5'-adenosine monophosphate-activated protein kinase-α2 (AMPKα2) and inhibition of mammalian target of the rapamycin (mTOR) signaling pathway. Furthermore, DIM protected against cardiac oxidative stress by regulating expression of estrogen-related receptor-alpha (ERRα) and NRF2 etc. The cardioprotective effects of DIM were ablated in mice lacking functional AMPKα2.
CONCLUSION:
DIM significantly improves left ventricular function via the activation of AMPKα2 in a murine model of cardiac hypertrophy.
BACKGROUND:
Traditional Chinese medicinal herbs Cortex Moutan and Radix Salviae Milthiorrhizaeare are prescribed together for their putative cardioprotective effects in clinical practice. However, the rationale of the combined use remains unclear. The present study was designed to investigate the cardioprotective effects of paeonol and danshensu (representative active ingredient of Cortex Moutan and Radix Salviae Milthiorrhizae, respectively) on isoproterenol-induced myocardial infarction in rats and its underlying mechanisms.
METHODOLOGY:
Paeonol (80 mg kg(-1)) and danshensu (160 mg kg(-1)) were administered orally to Sprague Dawley rats in individual or in combination for 21 days. At the end of this period, rats were administered isoproterenol (85 mg kg(-1)) subcutaneously to induce myocardial injury. After induction, rats were anaesthetized with pentobarbital sodium (35 mg kg(-1)) to record electrocardiogram, then sacrificed and biochemical assays of the heart tissues were performed.
PRINCIPAL FINDINGS:
Induction of rats with isoproterenol resulted in a marked (P<0.001) elevation in ST-segment, infarct size, level of serum marker enzymes (CK-MB, LDH, AST and ALT), cTnI, TBARS, protein expression of Bax and Caspase-3 and a significant decrease in the activities of endogenous antioxidants (SOD, CAT, GPx, GR, and GST) and protein expression of Bcl-2. Pretreatment with paeonol and danshensu combination showed a significant (P<0.001) decrease in ST-segment elevation, infarct size, cTnI, TBARS, protein expression of Bax and Caspase-3 and a significant increase in the activities of endogenous antioxidants and protein expression of Bcl-2 and Nrf2 when compared with individual treated groups.
CONCLUSIONS/SIGNIFICANCE:
This study demonstrates the cardioprotective effect of paeonol and danshensu combination on isoproterenol-induced myocardial infarction in rats. The mechanism might be associated with the enhancement of antioxidant defense system through activating of Nrf2 signaling and anti-apoptosis through regulating Bax, Bcl-2 and Caspase-3. It could provide experimental evidence to support the rationality of combinatorial use of traditional Chinese medicine in clinical practice.
Quinoxaline 1,4-dioxides (QdNOs) are widely used as a kind of antibacterial growth promoter in animal husbandry. The adrenal cortex was found to be one of the main toxic targets of QdNOs, accompanied by a decreased aldosterone level. However, the way in which QdNOs decrease production of the hormone aldosterone is far from clear. To illustrate the mechanism by which QdNOs damage the adrenal cortex and decrease aldosterone hormone levels, the QdNOs were screened to choose the drug with most toxic effects on aldosterone production, and then to reveal the mechanism between the gene and protein profiles in human adrenocortical cells (NCI-H295R cells). The results found that quinocetone (QCT) showed the highest adrenal toxic effect among QdNOs. After exposing H295R cells to 10 and 20μM QCT for 24h, compared with blank cells, the gene and protein expression profiles obtained were analyzed by microarray and MALDI TOF/TOF mass spectrometry, respectively. The results of microarray analysis suggested that ABCG1 and SREBF1, which were involved in the cholesterol biosynthetic and metabolic processes, and CYP17A1, NR4A2 and G6PD, which were related to aldosterone biosynthesis, were important molecular targets. It has been speculated that PKC and ERK pathways might be involved in the reduction of aldosterone production caused by QCT, through enhanced mRNA expression of CYP17A1. Additionally, JNK and p38MAPK signal transduction pathways might participate in apoptosis induced by QCT. Twenty-nine and 32 protein spots were successfully identified when cells were treated with 10 and 20μM QCT, respectively. These identified proteins mainly included material synthesis and energy metabolism-related proteins, transcription/translation processing-related proteins, signal transduction proteins, cytoskeletal proteins, molecular chaperones, proteins related to response to stress, and transport proteins. Further investigations suggested that oxidative stress caused by QCT was exacerbated through disruption of the Keap1/Nrf2/ARE anti-oxidative stress pathway. Taken together, the data demonstrated for the first time that the Keap1/Nrf2/ARE pathway plays a crucial role in adrenal toxicity, and that CYP17A1 was the key switch to reduce the aldosterone production induced by QCT. Furthermore, large numbers of genes and proteins and entry points for research in the inhibition of aldosterone synthesis induced by QCT were offered, which will provide new insight into the adrenal toxicity of QdNOs and help to provide a theoretical foundation for the formulation of safety controls for products obtained from animals and to design new QdNOs with less harmful effects.
