![Immunocytochemistry - Anti-Vimentin Antibody [VI-10] (A86650) - Antibodies.com](https://cdn.antibodies.com/image/catalog/86/A86652_789.jpg?profile=product_alternative)
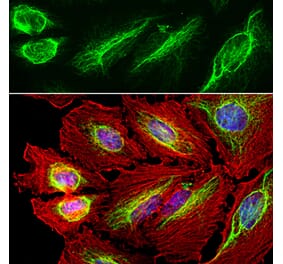
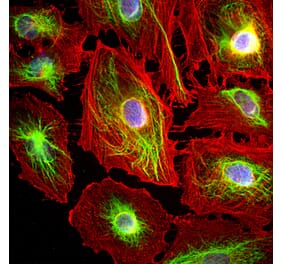
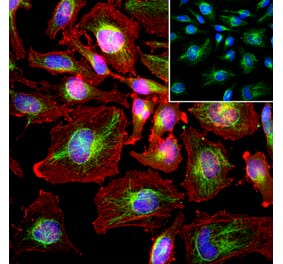
![Immunocytochemistry - Anti-Vimentin Antibody [VI-10] (A86650) - Antibodies.com](https://cdn.antibodies.com/image/catalog/86/A86652_789.jpg?profile=product_alternative)



Unconjugated
Research on the relationship between aberrant long non-coding RNA (lncRNA) and cancer stem cell (CSC) biology in cancer patients has been recently gaining attention. The goal of this study was to investigate whether the decreasing lncRNA HOTAIR expression would inhibit human colorectal cancer (CRC) stem cells. CD133(+)CSCs were isolated from human CRC LoVo cell line by using a magnetic-activated cell sorting system, and were transfected with the expression vector-based small hairpin RNA targeting HOTAIR (shHOTAIR). The ability of cellular proliferation, migration, invasion, colony-forming, and the epithelial-mesenchymal transition (EMT)-associated molecule expression as well as the tumorigenicity of CD133(+)-shHOTAIR were evaluated by the MTT, wound-healing, cellular invasion, colony formation and Western blot assays, respectively. This study found that, when compared with control cells in vitro, CD133(+)-shHOTAIR exhibited the decreased HOTAIR expression, suppressed cellular proliferation, migration, invasion, colony-forming, and inhibited the Vimentin expression with increased E-cadherin expression. In particular, the down-regulation of the HOTAIR expression in CD133(+)CSCs markedly attenuated the tumor growth and lung metastasis in xenograft nude mice. Taken together, this study found that down-regulating the HOTAIR expression in CD133(+)CSCs could serve as a potential anti-cancer regimen to inhibit the invasiveness and metastasis of CRC CSCs.
Apobec-1 complementation factor (A1CF) is a member of the heterogeneous nuclear ribonucleoproteins (hnRNP) family, which participates in site-specific posttranscriptional RNA editing of apolipoprotein B (apoB) transcript. The posttranscriptional editing of apoB mRNA by A1CF in the small intestine is required for lipid absorption. Apart from the intestine, A1CF mRNA is also reported to be highly expressed in the kidneys. However, it is remained unknown about the functions of A1CF in the kidneys. The aim of this paper is to explore the potential functions of A1CF in the kidneys. Our results demonstrated that in C57BL/6 mice A1CF was weakly expressed in embryonic kidneys from E15.5dpc while strongly expressed in mature kidneys after birth, and it mainly existed in the tubules of inner cortex. More importantly, we identified A1CF negatively regulated the process of epithelial-mesenchymal transition (EMT) in kidney tubular epithelial cells. Our results found ectopic expression of A1CF up-regulated the epithelial markers E-cadherin, and down-regulated the mesenchymal markers vimentin and α-smooth muscle actin (α-SMA) in NRK52e cells. In addition, knockdown of A1CF enhanced EMT contrary to the overexpression effect. Notably, the two A1CF variants led to the similar trend in the EMT process. Taken together, these data suggest that A1CF may be an antagonistic factor to the EMT process of kidney tubular epithelial cells.
CUL4A, a member of the CULLIN family, functions as a scaffold protein for an E3 ubiquitin ligase. It was reported that the CUL4A gene showed amplification in some human primary hepatocellular carcinomas (HCC). However, the exact role of CUL4A in HCC remains unknown. Here, we aimed to investigate the expression and function of CUL4A in HCC development. Through immunohistochemistry study, we showed increased CUL4A expression in HCC tissues. Statistical analysis disclosed an inverse correlation between CUL4A expression and tumor differentiation grade, and patient survival, but a positive correlation with hepatocyte proliferation as well as lymphatic and venous invasion. CUL4A expression in HCC tissues was associated with HBeAg status in patients and upregulated by HBV in HCC cell lines. Further functional assay showed that CUL4A overexpression significantly promoted growth of H22 tumor homografts in BALB/c mice. Consistently, CUL4A knockdown inhibited the proliferation of established HCC cells, accompanied by S-phase reduction and Cyclin A and Cyclin B1 repression. Furthermore, CUL4A siRNA ameliorated the motility of HCC cell lines with altered expression of epithelial-mesenchymal transition (EMT)-associated molecules. Taken together, our findings indicate that CUL4A plays a pivotal role in HCC progression and may serve as a potential marker for clinical diagnosis and target for therapy.
Bone marrow stroma plays a critical role in the bone metastasis of breast cancer. Bone marrow-derived mesenchymal stem cells (BMSC) are critical to facilitate cancer progression. Human bone morphogenetic protein 9 (BMP9) is the most potent osteogenic factor and one of bone-stored growth factors involved in both promotion and inhibition of different cancers. However, it is unclear whether BMP9 correlates with the bone metastasis of breast cancer. This study was to evaluate the role of BMP9 in the interaction between BMSC and breast cancer cells (BCC). To determine whether BMP9 is able to block the tumor promoting effect of BMSC, an in vitro model was developed using breast cancer MDA-MB-231 cells co-cultured with bone marrow-derived mesenchymal stem cells HS-5 with-BMP9 overexpression. The expressions of metastasis-related genes were detected to identify important factors mediating the role of BMP9 in breast cancer cells. Results showed BMP9 could inhibit invasion and promote apoptosis of MDA-MB-231 cells. The expressions of interleukin-6 (IL-6), matrix metalloproteinase-2 (MMP-2) and monocyte chemoattratctant protein-1 (MCP-1) decreased in the MDA-MB-231 cells of BMP9 over-expression group, and the expressions of epithelial-mesenchymal transition (EMT)-related molecules was also reduced. On the other hand, the expression of stromal cell derived factor-1 (SDF-1) decreased in HS-5 cells of BMP9 over-expression group. Taken together, BMP9 is able to inhibit the migration and promote the apoptosis of breast cancer by regulating the interaction between MDA-MB-231 cells and HS-5 cells in which SDF-1/CXCR4-PI3K pathway and EMT are involved.
Gastric cancer (GC) is the fourth most common malignancy in males and the fifth most common malignancy in females worldwide. DACH1 is frequently methylated in hepatic and colorectal cancer. To further understand the regulation and mechanism of DACH1 in GC, eight GC cell lines, eight cases of normal gastric mucosa, 98 cases of primary GC and 50 cases of adjacent non-tumour tissues were examined. Methylation-specific PCR, western blot, transwell assay and xenograft mice were used in this study. Loss of DACH1 expression correlated with promoter region methylation in GC cells, and re-expression was induced by 5-Aza-2'-deoxyazacytidine. DACH1 is methylated in 63.3% (62/98) of primary GC and 38% (19/50) of adjacent non-tumour tissues, while no methylation was found in normal gastric mucosa. Methylation of DACH1 correlated with reduced expression of DACH1 (P < 0.01), late tumour stage (stage III/IV) (P < 0.01) and lymph node metastasis (P < 0.05). DACH1 expression inhibited epithelial-mesenchymal transition and metastasis by inhibiting transforming growth factor (TGF)-β signalling and suppressed GC cell proliferation through inducing G2/M phase arrest. The tumour size is smaller in DACH1-expressed BGC823 cell xenograft mice than in unexpressed group (P < 0.01). Restoration of DACH1 expression also sensitized GC cells to docetaxel. These studies suggest that DACH1 is frequently methylated in human GC and expression of DACH1 was controlled by promoter region methylation. DACH1 suppresses GC proliferation, invasion and metastasis by inhibiting TGF-β signalling pathways both in vitro and in vivo. Epigenetic silencing DACH1 may induce GC cells' resistance to docetaxel.
Transcatheter arterial embolization (TAE) is widely used as an effective palliative treatment for hepatocellular carcinoma (HCC), and can prolong survival time. However, the high incidence of tumor recurrence and metastasis after TAE is still a major problem. Recent studies demonstrated that circulating tumor cells (CTCs) contribute to tumor metastasis. In this study, we tried to clarify whether the residual HCC after TAE can increase metastasis by increasing the number of CTCs. An orthotopic liver tumor model in the Buffalo rat was established using green fluorescent protein (GFP)-transfected HCC cell line, McA-RH7777. Two weeks after orthotopic liver tumor implantation, the rats underwent TAE treatment from the gastroduodenal artery. Iodized oil or saline was injected intra-arterially. Blood samples were taken on day 0, 1, 3, 7, 14, and 21 for detection of CTCs after TAE treatment. We analyzed the number of CTCs and assessed the metastatic potential of surviving tumor cells in rats between TAE and control groups. Our results demonstrated that the metastatic colonies in the lung were significantly increased by TAE treatment. The number of CTCs was also significantly increased by TAE treatment from day 7 to day 21. The expression of hypoxia-inducible factor (HIF)-1α and epithelial-mesenchymal transition (EMT) marker proteins (N-cadherin and vimentin) was upregulated, but E-cadherin was downregulated after TAE treatment. In conclusion, the metastatic potential of residual HCC can be induced by TAE treatment in a rat liver tumor model, which involves the acquisition of EMT features and an increased number of CTCs.
To explore epigenetic regulation and the impact of chemokine CXCL14 on colorectal cancer, 7 colorectal cancer cell lines, 107 cases of primary colorectal cancer, and 10 cases of normal colorectal mucosa were evaluated in this study. Methylation specific PCR (MSP), semi-quantitative reverse-transcription PCR (RT-PCR), cell proliferation assay, colony formation, and transwell assay were performed for the evaluation. Complete methylation and loss of CXCL14 expression were found in 5 colorectal cancer cell lines. Partial methylation and weak expression were found in two cell lines. CXCL14 was methylated in 79.4% (85/107) of primary human colorectal cancer. No methylation was found in 10 cases of normal colorectal mucosa. Restoration of CXCL14 expression was induced by the 5-aza-2'-deoxycytidine (DAC) treatment. The cell viability was reduced and colony formation was inhibited by restoration of CXCL14 expression in HCT116 cells, a colorectal cancer cell line. The number of invasive and migration cells was reduced by CXCL14. The expression of MMP-2, Vimentin, and NF-κB was suppressed, and the expression of E-cadherin and IκB-α was induced by CXCL14. In conclusion, CXCL14 is frequently methylated in human colorectal cancer and promoter region hypermethylation silenced CXCL14 expression in colorectal cancer cells. Restoration of CXCL14 expression suppressed colorectal cancer proliferation. CXCL14 inhibits colorectal cancer migration, invasion, and epithelial-to-mesenchymal transition (EMT) by suppressing NF-κB signaling.
Hepatocellular carcinoma (HCC) is one of the most malignant tumors and the biggest obstacle in curing HCC is its high metastasis potential. Alteration of p53 is the most frequent genetic change found in HCC. Although the biological function of p53 in tumor initiation and progression has been well characterized, whether or not p53 is implicated in metastasis of HCC is largely unknown. In this study, we analyzed the potential functions of p53 in epithelial-mesenchymal transition (EMT) and metastasis of HCC cells. Both insulin- and TGF-β1-induced changes of critical EMT markers were greatly enhanced by p53 knockdown in HCC cells. The insulin- and TGF-β1-stimulated migration of HCC cells were enhanced by p53 knockdown. Furthermore, in vivo metastasis of HCC cells using different mouse models was robustly enhanced by p53 knockdown. In addition, we found that p53 regulation on EMT and metastasis involves β-catenin signaling. The nuclear accumulation and transcriptional activity of β-catenin was modulated by p53. The enhanced EMT phenotype, cell migration and tumor metastasis of HCC cells by p53 knockdown were abrogated by inhibiting β-catenin signal pathway. In conclusion, this study reveals that p53 plays a pivotal role in EMT and metastasis of HCC cells via its regulation on β-catenin signaling.
MicroRNAs (miRNAs) play a critical role in tumor metastasis. In this study, we identified a set of 32 miRNAs involved in hepatocellular carcinoma (HCC) metastasis. Among them, miR-612 was shown for the first time to have inhibitory effects on HCC proliferation, migration, invasion, and metastasis. AKT2 was verified to be one of the direct targets of miR-612, through which the epithelial-mesenchymal transition (EMT) and metastasis were inhibited. The level of miR-612 in HCC patients was inversely associated with tumor size, stage, EMT, and metastasis. Of particular importance, miR-612 is involved in both the initial and final steps of the metastatic cascade, by suppressing local invasion and distant colonization. The pleiotropic roles of miR-612 in the HCC metastatic cascade suggest that it could be an effective target for both early and advanced HCC.
BACKGROUND:
Emerging evidence indicates that inappropriate cell-cell fusion might contribute to cancer progression. Similarly, mesenchymal stem cells (MSCs) can also fuse with other cells spontaneously and capable of adopting the phenotype of other cells. The aim of our study was to investigate the role of MSCs participated cell fusion in the tumorigenesis of gastric cancer.
METHODS:
We fused human umbilical cord mesenchymal stem cells (hucMSCs) with gastric cancer cells in vitro by polyethylene glycol (PEG), the hybrid cells were sorted by flow cytometer. The growth and migration of hybrids were assessed by cell counting, cell colony formation and transwell assays. The proteins and genes related to epithelial- mesenchymal transition and stemness were tested by western blot, immunocytochemistry and real-time RT-PCR. The expression of CD44 and CD133 was examined by immunocytochemistry and flow cytometry. The xenograft assay was used to evaluation the tumorigenesis of the hybrids.
RESULTS:
The obtained hybrids exhibited epithelial- mesenchymal transition (EMT) change with down-regulation of E-cadherin and up-regulation of Vimentin, N-cadherin, α-smooth muscle actin (α-SMA), and fibroblast activation protein (FAP). The hybrids also increased expression of stemness factors Oct4, Nanog, Sox2 and Lin28. The expression of CD44 and CD133 on hybrid cells was stronger than parental gastric cancer cells. Moreover, the migration and proliferation of heterotypic hybrids were enhanced. In addition, the heterotypic hybrids promoted the growth abilities of gastric xenograft tumor in vivo.
CONCLUSIONS:
Taken together, our results suggest that cell fusion between hucMSCs and gastric cancer cells could contribute to tumorigenic hybrids with EMT and stem cell-like properties, which may provide a flexible tool for investigating the roles of MSCs in gastric cancer.
INTRODUCTION:
Acquired tamoxifen resistance remains the major obstacle to breast cancer endocrine therapy. β1-integrin was identified as one of the target genes of G protein-coupled estrogen receptor (GPER), a novel estrogen receptor recognized as an initiator of tamoxifen resistance. Here, we investigated the role of β1-integrin in GPER-mediated tamoxifen resistance in breast cancer.
METHODS:
The expression of β1-integrin and biomarkers of epithelial-mesenchymal transition were evaluated immunohistochemically in 53 specimens of metastases and paired primary tumors. The function of β1-integrin was investigated in tamoxifen-resistant (MCF-7R) subclones, derived from parental MCF-7 cells, and MCF-7R β1-integrin-silenced subclones in MTT and Transwell assays. Involved signaling pathways were identified using specific inhibitors and Western blotting analysis.
RESULTS:
GPER, β1-integrin and mesenchymal biomarkers (vimentin and fibronectin) expression in metastases increased compared to the corresponding primary tumors; a close expression pattern of β1-integrin and GPER were in metastases. Increased β1-integrin expression was also confirmed in MCF-7R cells compared with MCF-7 cells. This upregulation of β1-integrin was induced by agonists of GPER and blocked by both antagonist and knockdown of it in MCF-7R cells. Moreover, the epidermal growth factor receptor/extracellular regulated protein kinase (EGFR/ERK) signaling pathway was involved in this transcriptional regulation since specific inhibitors of these kinases also reduced the GPER-induced upregulation of β1-integrin. Interestingly, silencing of β1-integrin partially rescued the sensitivity of MCF-7R cells to tamoxifen and the α5β1-integrin subunit is probably responsible for this phenomenon. Importantly, the cell migration and epithelial-mesenchymal transition induced by cancer-associated fibroblasts, or the product of cancer-associated fibroblasts, fibronectin, were reduced by knockdown of β1-integrin in MCF-7R cells. In addition, the downstream kinases of β1-integrin including focal adhesion kinase, Src and AKT were activated in MCF-7R cells and may be involved in the interaction between cancer cells and cancer-associated fibroblasts.