NLRP3 inflammasome is a key component of the inflammatory process and its dysregulation contributes to IBD for its ability to induce IL-1β release. Previously, we reported that a novel small molecular activator of Nrf2, 3-(2-oxo-2-phenylethylidene)-2,3,6,7-tetrahydro-1H-pyrazino-[2,1-a]isoquinolin-4(11bH)-one (compound 1) can prevent the development of colorectal adenomas in AOM-DSS models. Here we further investigated the anti-inflammatory effect of compound 1 in DSS-induced colitis in C57BL/6 and NLRP3(-/-) mice, and revealed the possible modulation by compound 1 of NLRP3 inflammasome-mediated IL-1β release from macrophages. In C57BL/6 mice, oral administration of compound 1 significantly attenuated DSS-induced colonic pathological damage, remarkably inhibited inflammatory cells infiltration and decreased myeloperoxidase (MPO) and IL-1β secretion in colons. In contrast, mice deficient for NLRP3 were less sensitive to DSS-induced acute colitis, and compound 1 treatment exerted no protective effect on DSS-induced intestinal inflammation in NLRP3(-/-) mice. The protective effect of compound 1 may be attributed to its inhibition of NLRP3 inflammasome and Nrf2 activation in colons. Furthermore, compound 1, as a small molecular activator of Nrf2, significantly inhibited NLRP3 inflammasome activation in both THP-1 derived macrophages and bone-marrow derived macrophages, as indicated by reduced expression of NLRP3 and cleaved caspase-1, and lowered IL-1β secretion. Finally, compound 1-induced NLRP3 inflammasome inhibition is through blocking NLRP3 priming step and dependent on Nrf2 activation. Taken together, our findings demonstrate that compound 1 might be a potential agent for the treatment of IBD by targeting Nrf2 and NLRP3 inflammasome.
Titanium dioxide nanoparticles (Nano-TiO2) are widely used to additives in cosmetics, pharmaceutical, paints and foods. Recent studies have demonstrated that Nano-TiO2 induces DNA damage and increased the risk of cancer and the mechanism might relate with oxidative stress. The aim of this study was to evaluate the effects of Nuclear factor erythroid 2 (NF-E2)-related factor 2 (Nrf2), an anti-oxidative mediator, on DNA damage induced by Nano-TiO2. Wildtype, Nrf2 knockout (Nrf2(-/-)) and tert-butylhydroquinone (tBHQ) pre-treated HepG2 cells and mice were treated with Nano-TiO2. And then the oxidative stress and DNA damage were evaluated. Our data showed that DNA damage, reactive oxygen species (ROS) generation and MDA content in Nano-TiO2 exposed cells were significantly increased than those of control in dose dependent manners. Nrf2/ARE droved the downstream genes including NAD(P)H dehydrogenase [quinine] 1(NQO1), heme oxygenase 1 (HO-1) and glutamate-cysteine ligase catalytic subunit (GCLC) expression were significantly higher in wildtype HepG2 cells after Nano-TiO2 treatment. After treatment with Nano-TiO2, the DNA damages were significantly increased in Nrf(-/-) cells and mice whereas significantly decreased in tBHQ pre-treatment cells and mice, compared with the wildtype HepG2 cells and mice, respectively. Our results indicated that the acquired of Nrf2 leads to a decreased susceptibility to DNA damages induction by Nano-TiO2 and decreasing of risk of cancer which would provide a strategy for a more efficacious sensitization of against of Nano-TiO2 toxication.