CONCLUSIONS:
GPER/EGFR/ERK signaling upregulates β1-integrin expression and activates downstream kinases, which contributes to cancer-associated fibroblast-induced cell migration and epithelial-mesenchymal transition, in MCF-7R cells. GPER probably contributes to tamoxifen resistance via interaction with the tumor microenvironment in a β1-integrin-dependent pattern. Thus, β1-integrin may be a potential target to improve anti-hormone therapy responses in breast cancer patients.
BACKGROUND:
The epithelial-to-mesenchymal transition (EMT) is a key process in carcinogenesis, invasion, and metastasis of oral squamous cell carcinoma (OSCC). In our previous studies, we found that neuropilin-1 (NRP1) is overexpressed in tongue squamous cell carcinoma and that this overexpression is associated with cell migration and invasion. Nuclear factor-kappa B (NF-κB) plays an essential role both in the induction and the maintenance of EMT and tumor metastasis. Therefore, we hypothesized that NRP1 induces EMT, and that NRP1-induced migration and invasion may be an important mechanism for promoting invasion and metastasis of OSCC through NF-κB activation.
METHODS/RESULTS:
The variations in gene and protein expression and the changes in the biological behavior of OSCC cell lines transfected with a vector encoding NRP1, or the corresponding vector control, were evaluated. NRP1 overexpression promoted EMT and was associated with enhanced invasive and metastatic properties. Furthermore, the induction of EMT promoted the acquisition of some cancer stem cell (CSC)-like characteristics in OSCC cells. We addressed whether selective inhibition of NF-κB suppresses the NRP1-mediated EMT by treating cells with pyrrolidinedithiocarbamate ammonium (PDTC), an inhibitor of NF-κB. Immunohistochemical analysis of NRP1 in OSCC tissue samples further supported a key mediator role for NRP1 in tumor progression, lymph node metastasis, and indicated that NRP1 is a predictor for poor prognosis in OSCC patients.
CONCLUSION:
Our results indicate that NRP1 may regulate the EMT process in OSCC cell lines through NF-κB activation, and that higher NRP1 expression levels are associated with lymph node metastasis and poor prognosis in OSCC patients. Further investigation of the role of NRP1 in tumorigenesis may help identify novel targets for the prevention and therapy of oral cancers.
BACKGROUND:
MiR-17-92 cluster and its paralogues have emerged as crucial regulators of many oncogenes and tumor suppressors. Transforming growth factor-β receptor II (TGFβR2), as an important tumor suppressor, is involved in various cancer types. However, it is in cancer that only two miRNAs of this cluster and its paralogues have been reported so far to regulate TGFβR2. MiR-93 is oncogenic, but its targetome in cancer has not been fully defined. The role of miR-93 in nasopharyngeal carcinoma (NPC) still remains largely unknown.
METHODS:
We firstly evaluated the clinical signature of TGFβR2 down-regulation in clinical samples, and next used a miRNA expression profiling analysis followed by multi-validations, including Luciferase reporter assay, to identify miRNAs targeting TGFβR2 in NPC. In vitro and in vivo studies were performed to further investigate the effects of miRNA-mediated TGFβR2 down-regulation on NPC aggressiveness. Finally, mechanism studies were conducted to explore the associated pathway and genes influenced by this miRNA-mediated TGFβR2 down-regulation.
RESULTS:
TGFβR2 was down-regulated in more than 50% of NPC patients. It is an unfavorable prognosis factor contributing to clinical NPC aggressiveness. A cluster set of 4 TGFβR2-associated miRNAs was identified; they are all from miR-17-92 cluster and its paralogues, of which miR-93 was one of the most significant miRNAs, directly targeting TGFβR2, promoting cell proliferation, invasion and metastasis in vitro and in vivo. Moreover, miR-93 resulted in the attenuation of Smad-dependent TGF-β signaling and the activation of PI3K/Akt pathway by suppressing TGFβR2, further promoting NPC cell uncontrolled growth, invasion, metastasis and EMT-like process. Impressively, the knockdown of TGFβR2 by siRNA displayed a consentaneous phenocopy with the effect of miR-93 in NPC cells, supporting TGFβR2 is a major target of miR-93. Our findings were also substantiated by investigation of the clinical signatures of miR-93 and TGFβR2 in NPC.
CONCLUSION:
The present study reports an involvement of miR-93-mediated TGFβR2 down-regulation in NPC aggressiveness, thus giving extended insights into molecular mechanisms underlying cancer aggressiveness. Approaches aimed at blocking miR-93 may serve as a promising therapeutic strategy for treating NPC patients.
Snail is closely linked to tumor invasion, metastasis, and recurrence and indicates prognosis of patients suffering from cancer. Overexpression of Snail increases motility and invasiveness of cancer cells, which has become target for anti-metastatic treatment. Oroxylin A, a natural compound extracted from Scutellaria radix, has been reported to inhibit invasion and migration in breast cancer. In this study, we investigated the anti-invasive effect of oroxylin A on lung cells and uncovered its underlying mechanism. The results suggested that oroxylin A could inhibit migration and invasion in Snail-expressing 95-D, and A549 cells whereas it had little effect on non-expressing GLC-82 cells. Furthermore, enhanced Snail expression after transfection of Snail vector in GLC-82 cells is decreased by oroxylin A. Snail can also induce epithelial-mesenchymal transition. We found oroxylin A could reverse TGFβ1-induced epithelial-mesenchymal transition by inhibiting Snail expression. As a result, oroxylin A up-regulated E-cadherin expression and down-regulated vimentin, MMP-9, and CD44v6 expression, which could lead to the inhibition of tumor migration and invasion. Mechanically, we demonstrated that oroxylin A suppressed activation of ERK instead of AKT pathway and then promoted activation of GSK-3β to reduce Snail protein content. Finally, we established transplanted, metastatic, and orthotopic models of A549 cells, and found that oroxylin A inhibited the growth and lung metastasis of A549 cells in vivo. Taken together, we proposed that oroxylin A might be a promising candidate targeting tumor metastasis.
© 2016 Wiley Periodicals, Inc.
Tumor vaccines may induce antitumor efficacy, however, weak immunogenicity of tumor antigens is one of the prime obstacles for excitation of the antitumor immune responses. Therefore, strategies that enhance immunogenicity of tumor vaccines are of particular interest. In this study, a novel melanoma B16F10 CD133(+)CD44(+) cancer stem cell (CSC) vaccine expressing 6 kDa early secreted antigenic target (ESAT-6) in the glycosylphosphatidylinositol (GPI)-anchored form and secreting interleukin (IL)-21 was developed. Its anti-melanoma efficacy and mechanisms were investigated in mice. The results demonstrated that the B16F10-ESAT-6-gpi/IL-21 CD133(+)CD44(+) CSC vaccine exhibited enhanced anti-melanoma efficacy as determined by inhibited melanoma growth, prolonged survival of melanoma bearing mice. The anti-melanoma immunity was associated with elevated levels of serum anti-ESAT-6 and interferon (IFN)-γ as well as increased cytotoxic activities of natural killer cells, splenocytes, and complement dependent cytotoxicity. Furthermore, this CSC-based vaccine apparently inhibited melanoma lung metastasis by decreasing the level of Vimentin while increasing the level of E-cadherin expression, suggesting an inhibited epithelial mesenchymal transition. Thus, the B16F10-ESAT-6-gpi/IL-21 CD133(+)CD44(+) CSC vaccine may be used to reactivate the anti-tumor immunity and for treatment of melanoma.
The high-mobility group protein A2 (HMGA2) is an architectural transcription factor that plays a crucial role in the development and progression of various malignant cancers. However, the function of HMGA2 in bladder cancer remains largely unknown. Therefore, we aim to investigate the effect of HMGA2 on the proliferation, migration, invasion, and epithelial-mesenchymal transition (EMT) of bladder cancer cells. The expression of HMGA2 in human bladder cancer cells was downregulated by small interfering RNA (siRNA). The protein levels of HMGA2 and other related proteins were detected by Western blotting. The cell proliferation and apoptosis were examined by Cell Counting Kit-8 and flow cytometry, respectively. Transwell migration and invasion assays were performed to assess the effect of HMGA2 on the migration and invasion ability of cells. In conclusion, we found that HMGA2 knockdown markedly inhibited cell proliferation; this reduced cell growth was due to the high apoptosis rate of cells, as Bcl-xl was diminished, whereas Bax was upregulated. Moreover, our results showed that silencing of HMGA2 in cancer cells greatly inhibited the cell migration and invasion, decreased the expression of matrix metalloproteinase-2 (MMP-2) and matrix metalloproteinase-9 (MMP-9), and affected the occurrence of EMT. We further found that decreased HMGA2 expression suppressed the transforming growth factor-β (TGF-β)/Smad and Wnt/β-catenin signaling pathway in bladder cancer cells. These results revealed that HMGA2 played an important role in the progression of bladder cancer and might be a novel target for therapy in human bladder cancer.
Downregulation of E-cadherin by the transcriptional repressor Snail is associated with acquisition of metastatic potential. Although hepatitis C virus (HCV) core protein has been implicated in hepatocarcinogenesis, it is unclear whether Snail is involved in HCV core-induced dysregulation of E-cadherin. Herein, we investigated the mechanism by which HCV core induces E-cadherin repression and the role of Snail in HCV core-mediated invasiveness and metastasis. We found that HCV infection, especially HCV core expression, effectively induced the epithelial-mesenchymal transition (EMT) in hepatoma cells by repressing E-cadherin. HCV core interacted with Snail and enhanced its binding to the E-box in the promoter region of E-cadherin, leading to decreased E-cadherin promoter activity. We found that HCV core, Snail, and the histone deacetylases HDAC1/HDAC2 formed a co-repressor complex at the E-cadherin promoter. Moreover, HCV core was shown to stabilize Snail through activation of the PI3K/Akt/GSK3β pathway. Silencing Snail expression restored E-cadherin expression and inhibited HCV core-promoted tumor growth and distant lung metastasis in vivo. Collectively, these results demonstrated that HCV core induced EMT by interacting with the transcriptional repressor complex Snail/HDACs at the E-cadherin promoter, which led to E-cadherin repression and increased invasiveness of hepatoma cells. These findings increase understanding of factors regulating metastasis in hepatoma and may ultimately lead to the development of novel treatment strategies for HCV-associated hepatocellular carcinoma.
Cancer stem cells (CSCs) are a subpopulation of neoplastic cells with self-renewal capacity and limitless proliferative potential as well as high invasion and migration capacity. These cells are commonly associated with epithelial-mesenchymal transition (EMT), which is also critical for tumor metastasis. Recent studies illustrate a direct link between EMT and stemness of cancer cells. Long non-coding RNAs (lncRNAs) have emerged as important new players in the regulation of multiple cellular processes in various diseases. To date, the role of lncRNAs in EMT-associated CSC stemness acquisition and maintenance remains unclear. In this study, we discovered that a set of lncRNAs were dysregulated in Twist-positive mammosphere cells using lncRNA microarray analysis. Multiple lncRNAs-associated canonical signaling pathways were identified via bioinformatics analysis. Especially, the Shh-GLI1 pathway associated lncRNA-Hh, transcriptionally regulated by Twist, directly targets GAS1 to stimulate the activation of hedgehog signaling (Hh). The activated Hh increases GLI1 expression, and enhances the expression of SOX2 and OCT4 to play a regulatory role in CSC maintenance. Thus, the mammosphere-formation efficiency (MFE) and the self-renewal capacity in vitro, and oncogenicity in vivo in Twist-positive breast cancer cells are elevated. lncRNA-Hh silence in Twist-positive breast cells attenuates the activated Shh-GLI1 signaling and decreases the CSC-associated SOX and OCT4 levels, thus reduces the MFE and tumorigenesis of transplanted tumor. Our results reveal that lncRNAs function as an important regulator endowing Twist-induced EMT cells to gain the CSC-like stemness properties.
Epithelial-mesenchymal transition (EMT) occurs during adult tissue remodeling responses including carcinogenesis and fibrosis. Existing evidence reveals that hepatocytes can undergo EMT in adult liver, which is critically involved in chronic liver injury. We herein established a hypoxia-induced EMT model in human LO2 hepatocytes treated with cobalt chloride (CoCl2) in vitro, and evaluated the effects of curcumin, a natural antifibrotic compound, on hepatocyte EMT and explored the underlying molecular mechanisms. We found that CoCl2 at non-toxic doses induced a mesenchymal cell phenotype in hepatocytes and upregulated several mesenchymal markers including α-smooth muscle actin, vimentin, N-cadherin, fibronectin and Snail (an EMT-related transcription factor), but downregulated the epithelial marker E-cadherin in hepatocytes. However, curcumin reversed the morphological changes, abrogated the increased expression of mesenchymal markers, and rescued E-cadherin expression in CoCl2-treated hepatocytes, suggesting the inhibition of hepatocyte EMT in vitro. We further found that curcumin interfered with the transforming growth factor-β (TGF-β) signaling by reducing the expression of TGF-β receptor I and inhibiting the expression and phosphorylation of Smad2 and Smad3. Use of SB431542, a specific inhibitor of TGF-β receptor I, demonstrated that interference with the TGF-β/Smad pathway was associated with curcumin suppression of hepatocyte EMT. Our in vivo data showed that curcumin affected hepatic EMT in rat fibrotic liver caused by carbon tetrachloride, which was associated with the inhibition of TGF-β/Smad signaling. These findings characterized a novel mechanism by which curcumin modulated hepatocyte EMT implicated in treatment of liver fibrosis.
Breast cancer is the most common cause of death among women. KIF3C, a member of kinesin superfamily, functions as a motor protein involved in axonal transport in neuronal cells. To explore the expression, regulation and mechanism of KIF3C in breast cancer, 4 breast cancer cell lines and 93 cases of primary breast cancer and paired adjacent tissues were examined. Immunohistochemistry, Real Time Polymerase Chain Reaction (RT-PCR), Western blot, flow cytometry, short hairpin RNA (shRNA) interference, 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT), colony formation techniques and xenograft mice model were used. We found that KIF3C was over-expressed in breast cancer tissues and such high KIF3C expression was also associated with tumor recurrence and lymph node metastasis. Silencing of KIF3C by shRNA inhibited epithelial-mesenchymal transition and metastasis by inhibiting TGF-β signaling and suppressed breast cancer cell proliferation through inducing G2/M phase arrest. The tumor size was smaller and the number of lung metastatic nodules was less in KIF3C depletion MDA-MB-231 cell xenograft mice than in negative control group. These results suggested that high expression of KIF3C in breast cancer may be associated with the tumor progression and metastasis.
The contribution of Ca(2+) in TGF-β-induced EMT is poorly understood. We aimed to confirm the effect of TGF-β on the gene expression of intracellular calcium-handling proteins and to investigate the potential underlying mechanisms in TGF-β-induced EMT. T47D and MCF-7 cells were cultured in vitro and treated with TGF-β. The mRNA expression of EMT marker genes and intracellular calcium-handling proteins were quantified by qRT-PCR. qRT-PCR and Western blot analysis results verified the changes of EMT marker gene expression. Furthermore, we found that TGF-β induced cell morphological changes significantly with an increase of cell surface area and cell length. These results indicated that TGF-β induced EMT. The mRNA expression levels of SPCA1, SPCA2 and MCU were not influenced by TGF-β treatment, while NCX1 expression was decreased in T47D cells. In addition, the mRNA levels of SERCAs and IP3Rs were significantly changed due to TGF-β-induced EMT. The TGF-β-treated T47D cells exhibited markedly greater response to ATP than the control cells, and the descent velocity of cytosolic calcium concentration was faster in TGF-β-treated cells than in control cells. This is the first report to demonstrate that TGF-β-induced EMT in human breast cancer cells is associated with alterations in endoplasmic reticulum calcium homeostasis.