Foxtail millet (Setaria italica) is the sixth most important cereal in the world. In particular, the millet-derived active components play important roles in disease prevention. In this study, we found that a peroxidase from foxtail millet bran, named FMBP, displayed profound inhibitory effects on the growth of human colon cancer cells, but not on that of the normal colon epithelial cells. Mechanistic investigations suggested that the selective anti-cancer effects of FMBP were mainly achieved by inducing more accumulation of reactive oxygen species (ROS) in colon cancer cells than normal cells. The preferential ROS accumulation in cancer cells by FMBP appears to be partially attributed to the down-regulation of NF-E2-related factor 2 (Nrf2) expression, and the reduction of catalase activities and glutathione contents. The increased ROS accumulation is speculated to block the STAT3 signaling pathway, which results in the anti-proliferative effects on colon cancer cells. Therefore, these results suggest that the millet bran-derived peroxidase has a therapeutic potential in the management of colon cancer.
Carbon tetrachloride (CCl4)-induced hepatotoxicity is a common syndrome with simultaneous severe hepatocyte death and acute cholestasis. The purpose of the present study is to investigate the hepatoprotective effect of alisol B 23-acetate (AB23A), a natural triterpenoid from edible botanical Rhizoma alismatis, on acute hepatotoxicity induced by CCl4 in mice, and further to elucidate the involvement of farnesoid X receptor (FXR), signal transducers and activators of transcription 3 (STAT3) in the hepatoprotective effect. H&E staining, BrdU immunohistochemistry and TUNEL assay were used to identify the amelioration of histopathological changes, hepatocyte proliferation and apoptosis. Real-time PCR and western blot assay were used to elucidate the mechanisms underlying AB23A hepatoprotection. The results indicated that AB23A treatment in a dose-dependent manner resulted in protection against hepatotoxicity induced by CCl4via FXR activation. Through FXR activation, AB23A promoted hepatocyte proliferation via an induction in hepatic levels of FoxM1b, Cyclin D1 and Cyclin B1. AB23A also reduced hepatic bile acids through a decrease in hepatic uptake transporter Ntcp, bile acid synthetic enzymes Cyp7a1, Cyp8b1, and an increase in efflux transporter Bsep, Mrp2 expression. In addition, AB23A induced the expression of STAT3 phosphorylation, and STAT3 target genes Bcl-xl and SOCS3, resulting in decreased hepatocyte apoptosis. In conclusion, AB23A produces a protective effect against CCl4-induced hepatotoxicity, due to FXR and STAT3-mediated gene regulation.
p,p'-dichlorodiphenyldichloroethylene (p,p'-DDE), the major isomer of persistent 1,1-Bis(4-chlorophenyl)-2,2,2-trichloroethane metabolite, is highly associated with the risk of liver cancer. γ-glutamyl-cysteine synthetase (γ-GCS), which is the rate-limiting enzyme of glutathione (GSH) biosynthesis and an important scavenger of reactive oxygen species (ROS), is considered as a potential therapeutic target for many cancers. However, the association between the body burden of p,p'-DDE and γ-GCS has not been fully established. Here, we indicated that low doses of p,p'-DDE exposure promoted the proliferation and decreased γ-GCS activity of HepG2 cells in a dose- and time-dependent manner. In addition, p,p'-DDE elevated ROS content and attenuated glutathione peroxidase activity. This was accompanied with inhibitions of NF-E2-related factor 2 (Nrf2) at the mRNA and protein levels. ROS inhibitor supplement could significantly reverse these effects. Moreover, the addition of the proteasome inhibitor, MG132, strongly reversed the p,p'-DDE-reduced Nrf2 expression and γ-GCS activity. Consistently, GSH content was in line with the alteration of γ-GCS. Collectively, the results indicate that p,p'-DDE treatment downregulates γ-GCS activity in HepG2 cells by inducing ROS-mediated Nrf2 loss.
Regulating inflammation could be an important measure for the effective treatment of cancer. Here we examine the mechanisms by which oroxylin A inhibits inflammation in RAW264.7 cells. The results demonstrate that pretreatment with oroxylin A (50, 100, and 150 μmol/L) inhibited lipopolysaccharide (LPS)-induced mRNA and protein expression of COX-2 and iNOS. In addition, oroxylin A significantly increased the protein expression of nuclear factor erythroid 2-related factor 2 (Nrf2), heme oxygenase 1 (HO-1), and NADP(H):quinone oxidoreductase (NQO1), induced Nrf2 translocation to the nucleus and up-regulated antioxidant response element (ARE)-luciferase reporter activity. Moreover, oroxylin A inhibited Nrf2 ubiquitination and proteasome activity. Transfection with Nrf2 siRNA knocked down Nrf2 expression and partially reversed oroxylin A-mediated inhibition of LPS-induced COX-2 and iNOS expression. Importantly, we showed for the first time that Nrf2 plays an important role in oroxylin A-suppressed inflammation in RAW264.7 cells. Uncovering the effect of oroxylin A on the regulation of Nrf2 signaling may be beneficial for developing new therapeutic strategies against inflammatory diseases.
The mechanism of blue light-induced retinal ganglion cell (RGC) injury is poorly understood. In this study, we established a patented light-emitting diode-based system to study the effects of long-term blue light exposure under culture conditions on RGC-5 cells. Long-term blue light exposure significantly reduced cell viability in a time-dependent manner and induced apoptosis and necrosis in RGC-5 cells. Long-term blue light exposure marked an increase in the expression of Bax and active Caspase-3 (p17), which was accompanied by Bcl-2 down-regulation, and displayed features of the mitochondria-dependent apoptosis pathway. Blue light exposure also increased the generation of reactive oxygen species (ROS), and was a strong inducer of ROS-sensitive protein nuclear factor erythroid 2-related factor 2 (Nrf2) and heme oxygenase-1 (HO-1) expression. Moreover, blue light exposure constitutively activated p38 mitogen-activated protein kinases and c-Jun NH2-terminal kinase (JNK), as well as induced the phosphorylation of extracellular signal-regulated kinase in the early phase, in blue light-exposed RGC-5 cells. The protein expression of c-jun and c-fos was further enhanced after RGC-5 cells were exposed to blue light. Taken together, these findings indicated that blue light induced RGC-5 cell line death in dependence upon exposure duration. The potential mechanisms for this phenomenon might be via activated mitochondria-dependent apoptosis, increased ROS production and protein expressions of Nrf2 and HO-1, and activated JNK/p38 MAPK signaling pathways.
Cancer cells, compared with normal cells, are under increased oxidative stress with higher level of reactive oxygen species (ROS). When exposed to environmental stresses such as ROS, NFE-related factor 2 (Nrf2) is the key to antioxidant response by transcriptionally activating various detoxification and antioxidant enzymes. Previously, we have shown that wogonin, a flavonoid isolated from the root of Scutellaria baicalensis Georgi, could reverse drug resistance in MCF-7/DOX cells by blocking the translocation of Nrf2 into nucleus. However, the exact mechanism underlying the effect remains unclear. In this study, we observed that wogonin reduced the Nrf2 nuclear translocation, and therefore elevated the level of intracellular ROS to accomplish the purpose of killing malignant cells. Furthermore, the suppression of Nrf2 by wogonin can potentiate cytotoxic effects of chemotherapeutic agents in HepG2 cells. On one hand, down-regulation of Nrf2 lead to reduction of cytoprotective effect by inducing phage II enzymes which sensitize cells to chemotherapeutic agents. On the other hand, inhibition of multidrug resistance-associated proteins (MRPs) by wogonin enhances the effective drug level in cancer cells and potentiates their chemotherapeutic effects. Finally, we found that the decrease of Nrf2 may be related to overexpression of p53. Using p53 siRNA to knock down the endogenous p53 expression, the levels of both c-myc and Nrf2 in nucleus increased when exposed to wogonin. The present study indicates that wogonin can be used in chemotherapy not only because of its own antitumor ability, but also due to the enhanced cytotoxic effects of chemotherapeutic agents.
Pulmonary hypertension is a progressive disease characterized by marked pulmonary arterial remodeling and increased vascular resistance. Inflammation and oxidative stress promote the development of pulmonary hypertension. Oxymatrine, one of the main active components of the Chinese herb Sophora flavescens Ait. (Kushen), plays anti-inflammatory and antioxidant protective roles, which effects on pulmonary arteries remain unclear. This study aimed to investigate the effects of oxymatrine on pulmonary hypertension development. Sprague-Dawley rats were exposed to hypoxia for 28 days or injected with monocrotaline, to develop pulmonary hypertension, along with administration of oxymatrine (50mg/kg/day). Hemodynamics and pulmonary arterial remodeling data from the rats were then obtained. The antiproliferative effect of oxymatrine was verified by in vitro assays. The inflammatory cytokine mRNA levels and leukocyte and T cell accumulation in lung tissue were detected. The antioxidative effects of oxymatrine were explored in vitro. Our study shows that oxymatrine treatment attenuated right-ventricular systolic pressure and pulmonary arterial remodeling induced by hypoxia or monocrotaline and inhibited proliferation of pulmonary arterial smooth muscle cells (PASMCs). Increased expression of inflammatory cytokine mRNA and accumulation of leukocytes and T cells around the pulmonary arteries were suppressed with oxymatrine administration. Under hypoxic conditions, oxymatrine significantly upregulated Nrf2 and antioxidant protein SOD1 and HO-1 expression, but downregulated hydroperoxide levels in PASMCs. In summary, this study indicates that oxymatrine may prevent pulmonary hypertension through its antiproliferative, anti-inflammatory, and antioxidant effects, thus providing a promising pharmacological avenue for treating pulmonary hypertension.