Recent studies reveal that chemotherapy can enhance metastasis due to host responses, such as augmented expression of adhesion molecules in endothelial cells and increased populations of myeloid cells. However, it is still unclear how tumour cells contribute to this process. Here, we observed that paclitaxel and carboplatin accelerated lung metastasis in tumour-bearing mice, while doxorubicin and fluorouracil did not. Mechanistically, paclitaxel and carboplatin induced similar changes in cytokine and angiogenic factors. Increased levels of CXCR2, CXCR4, S1P/S1PR1, PlGF and PDGF-BB were identified in the serum or primary tumour tissues of tumour-bearing mice treated by paclitaxel. The serum levels of CXCL1 and PDGF-BB and the tissue level of CXCR4 were also elevated by carboplatin. On the other hand, doxorubicin and fluorouracil did not induce such changes. The chemotherapy-induced cytokine and angiogenic factor changes were also confirmed in gene expression datasets from human patients following chemotherapy treatment. These chemotherapy-enhanced cytokines and angiogenic factors further induced angiogenesis, destabilized vascular integrity, recruited BMDCs to metastatic organs and mediated the proliferation, migration and epithelial-to-mesenchymal transition of tumour cells. Interestingly, inhibitors of these factors counteracted chemotherapy-enhanced metastasis in both tumour-bearing mice and normal mice injected intravenously with B16F10-GFP cells. In particular, blockade of the SDF-1α-CXCR4 or S1P-S1PR1 axes not only compromised chemotherapy-induced metastasis but also prolonged the median survival time by 33.9% and 40.3%, respectively. The current study delineates the mechanism of chemotherapy-induced metastasis and provides novel therapeutic strategies to counterbalance pro-metastatic effects of chemo-drugs via combination treatment with anti-cytokine/anti-angiogenic therapy.
Glucose-regulated protein of 78kD (GRP78) is a multifunctional protein belonging to the heat shock protein 70 family. Overexpression of GRP78 triggered by environmental and physiological stresses is positively correlated with the occurrence and progression of various tumors, but the molecular mechanisms have not been well established. The present study indicated that overexpression of GRP78 in colon cancer cells could promote cell-matrix adhesion through the upregulation of fibronectin, integrin-β1 and phosphorylated FAK. Meanwhile, it resulted in a visible epithelial-mesenchymal transition in DLD1 cells, and the Snail-2 played the key role during the process. More importantly, the data indicated that GRP78 overexpression facilitated the expression and secretion of TGF-β1, which further activated the downstream Smad2/3 signaling module to effectuate the cell-matrix adhesion and epithelial-mesenchymal transition. Taken together, this study provides a novel molecular mechanism involving in the effects of GRP78 on colon cancer metastasis.
TGF-β1 secreted abundantly by tumors cells as well as present in the local microenvironment promotes neoplasm invasion and metastasis by triggering the epithelial to mesenchymal transition (EMT). MiR200c has been shown to suppress EMT and to regulate the cellular epithelial and interstitial state conversion, whereas the tumor vaccines are intended to specifically initiate or amplify a host response against evolving tumor cells. Our study aimed at optimizing the antitumor effects of the B16F10/glycosylphosphatidylinositol-interleukin 21 (B16F10/GPI-IL-21) tumor vaccine on melanoma bearing mice by combining the TGF-β1 knockdown and the administration of miR200c agomir. The mice were subcutaneously vaccinated with inactivated B16F10/GPI-IL-21 vaccine and challenged by B16F10 cells transfected with shTGF-β1 (B16F10/shTGF-β1 cells) or B16F10/shTGF-β1 cells with the administration of miR200c agomir. The later combination showed that, when compared with the mice in the control group that received no vaccination, vaccinated mice significantly increased NK and CTL activities, enhanced levels of IFN-γ, and reduced expression of TGF-β1, N-cadherin, Vimentin, Gli1/2, P-Smad2/3 and others involved in promoting expression of EMT-related molecules in tumor areas, and inhibited the melanoma metastasis in lungs and lymph nodes. Altogether, our findings demonstrate that this synergistic anti-cancer regimen effectively induces strong immune response and diminishes the melanoma progression.
Malic enzyme 1 (ME1) links the glycolytic and citric acid cycles and is important for NADPH production, glutamine metabolism, and lipogenesis. Recently, its deregulation has been implicated in the progression of various cancers. However, the role of ME1 in the progression of hepatocellular carcinoma (HCC) remains unclear. In this study, we utilized short hairpin RNA-mediated gene silencing to investigate the biological effects of ME1 depletion in HCC and determined its prognostic significance in HCC. ME1 expression was examined by real-time (RT)-PCR and Western blot using five HCC cell lines and one normal liver cell line. We used polyethylenimine nanoparticles to deliver a short hairpin RNA to induce cessation of ME1 expression in HCC cells. Changes in NADPH production and reactive oxygen species (ROS) production were studied. Metastatic potentials of HCC cells were evaluated in vitro. Furthermore, we evaluated the protein level of ME1 in para-tumor and cancerous tissues of 65 HCC patients with detailed clinical, pathological, and clinical follow-up data. Patients' survivals were further assessed as well. Upregulated ME1 expression was observed in HCC cell lines. Downregulation of ME1 attenuated NADPH production and stimulated ROS production. Silencing ME1 was noted to inhibit migratory and invasive properties of HCC cells by inducing the E-cadherin expression and decreasing of N-cadherin and vimentin expression in a ROS-dependent pathway. Overexpression of ME1 was observed in a major fraction of HCC samples. Higher level of ME1 in tumors was significantly associated with reduced overall survival (Kaplan-Meier analysis, P = 0.024) and reduced progression-free survival (Kaplan-Meier analysis, P = 0.011). Inhibition of ME1 expression decreases HCC metastasis via suppression of epithelial-mesenchymal transition (EMT) processes in ROS-induced pathways. ME1 overexpression associates with unfavorable prognoses in patients with HCC, suggesting that ME1 is a poor prognostic predictor of hepatocellular carcinoma.
Hairy enhancer of split-1 (HES1) is a transcriptional target of the Notch pathway, and a high level of HES1 is regarded as a marker of activated Notch. The aim of the study was to investigate the role of HES1 in colorectal cancer progression. We used tissue microarrays to analyze the expression and clinical significance of HES1 in 320 colorectal cancer samples. Stable overexpression and knockdown of HES1 were established in three colorectal cancer cell (CRC) lines (RKO, HCT8 and LOVO). We investigated the differentially expressed genes and enriched pathways in HES1 overexpressing CRC cells by gene expression profiling. Also, the role of HES1 in invasion and migration were examined in vitro and in vivo. We found that high expression of HES1 was significantly correlated with distal metastasis (P = 0.037) at diagnosis, and HES1 could serve as an unfavorable prognostic factor for colorectal cancer patients (P = 0.034). Gene expression profiling and pathway enrichment analysis revealed that HES1 was related to cellular adherens junction loss. In addition, we showed that HES1 overexpression lead to depressed E-cadherin, and elevated N-cadherin, vimentin and Twist-1 levels. Functionally, HES1 enhanced invasiveness and metastasis of CRC cells. HES1 promotes cancer metastasis via inducing epithelial mesenchymal transition and serves as a poor prognosis factor of colorectal cancer patients.
Human leukocyte antigen class I antigens (HLA-I) is essential in immune response by presenting antigenic peptides to cytotoxic T lymphocytes. Downregulation of HLA-I is observed in primary and metastatic prostate cancers, which facilitates them escape from immune surveillance, thereby promotes prostate cancer progression. In addition, elevated level of growth factors like TGF-β or EGF in microenvironment is related to the prostate cancer deterioration. Thus, we wondered whether TGF-β or EGF was involved in the regulation of HLA-I during the development of prostate cancer cells. In this study, we demonstrated that TGF-β and EGF both downregulated the expression of HLA-I, thereby attenuated the cytotoxic T cell mediated lysis of prostate cancer cells. Next, we revealed that TGF-β and EGF induced downregulation of HLA-I is associated with classical epithelial-mesenchymal transition (EMT) morphological changes and expression profiles. We further illustrated that overexpression of Snail is crucial for HLA-I downregulation and its association with EMT. At last, we discussed that NF-κB/p65 is the plausible target for Snail to induce HLA-I downregulation. Taken together, this is the first evidence to reveal that both TGF-β and EGF can induce HLA-I downregulation which is then proven to be associated with EMT in prostate cancer cells. These discoveries provide a deeper understanding of growth factors induced immune escape and introduce potential therapeutic targets for prostate cancers.