(S)-ZJM-289, a novel nitric oxide (NO)-releasing derivative of 3-n-butylphthalide, induces the neuroprotection in a rat model of focal cerebral ischemia/reperfusion (I/R). However, much is unknown about the late phase effect in the neuroprotection of (S)-ZJM-289 preconditioning. The purpose of this study is to explore the late phase neuroprotection of (S)-ZJM-289 preconditioning, as well as underlying mechanisms involved. Preconditioning with 40-160 mg/kg, (S)-ZJM-289 significantly reduces brain damage after I/R. (S)-ZJM-289 preconditioning is effective when applied 1-3 days before I/R. Moreover, the degrees of neuroprotection offered by (S)-ZJM-289 preconditioning and ischemic preconditioning are virtually identical. (S)-ZJM-289 preconditioning also protects primary cultured cortical neurons against oxygen-glucose deprivation and recovery-induced cytotoxicity in vitro. (S)-ZJM-289 preconditioning significantly increases the generation of NO, but has no effect on the nitric oxide synthase activities. Additionally, (S)-ZJM-289 preconditioning promotes the dissociation between nuclear-factor-E2-related factor (Nrf2) and kelch-like ECH-associated protein 1, and induces Nrf2 nuclear localization. The neuroprotection of (S)-ZJM-289 preconditioning is blocked by Nrf2-siRNA in vitro. (S)-ZJM-289 preconditioning up-regulates antioxidant enzymes against nervous injury. (S)-ZJM-289 preconditioning significantly activates extracellular regulated protein kinases (ERK) and inhibits c-Jun N-terminal kinases signaling cascade. The neuroprotection is abolished by the ERK inhibitor PD98059 in vitro. Subsequently, (S)-ZJM-289 preconditioning increases the levels of anti-apoptotic protein B cell lymphoma 2 (Bcl-2) and inhibited the translocation of Bcl-2 associated X to the mitochondria, thus attenuating the release of cytochrome c from the mitochondria and the activation of downstream caspase. These results suggest that (S)-ZJM-289 preconditioning exerts the late phase protection against nervous injury induced by transient cerebral ischemia and oxygen-glucose deprivation.
Nrf2-mediated activation of ARE regulates expression of cytoprotective enzymes against oxidative stress, inflammation, and carcinogenesis. We have discovered a novel structure (1) as an ARE inducer via luciferase reporter assay to screen the in-house database of our laboratory. The potency of 1 was evaluated by the expression of NQO-1, HO-1, and nuclear translocation of Nrf2 in HCT116 cells. In vivo potency of 1 was studied using AOM-DSS models, showing that the development of colorectal adenomas was significantly inhibited. Administration with 1 lowered the expression of IL-6, IL-1β, and promoted Nrf2 nuclear translocation. These results indicated that 1 is a potent Nrf2/ARE activator, both in vitro and in vivo. Forty-one derivatives were synthesized for SAR study, and a more potent compound 17 was identified. To our knowledge, this is a potent ARE activator. Besides, its novel structure makes it promising for further optimization.
Peroxiredoxin 6 (Prx 6) is a bifunctional enzyme with both glutathione peroxidase and acidic Ca(2+)-independent phospholipase A(2) activities. We have recently shown that exposure of murine bone marrow-derived macrophages to LPS and IFN-γ leads to induction of COX-2 expression and secretion of PGE(2), up-regulating Prx 6 mRNA levels. This study was designed to investigate various prostaglandins (PGs) for their ability to induce gene expression of Prxs, in particular Prx 6, and to determine the underlying regulatory mechanisms. We provide evidence that both conventional and cyclopentenone PGs enhance Prx 6 mRNA expression. Treatment with either activators or inhibitors of adenylate cyclase as well as cAMP analogs indicated that Prx 6 gene expression is regulated by adenylate cyclase in response to PGD(2) or PGE(2). Furthermore, our study revealed that JAK2, PI3K, PKC, and p38 MAPK contribute to the PGD(2)- or PGE(2)-dependent Prx 6 induction. Using stimulated macrophages from Nrf2-deficient mice or activators of Nrf2 and PPARγ, we found that Nrf2, but not PPARγ, is involved in the PG-dependent increase in Prx 6 mRNA expression. In summary, our data suggest multiple signaling pathways of Prx 6 regulation by PGs and identified Nrf2 as a critical player mediating transcriptional induction.
The aim of this study was to investigate whether BML-111 can exert protective effects on cerulein-induced acute pancreatitis-associated lung injury (APALI) via activation of nuclear factor erythroid 2-related factor 2 (Nrf2)/antioxidant responsive element (ARE) signaling pathway. Severe acute pancreatitis (SAP) was established by intraperitoneal injection of cerulein (50 μg/kg) seven times at hourly intervals and Escherichia coli lipopolysaccharide (10 mg/kg) once after the last dose of cerulein immediately. BML-111 (1 mg/kg) was administered 1 h before the first injection of cerulein. Samples were taken at 3, 6, 12, and 24 h after the last injection. Pathologic lesions of the pancreas and lung tissues as well as the levels of serum amylase were analyzed; Myeloperoxidase (MPO), malondialdehyde (MDA), superoxide dismutase (SOD), Nrf2, heme oxygenase-1 (HO-1), and
NAD(P)H:
quinone oxidoreductase-1 (NQO1) of lung tissue were determined. The findings revealed that the injuries of pancreas and lung were typically induced by cerulein. The administration of BML-111 reduced the levels of serum amylase, lung MPO, lung MDA, the wet-to-dry weight ratio, and the pathology injury scores of the lung and pancreas, which increased in the SAP group. The expressions of Nrf2, HO-1, NQO1, and activity of SOD in lung tissue increased in the BML-111 group compared with those in the SAP group. This study indicates that BML-111 may play a critical protective role in APALI induced by cerulein. The underlying mechanisms of protective role may be attributable to its antioxidant effects through the activation of Nrf2/ARE pathway.
ETHNOPHARMACOLOGICAL RELEVANCE:
Baicalein (BE), a phenolic flavonoid extracted mainly from the root of Scutellaria baicalensis Georgi, a Chinese herb, is traditionally used in oriental medicine. Several studies have demonstrated that BE exerts many beneficial effects including anti-inflammatory and antioxidant activities. However, its effect on acute lung injury (ALI) and the molecular mechanisms involved remain unclear and warrant further investigation. The aim of the study is to investigate whether BE improves lipopolysaccharide (LPS, intratracheally, i.t.)-induced ALI in rats, and further study the underlying mechanisms of its activity.
MATERIAL AND METHODS:
Rats were administrated with LPS (5mg/kg/body weight, i.t.) through a 24-gauge catheter to establish the ALI model. The effects of BE on the levels of pro-inflammatory cytokines, nitrite/nitrate in bronchoalveolar lavage fluid, and the expression of nuclear factor-erythroid 2-related factor 2 (Nrf2), heme oxygenase-1 (HO-1) and nuclear factor-kappa B (NF-κB) activation as well as the histopathological changes were evaluated.
RESULTS:
Results showed that BE (20mg/kg, i.p.) treatment markedly attenuated LPS-induced lung edema, elevation of the levels of IL-1β, TNF-α, IL-6, CINC-3, and nitrite/nitrate in bronchoalveolar lavage fluid accompanied by a remarkable improvement of lung histopathological symptoms. The LPS-enhanced inflammatory cell infiltration and myeloperoxidase activity, O2(-) formation and the expression of inducible nitric oxide synthase and nitrotyrosin in lungs were all attenuated by BE. Notably, BE could augment Nrf2/HO-1 cascade, but inhibited NF-κB activation in LPS-instilled lungs that was strongly reversed by blocking HO-1 activity.
CONCLUSION:
This study is the first to demonstrate that BE protects against LPS-induced ALI in rats. The underlying mechanisms may include inhibition of NF-κB-mediated inflammatory responses and upregulation of Nrf2/HO-1 pathway, which ultimately alleviates the pathological symptoms of ALI.