HER2 receptor dimerization is a critical step in the HER2 activation process. Here, we demonstrated that heat shock protein gp96 on cell membrane interacts with HER2, facilitates HER2 dimerization and promotes cell proliferation. Cell membrane gp96 levels were observed to correlate with HER2 phosphorylation in primary breast tumors. Finally, we provide evidence that targeting gp96 with a specific monoclonal antibody led to decreased cell growth and increased apoptosis in vitro, and suppression of tumor growth in vivo. Our work represents a new therapeutic strategy for inhibiting HER2 signaling in cancer.
Metastasis is the major cause of death in colorectal cancer (CRC). Although multiple genes have been identified to be responsible for the development of CRC, the molecular changes that enable CRC cells to undergo early local invasion and to form distant metastatic colonies still remain largely unknown. Herein, we investigated the role of Forkhead box protein C2 (FOXC2) and explored the underlying mechanisms in invasion and metastasis of CRC. We show that both high FOXC2 expression and nuclear localization of FOXC2 are significantly correlated with advanced TNM (T=primary tumor; N=regional lymph nodes; M=distant metastasis) stages. FOXC2 enhanced the invasive abilities of CRC cells in vitro and promoted local invasion and distant metastasis in an orthotopic mouse metastatic model of CRC. Microarray analysis revealed that overexpression of FOXC2 increased the proto-oncogene MET tyrosine kinase expression and activated the hepatocyte growth factor (HGF)-MET signaling pathway. Furthermore, luciferase reporter assays and chromatin immunoprecipitation assays revealed that FOXC2 directly associated with MET promoter to increase the transcriptional activity of MET. Inhibition of MET attenuates the invasive phenotype and metastatic potential of FOXC2-overexpressing CRC cells, indicating that MET is a major mediator of FOXC2-promoted metastasis. In addition, FOXC2 expression was positively correlated with MET expression in CRC tissue samples. Our findings suggest that FOXC2 has a crucial role in CRC metastasis by regulating HGF-MET signaling via inducing MET expression, highlighting FOXC2 as a potential therapeutic target for preventing or reducing metastasis in CRC.
In the brain, astrocytes play an essential role with their multiple functions and sophisticated structure, as surrounded by a fractal environment which has not been available in our traditional cell culture. Water-repellent fractal tripalmitin (PPP) surfaces can imitate the fractal environment in vivo, so the morphology and biochemical characterization of astrocytes on these surfaces are examined. Water-repellent fractal PPP surface can induce astrocytes to display sophisticated morphology with smaller size of cell area, longer and finer filopodium-like processes, and higher morphological complexity. The super water-repellent fractal PPP surface with water contact angle of 150°∼160° produces the maximal effects compared with other surfaces at lower water contact angles. The trends of characteristic protein expression, including that of nestin, vimentin, GFAP and glutamine synthetase, for astrocytes cultured on super water-repellent fractal PPP surfaces approximate more to in vivo pattern. The super water-repellent PPP surface also render astrocytes to perform more pronounced promotion of neurogenesis by increasing the release of nerve growth factor in a co-culture system. Altogether, our results suggest that the super water-repellent fractal PPP surface facilitates the astrocytes to mimic their in vivo performance, thus provides a closer-to-natural culture environment for experimental assessment of glial structure and functions.
The membrane protein tyrosine phosphatase receptor U (PTPRU) has been shown to function as a negative regulator of adhesion and proliferation in certain cancer cell types, primarily through its dephosphorylation of β-catenin and inhibition of subsequent downstream signaling. In the present study, we set out to characterize the role of PTPRU in glioma and found that, while the expression of full-length PTPRU protein is low in these tumors, a number of non-full-length PTPRU isoforms are highly expressed. Among these isoforms, one in particular is localized to the nucleus, and its expression is increased in glioma tissues in a manner that positively correlates with malignancy grade. Short hairpin RNA knockdown of endogenous PTPRU in human and rat glioma cell lines suppressed proliferation, survival, invasion, migration, adhesion and vasculogenic tube formation in vitro, as well as intracranial tumor progression in vivo. In addition, knocking down PTPRU reduced tyrosine phosphorylation (pY) and transcriptional activity of β-catenin, and we were able to specifically rescue the cell migration defect by expressing a LEF1-β-catenin fusion protein in PTPRU-depleted cells. PTPRU knockdown also led to increased tyrosine pY of the E3 ubiquitin ligase c-Cbl and to the destabilization of several focal adhesion proteins. Taken together, our findings demonstrate that endogenous PTPRU promote glioma progression through their effect on β-catenin and focal adhesion signaling.
Accumulating evidences implicate that ribonuclease inhibitor (RI) plays a suppressing role in cancer development. However, the mechanisms underlying antitumor of RI remain largely unknown. Epithelial-mesenchymal transition (EMT) is regarded as a key event in tumor progression. The reports have demonstrated that EMT was implicated in metastasis of bladder cancer. Therefore, we suppose that RI might involve regulating EMT of bladder cancer. Here bladder cancer T24 cells were transfected with pGensil-1-siRNA-RI vectors. HE staining, living cell observation, Phalloidine-FITC staining of microfilament, cell adhesion, scratch migration, and Matrigel invasion were examined respectively. RI expression and colocalization with ILK were detected using confocal microscope. Proteins associated with EMT were determined with Western blotting and immunohistochemistry in vivo and in vitro. Effects of RI expression on tumor growth, metastasis and EMT related proteins in BALB/C nude mouse and clinical human bladder cancer specimens were valued with histological, immunohistochemical and immunofluorescent examination respectively. We demonstrated that down-regulating RI increased cell proliferation, migration and invasion, changed cell morphology and adhesion, and rearranged cytoskeleton by inducing EMT and ILK signaling pathway in bladder cancer cells. In addition, we showed that down-regulating RI promoted tumorigenesis and metastasis of bladder cancer in vivo. Finally, we found that bladder cancer with invasive capability had higher Vimentin, Snail, Slug and Twist as well as lower E-cadherin and RI expression in clinical human specimens. Our results suggest that RI could play a novel role in inhibiting metastasis of bladder through regulating EMT and ILK signaling pathway.
Understanding the mechanisms of colorectal cancer (CRC) metastatic progression is essential to reducing its morbidity and mortality. Pyruvate kinase (PK) catalyses the final step of glycolysis and has been identified as a critical regulator of glucose consumption. However, the mechanisms and roles of PKM1 and PKM2 in the regulation of CRC cell migration and cell adhesion remain elusive. Here, we report that PKM2 rather than PKM1 drives CRC cell migration and cell adhesion, whereas PKM attenuation reverses these phenomena. Furthermore, the overexpression of PKM2 significantly increases the expression of N-cadherin, MMP-2, MMP-9, STAT3, Snail-2, pFAK and active β1-integrin, while E-cadherin expression is suppressed. More importantly, the results indicated that PKM2 overexpression facilitates STAT3 nuclear translocation, and it is required for PKM2 function in the regulation of migration and adhesion associated signalling. In addition, the dimeric form of PKM2, which lacks the pyruvate kinase activities but possesses protein kinase activity, is critical for CRC cell migration and cell adhesion. Overall, this study suggests that PKM2 overexpression promotes CRC cell migration and cell adhesion by regulating STAT3-associated signalling and that PKM2 may serve as a therapeutic target for CRC metastasis.
Expression of epithelial-mesenchymal transition (EMT) markers has been detected clinically in benign prostatic hyperplasia (BPH) tissues. To understand the molecular basis, we investigated the role of stromal microenvironment in the progression of EMT in BPH cells. First, we used cell culture supernatant from normal prostate stromal WPMY-1 cells to provide supernatant-conditioned medium (WSCM) to culture the BPH-1 cell line. Then, the morphological changes and migratory capacity were detected in BPH-1 cells. The expression of EMT markers was examined in BPH-1 cells by Western blot and immunofluorescent analysis. Finally, to investigate the role of transforming growth factor beta 1 (TGF-β1) in this process, the WSCM-cultured cells were treated with monoclonal antibody against TGF-β1 to study its effect on EMT. We found that the morphology of BPH-1 cells changed to a spindle-like shape after cultured in WSCM, and the levels of E-cadherin and cytokeratin 5/8 (CK5/8) were significantly lower than the cells cultured in ordinary medium. These BPH-1 cells were also tested positive for mesenchymal markers vimentin and a-smooth muscle actin (SMA) as well as Snail. We also found WSCM can increase the migratory capacity of BPH-1 cells. In addition, when they were treated with anti-TGF-β1, upregulation of E-cadherin and CK5/8 levels was observed but no expression of vimentin, alpha-SMA or Snail was detected. Furthermore, phosphorylated-Smad3 expression in WSCM-cultured BPH-1 cells was also suppressed by anti-TGF-β1 treatment. Our results demonstrated that stromal cell supernatant was able to induce EMT in BPH-1 cells, possibly through secreting TGF-β1 to activate Smad signaling. Our results suggest novel molecular targets for clinical treatment of BPH by modification of stromal microenvironment through inhibiting TGF-β1/Smad expression.