Copyright © 2014 Elsevier Ireland Ltd. All rights reserved.
OBJECTIVE:
Myocardial infarction (MI) is a cause of high morbidity and mortality in the world. Sodium tanshinone IIA sulphonate (STS) has been well used in Oriental medicine for treating cardiovascular diseases, however, the underlying mechanisms remain unclear. Alterations of circulating lipid profiles, increased fatty acid β-oxidation and oxidative stress play most important roles in the pathogenesis of MI. The present study aims to elucidate whether STS possesses cardioprotective effect against MI driven by isoproterenol (ISO), and to investigate its potential mechanisms of action.
METHODS:
MI was induced by subcutaneous injection of ISO (85 mg/kg at interval of 24 h for 2 consecutive days) to rats. The rats were randomly divided into 6 groups: (1) control; (2) ISO; (3) STS (16 mg/kg) +control; (4-6) STS (16, 8, 4 mg/kg) +ISO.
RESULTS:
Our study showed that STS could ameliorate cardiac dysfunction and variation of myocardial zymogram, up-regulate antioxidant systems, and maintain the levels of circulating lipids driven by supramaximal doses ISO as well. Moreover, modulation of redox-sensitive extracellular signal-regulated kinase1/2 (ERK1/2)/Nuclear factor erythroid 2-related factor 2 (Nrf2)/heme oxygenase-1 (HO-1) and AMP-activated protein kinase (AMPK)/acetyl CoA carboxylase (ACC)/carnitine palmitoyltransferase (CPT) 1 pathways were involved in STS induced cardioprotection.
CONCLUSIONS:
STS exerts strong favorable cardioprotective action. Additionally, the properties of STS, such as anti-dyslipidemia, anti-oxidant and inhibition of fatty acid β-oxidation, may be the mechanisms underlying the observed results.
© 2013 Elsevier Ireland Ltd. All rights reserved.
PURPOSE:
As hypertension (HT) is one of the risk factors for lower urinary tract symptoms, we investigated the effect of an angiotensin II type I receptor blocker, olmesartan, on bladder dysfunction in the spontaneously hypertensive rat (SHR).
MATERIALS AND METHODS:
Twelve-week-old male SHRs were administered perorally with olmesartan (0, 1, or 3 mg/kg/day) or nifedipine (30 mg/kg/day) for 6 weeks. Wistar rats were used as normotensive controls. The effects of olmesartan or nifedipine on blood pressure (BP), bladder blood flow (BBF), urodynamic parameters, tissue levels of malondialdehyde (MDA), nuclear factor erythroid 2-related factor 2 (Nrf2), and nerve growth factor (NGF) were measured in the bladder. Localization of 4-hydroxy-2-nonenal (4-HNE), Nrf2, and NGF in the bladder was shown by immunohistochemistry.
RESULTS:
The SHRs showed significant increase in BP, micturition frequency, and expression of MDA, 4-HNE, Nrf2, and NGF when compared to the control Wistar rats. Conversely, there was a decrease in BBF and single voided volume in SHRs when compared to Wistar rats. Treatment with olmesartan and nifedipine significantly improved BP. However, only olmesartan significantly ameliorated urodynamic parameters and oxidative damage compared to the non-treated SHR. The immunoreactivities of 4-HNE, Nrf2, and NGF in SHR urothelium and blood vessels were increased compared to the control. Treatment with a high dose of olmesartan decreased the expressions of 4-HNE, Nrf2, and NGF in the bladder.
CONCLUSION:
Our data suggest that BP, BBF, and oxidative stress may be responsible for the functional changes in HT-related bladder dysfunction. Olmesartan significantly ameliorated this bladder dysfunction.
© 2013 Wiley Periodicals, Inc.
![Western Blot - Anti-Nrf2 Antibody [ARC50393] (A308758) - Antibodies.com](https://cdn.antibodies.com/image/catalog/308/A308758_1.jpg?profile=product_alternative)
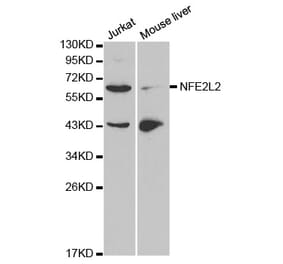
![Western Blot - Anti-Nrf2 Antibody [ARC50393] (A308758) - Antibodies.com](https://cdn.antibodies.com/image/catalog/308/A308758_1.jpg?profile=product_alternative)