Tumor invasion and migration obstructs the treatment and prognosis of cancer. In this research, we investigated the effect of oroxylin A, a natural compound extracted from Scutellaria radix, the root of Scutellaria baicalensis, on inhibition of the invasion and migration of three different tumor cell lines: MCF-7, DU145, and HepG2. The results suggested that oroxylin A could inhibit hypoxia-induced migration and invasion of the three cell lines mentioned above. To study the detailed mechanisms, studies were carried out on MCF-7 cells and it was found that oroxylin A could regulate the expression of related markers in MCF-7 cells including E-cadherin, N-cadherin, and Vimentin. It was also found that oroxylin A inhibited the hypoxia-induced invasion and migration of MCF-7 cells by suppressing the Notch pathway. Oroxylin A inhibited N1ICD translocating to the nucleus and binding to epithelial-mesenchymal transition-related transcription factor Snail, thus suppressing the invasion and migration of MCF-7 cells. Therefore, oroxylin A is expected to be a promising candidate for antimetastasis treatment through suppression of the hypoxia-induced Notch pathway.
Zinc-finger E-box binding homeobox 1 (ZEB1) is a master regulator of epithelial-mesenchymal transition (EMT) and has been implicated in primary epithelial cancer biological processes, such as invasion and metastasis. However, the role of ZEB1 in progression of melanoma and cancer stem cells (CSCs) remains obscure. In this study, the recombinant plasmids of t3 shRNAs targeting mouse ZEB1 were constructed and transfected into melanoma B16F10 cells. The stable transfected cells were selected and the characteristics of ZEB1 downregulated B16F10 cells was assessed. The tumourigenicity of CD44(+) CD133(+) CSCs isolated from B16F10 cells stably transfected with the ZEB1-shRNA2 recombinant was also assessed. ZEB1-shRNAs B16F10 showed a lower expression of ZEB1 and vimentin, weaker migration, invasiveness, colony forming, and proliferation, and a lower tumourigenicity than the control cells. The tumourigenicity of the ZEB1-shRNA2 CD44(+) CD133(+) CSCs was also inhibited. In conclusion, ZEB1-shRNA2-mediated downregulation of ZEB1 expression in B16F10 cells and CSCs is involved in the inhibition of the EMT process. ZEB1 may be a potential target in melanoma targeted.
The epithelial-to-mesenchymal transient (EMT) is associated with tumor metastasis. Twist is one of the key transcription factors for EMT and relates to tumor cell migration. Long non-coding RNAs (lncRNAs) have recently emerged as important regulatory molecules involved in a broad range of biological processes and complicated diseases. However, it is unknown whether a signal network and lncRNAs are involved in Twist-induced EMT program. Taking MCF10A/Twist as a model, more than 99 lncRNAs and 3164 genes are regulated in the Twist-induced EMT process using lncRNA-array and cDNA micro-array. We establish a downstream signal network associated with EMT induced by Twist using bioinformatic analysis (Gene Ontology, pathway analysis) and experimental data. A set of multiple canonical signal pathways (such as WNT, MAPK, JAK/STAT, TGF-β, mTOR, Hedgehog and P53 signaling pathways) and several lncRNAs [such as lncRNA (chr6, 26124411-26139312, +), lncRNA (chr1, 41944445-41949874, -), lncRNA (chr17, 44833874-44834830, +)] are altered in MCF10A/Twist cells. More interestingly, lncRNA (chr17, 44833874-44834830, +), lncRNA (chr17, 21142183-21156578, -), lncRNA (chr6, 26124411-26139312, +) and lncRNA (chr19, 438420-2083745, -) may be involved in regulation or activation of WNT signaling pathway in the Twist-induced EMT process. These findings first determine that Twist contributes to invasion and metastasis by inducing wide-ranging transcriptional and functional changes of lncRNAs and signal pathways in our study.
MicroRNAs (miRNAs) have been believed to associate with malignant progression including cancer cell proliferation, apoptosis, differentiation, angiogenesis, invasion and metastasis. However, the functions of miRNAs are intricate, one miRNA can directly or indirectly target multiple genes and function as oncogene or tumor suppressor gene. In this study, we found that miR-21 inhibits PTEN and human sulfatase-1 (hSulf-1) expression in hepatocellular carcinoma (HCC) cells. The hSulf-1 is a heparin-degrading endosulfatase, which can inhibit the heparin binding growth factor-mediated signaling transduction into cells. Therefore, miR-21-mediated suppression of both hSulf-1 and PTEN led to activation of AKT/ERK pathways and epithelial-mesenchymal transition (EMT) in HCC cells, and finally enhance the activity of HCC cell proliferation and movement and promote HCC xenograft tumor growth in mouse models. These findings may provide candidate targets for prevention and treatment of HCC.
Integrin-linked kinase (ILK) is a multifunctional serine/threonine kinase in cytoplasm. Recent studies showed that cancer patients with increased ILK expression had low survival, poor prognosis and increased metastasis. Although the causes of ILK overexpression remain to be fully elucidated, accumulating evidence suggests that its oncogenic capacity derives from its regulation of several downstream targets that provide cells with signals that promote proliferation, survival and migration. However, the mechanisms underlying tumor metastasis by ILK is still not fully understood. Epithelial–mesenchymal transition (EMT) is a critical event of cancer cells that triggers invasion and metastasis. We recently reported that knockdown of ILK inhibited the growth and induced apoptosis in human bladder cancer cells. Therefore, we postulate that ILK might involve in EMT. Here we further investigate the function of ILK with RNA interference in bladder cancer cells. Knockdown of ILK impeded an EMT with low Vimentin, Snail, Slug and Twist as well as high E-cadherin expression in vivo and vitro. In addition, we found that knockdown of ILK inhibited cell proliferation, migration and invasion as well as changed cell morphology, adhesion and rearranged cytoskeleton in vitro. We also demonstrated that ILK siRNA inhibited phosphorylation of downstream signaling targets Akt and GSK3β, increased expression of nm23-H1, as well as reduced expression of MMP-2 and MMP-9 in vivo and vitro. Furthermore, downregulation of ILK could increase expression of Ribonuclease inhibitor (RI), an important acidic cytoplasmic protein with many functions. Finally, the effects of ILK siRNA on bladder cancer cell phenotype and invasiveness translate into suppression for tumorigenesis and metastasis in vivo. Taken together, our findings highlight that ILK signaling pathway plays a novel role in the development of bladder cancer through regulating EMT. ILK could be a promising diagnostic marker and therapeutic target for bladder cancer.
Hypoxia-induced epithelial mesenchymal transition (EMT) is an essential step in cancer metastasis. Luteolin, a flavonoid that is widely distributed in plants, is a novel anticancer agent. However, the mechanism underlying its anticancer effects remains undefined. In this study, for the first time, we demonstrate that luteolin inhibits hypoxia-induced EMT in human non-small cell lung cancer cells in culture, which is demonstrated by the fact that hypoxia-induced EMT reduced the expression of E-cadherin and other epithelial markers and increased the expression of N-cadherin, vimentin and other mesenchymal markers; these effects were markedly attenuated by luteolin. In addition, luteolin also inhibited hypoxia-induced proliferation, motility and adhesion in the cells. Furthermore, we reveal that luteolin inhibits the expression of integrin β1 and focal adhesion kinase (FAK).Since integrin β1 and FAK signaling are closely related to EMT formation, these results suggest that luteolin inhibits hypoxia-induced EMT, at least in part, by inhibiting the expression of integrin β1 and FAK.
Human ribonuclease inhibitor (RI) is a cytoplasmic acidic protein. RI is constructed almost entirely of leucine rich repeats, which might be involved in unknown biological effects except inhibiting RNase A and angiogenin activities. We previously reported that up-regulating RI inhibited the growth and metastasis of melanoma cells. Epithelial-mesenchymal transition (EMT) is a critical event of cancer cells that triggers invasion and metastasis. However, the role of RI in the EMT process remains unknown. Here we hypothesize that RI might inhibit melanoma invasion and metastasis by regulating EMT. We found that over-expression of RI induced up-regulation of E-cadherin, accompanied with decreased expressions of proteins associated with EMT such as N-cadherin, Snail, Slug, Vimentin and Twist both in vitro and in vivo. Furthermore, RI restrained matrix metalloproteinase MMP-2 and MMP-9 secretions in B16 and B16-F10 melanoma cells. In addition, we also found that up-regulation of RI inhibited cell proliferation, migration and invasion as well as changed cell morphology, adhesion and rearranged cytoskeleton in vitro. Finally, the effects of RI on phenotype and invasiveness translated into suppressing metastasis by the experimental metastasis models of melanoma with lighter lung weight, a fewer metastasis nodules and a lower incidence rate, with respect to the control groups. Taken together, our data highlight, for the first time, that RI plays a novel role in inhibiting development and progression of murine melanoma cells through regulating EMT. These results suggest that RI could be a therapeutic target protein for melanoma and may be of biological importance.
BACKGROUND:
The gastric dramatic down-related gene (GDDR) is an abundantly expressed secretory protein in normal gastric epithelia, while its expression is distinctly decreased in gastric cancer. However, the role of GDDR in gastric cancer remains poorly understood.
AIMS:
This study aims to detect the expression and clinical significance of GDDR in gastric cancer and investigate its effects on epithelial-mesenchymal transition.
METHODS:
The expression of GDDR in gastric cancer was examined by immunohistochemistry, immunoblotting, and Western blotting. The relationships between GDDR expression and clinicopathological factors were evaluated. The effects of GDDR on epithelial-mesenchymal transition of gastric cancer cells were investigated in vitro.
RESULTS:
GDDR was absent in gastric cancer tissue or dramatically downregulated in gastric cancer cell lines. Loss of GDDR expression in gastric cancer was strongly correlated with clinicopathological factors, such as tumor differentiation (p = 0.037), T stage (p < 0.001), lymph node metastasis (p = 0.008) and TNM stage (p < 0.001). Patients with decreased GDDR expression presented shortened overall survival (p = 0.033). Functional studies demonstrated that GDDR elevation augmented cell-cell adhesion and suppressed cell motility, concomitant with increased expression of E-cadherin and decreased expression of β-catenin and vimentin. Conversely, GDDR depletion increased cell motility, concomitant with decreased expression of E-cadherin and increased expression of β-catenin and vimentin. Moreover, GDDR had an inhibitory effect on PI3K/Akt signaling pathway.
CONCLUSIONS:
Our findings suggested that GDDR expression was significantly associated with the progression of gastric cancer and GDDR may function as a tumor suppressor via inhibiting the epithelial-mesenchymal transition.
PURPOSE:
This study was designed to investigate the role of PDGF-DD secreted by gastric cancer-derived mesenchymal stem cells (GC-MSCs) in human gastric cancer progression.
METHODS:
Gastric cancer cells were indirectly co-cultured with GC-MSCs in a transwell system. The growth and migration of gastric cancer cells were evaluated by cell colony formation assay and transwell migration assay, respectively. The production of PDGF-DD in GC-MSCs was determined by using Luminex and ELISA. Neutralization of PDGFR-β by su16f and siRNA interference of PDGF-DD in GC-MSCs was used to demonstrate the role of PDGF-DD produced by GC-MSCs in gastric cancer progression.
RESULTS:
GC-MSC conditioned medium promoted gastric cancer cell proliferation and migration in vitro and in vivo. Co-culture with GC-MSCs increased the phosphorylation of PDGFR-β in SGC-7901 cells. Neutralization of PDGFR-β by su16f blocked the promoting role of GC-MSC conditioned medium in gastric cancer cell proliferation and migration. Recombinant PDGF-DD duplicated the effects of GC-MSC conditioned medium on gastric cancer cells. Knockdown of PDGF-DD in GC-MSCs abolished its effects on gastric cancer cells in vitro and in vivo.
CONCLUSIONS:
PDGF-DD secreted by GC-MSCs is capable of promoting gastric cancer cell progression in vitro and in vivo. Targeting the PDGF-DD/PDGFR-β interaction between MSCs and gastric cancer cells may represent a novel strategy for gastric cancer therapy.
BACKGROUND:
Genetically modified cells have been shown to be one of the most effective tumor vaccine strategies. However, in many cases, such as in melanoma, induction of a potent immune responses against the disease still remains a major challenge. Thus, novel strategies to reinforce tumor vaccine efficacy are needed. Using microRNA (miR) and Zinc-finger E-box binding homeobox (ZEB) have received much attention for potentially regulating tumor progression. To elicit a potent antitumor efficacy against melanoma, we used tumor vaccine in combination with miR200c overexpression or ZEB1 knockdown to assess the efficacy of treatment of murine melanoma.
METHODS:
B16F10 cell vaccine expressing interleukin 21 (IL-21) in the glycosylpho- sphatidylinositol (GPI)-anchored form (B16F10/GPI-IL-21) were developed. The vaccine was immunized into mice challenged by B16F10 cells or B16F10 cells stably transduced with lentiviral-miR200c (B16F10/miR200c) or transfected with the ZEB1-shRNA recombinant (B16F10/shZEB1) or the B16F10/GPI-IL-21 vaccine. The immune responses, tumorigenicity and lung metastasis in mice were evaluated, respectively.
RESULTS:
The vaccination with B16F10/GPI-IL-21 markedly increased the serum cytokine levels of IFN-γ, TNF-α, IL-4 and decreased TGF-β level as well as augmented the cytotoxicity of splenocytes in immunized mice compared with control mice. In addition, the tumor vaccine B16F10/GPI-IL-21 significantly inhibited the tumor growth and reduced counts of lung metastases in mice challenged by B16F10/GPI-IL-21, B16F10/shZEB1 and B16F10/miR200c respectively compared with the control mice challenged by B16F10 cells. The efficacy mechanisms may involve in reinforcing immune responses, increasing expression of miR200c, E-cadherin and SMAD-7 and decreasing expression of TGF-β, ZEB1, Vimentin and N-cadherin in tumor tissues from the immunized mice.
CONCLUSIONS:
These results indicate that the tumor vaccine B16F10/GPI-IL-21 in combination with miR200c overexpression or ZEB1 knockdown effectively inhibited melanoma growth and metastasis a murine model. Such a strategy may, therefore, be used for the clinical trials.
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/1937R] - BSA and Azide free (A253494) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253494_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/1937R] (A250314) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250314_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [V9] (A250310) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250310_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [ARC0086] (A305554) - Antibodies.com](https://cdn.antibodies.com/image/catalog/305/A305554_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [VM452] - BSA and Azide free (A253487) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253487_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [VM452] (A250307) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250307_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [V9] - BSA and Azide free (A253490) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253490_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/6576R] (A250313) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250313_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [rVIM/6575] - BSA and Azide free (A253486) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253486_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/6576R] - BSA and Azide free (A253493) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253493_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [rVIM/6575] (A250306) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250306_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/1937R] - BSA and Azide free (A253494) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253494_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/1937R] (A250314) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250314_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [V9] (A250310) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250310_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [ARC0086] (A305554) - Antibodies.com](https://cdn.antibodies.com/image/catalog/305/A305554_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [VM452] - BSA and Azide free (A253487) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253487_1.jpg?profile=product_alternative)
![Western Blot - Anti-Vimentin Antibody [VM452] (A250307) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250307_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [V9] - BSA and Azide free (A253490) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253490_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/6576R] (A250313) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250313_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [rVIM/6575] - BSA and Azide free (A253486) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253486_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [VIM/6576R] - BSA and Azide free (A253493) - Antibodies.com](https://cdn.antibodies.com/image/catalog/253/A253493_1.jpg?profile=product_alternative)
![Immunohistochemistry - Anti-Vimentin Antibody [rVIM/6575] (A250306) - Antibodies.com](https://cdn.antibodies.com/image/catalog/250/A250306_1.jpg?profile=product_alternative)








